“By 30 months, 40 percent of patients were determined to have suffered at least one episode of this type of abnormal rhythm (A-fib)…”
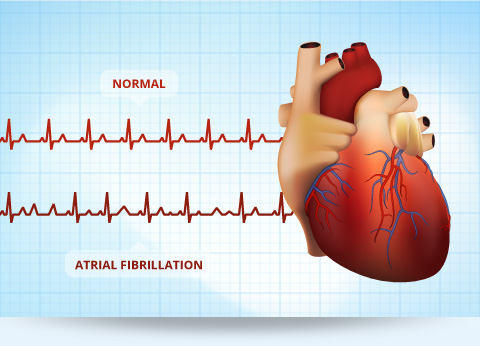
If you take away only two pieces of information from this post, let them be 1) studies show more than 40% of seniors experience A-Fib occasionally increasing their risk of stroke and 2) prescription blood thinners like eliquis and pradaxa cause a host of negative side effects.
I’m not a board-certified medical doctor so I can’t prescribe medicine. I am a cancer survivor who underwent a host of cardio-toxic chemotherapy regimens that resulted in chemotherapy-induced atrial fibrillation.
I took coumadin for about a year because my board-certified medical doctor told me that this was the “standard-of-care.” Coumadin made me tired and gain weight.
So I decided to stop taking coumadin. The issue I had to deal with is 1) how afib made me feel and 2) my increased risk of stroke. I have long since gotten used to feeling out-of-breath. So the main issue is increased risk of stroke.
I reduce my risk of stroke with evidence-based non-toxic therapies such as
- daily moderate exercise
- hydration
- magnesium
- omega 3 fatty acids,
- green tea extract.
These non-toxic, natural supplements also prevent cancer and are heart and brain healthy.
I have lived with chronic atrial fibrillation since 2010. I reduce my risk of stroke with Life Extension Super Omega 3 and Life Extension Super Green Tea Extract.
I am both a cancer survivor and cancer coach. To learn more about managing your health through evidence-based, non-toxic therapies please scroll down the page, post a question or comment and I will reply to you ASAP.
Thank you,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
‘A-fib’ heart problem more common than thought, doctor finds
“Several million older Americans have been diagnosed with atrial fibrillation, the abnormal heart rhythm abbreviated as A-fib, because they experienced symptoms such as palpitations, dizziness, and shortness of breath…
Yet many others may have the heart condition without realizing it, raising their risk of stroke,..
Kowey and his coauthors monitored 385 older patients who were at risk of A-fib because of diabetes, high blood pressure, and other telltale indicators but who had not been diagnosed with the rhythm disorder…
The longer the patients were followed, the more they experienced at least one episode of A-fib lasting six minutes or more, the authors reported in the journal JAMA Cardiology…
Six months into the study, 20.4 percent of patients were found to have A-fib. After one year, that figure rose to 27.1 percent. By 30 months, 40 percent of patients were determined to have suffered at least one episode of this type of abnormal rhythm.
According to the U.S. Centers for Disease Control and Prevention, 9 percent of people age 65 and up have been diagnosed with atrial fibrillation…
Patients with atrial fibrillation are typically counseled to take blood-thinning medications called anticoagulants. That is because during an episode of A-fib, the patient’s blood may stagnate and form a dangerous clot, leading to a stroke.
Yet strokes can occur weeks after the heart rhythm has returned to normal, suggesting that they might not be directly caused by A-fib, Kowey said. Instead, the higher rate of stroke may stem from a related symptom: scarring on the atrial walls…
The rate of stroke in older people is about 1 percent to 2 percent per year. Among those diagnosed with A-fib, the risk is roughly three times that high, Kowey said…”
“The rate of ischemic stroke in patients with nonrheumatic AF averages 5% a year, which is somewhere between 2 and 7 times the rate of stroke in patients without AF. The risk of stroke is not due solely to AF; it increases substantially in the presence of other cardiovascular diseases. [32] The prevalence of stroke in patients younger than 60 years is less than 0.5%; however, in those older than 70 years, the prevalence doubles with each decade. [33]
The attributable risk of stroke from AF is estimated to be 1.5% for those aged 50-59 years, and it approaches 30% for those aged 80-89 years. Women are at a higher risk of stroke due to AF than men and some have suggested this may be due to undertreatment with warfarin. However, one study of patients 65 years or older with recently diagnosed AF found warfarin use played no part in the increased risk of stroke among female patients. [34]..
APPIP ERROR: amazonproducts[
AccessDeniedAwsUsers|The Access Key Id AKIAJAJ37JVNL7OUU4CA is not enabled for accessing this version of Product Advertising API. Please migrate your credentials as referred here https://webservices.amazon.com/paapi5/documentation/migrating-your-product-advertising-api-account-from-your-aws-account.html.
]




