Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- Skin Cancer »
- Actinic Keratosis – Treating Pre-Pre Skin Cancer
Actinic Keratosis – Treating Pre-Pre Skin Cancer
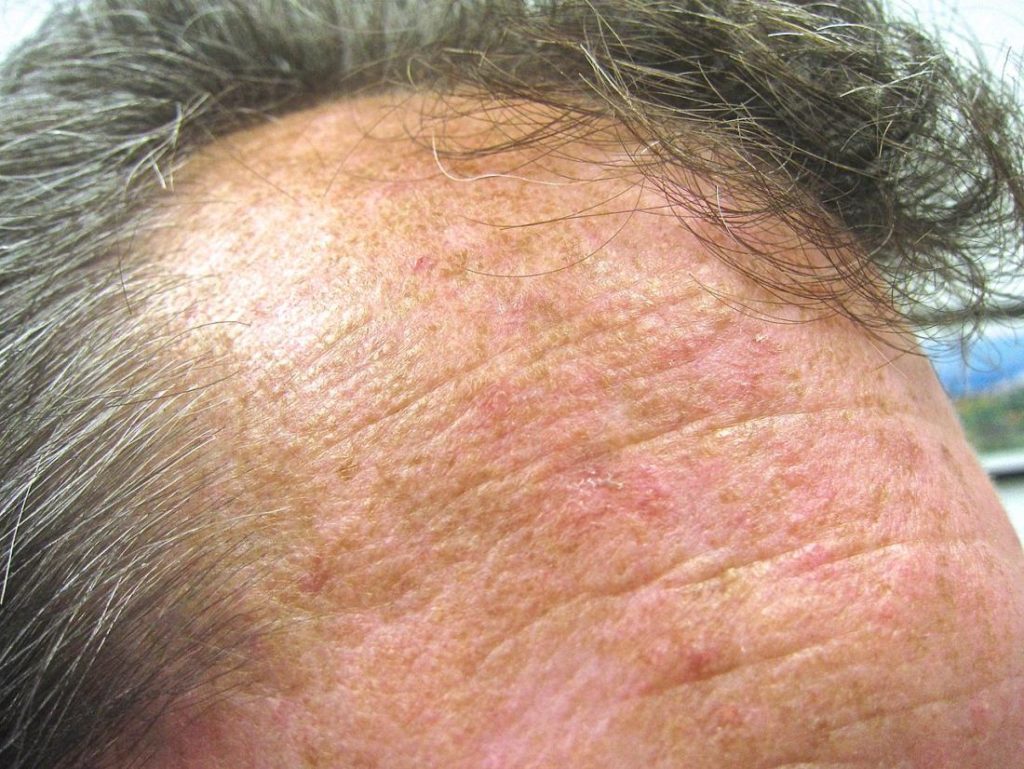
“Actinic keratosis (AK), the most common in situ cancerous skin lesion, was first described by Dubreuillh over one hundred years ago [1]. AKs are caused by chronic exposure to ultraviolet rays from sunlight…”
Actinic Keratosis (AK) is not cancer. AK increases the risk of cancer but it’s not cancer.
I wish I knew then what I know now. I used to sit in the sun constantly as a teen. Sun burned? Frequently. Here I am in my sixties, a cancer survivor who has had lots of chemotherapy, radiation and a stem cell transplant, and I have many reasons why I am have a real risk of skin cancer.
Non-melanoma skin cancer (basel, squamous cell) is diagnosed 2-3 million times in the U.S. annually
According to the Skin Cancer Foundation, at 58 million diagnoses, actinic keratosis (AK) is the most common precancer that forms on skin damaged by chronic exposure to ultraviolet (UV) rays from the sun and/or indoor tanning. Solar keratosis is another name for the condition.
AKs result from long-term exposure to ultraviolet (UV) radiation. This means that if you already have an AK, you are likely to develop more actinic keratoses (plural) in the future. This puts you at a higher risk for skin cancer, since AKs can develop into squamous cell carcinoma (SCC), a common and sometimes invasive form of the disease.
Non-Melanoma Skin Cancer at a Glance-
- Risks– UV Exposure, HPV, Genetics, Skin Pigment, Immunosuppression, Radiation Therapy, Age, Previous Skin Cancer,
- Symptoms– Itching, Bleeding, Shape (A,B,C,D,E).
- Diagnosis– Visual inspection (A,B,C,D,E), Skin Biopsy (Shave, Punch, Incisional/Excisional)
- Prognosis- Staging-
- Therapy– Conventional, Non-Conventional, Integrative, Alternative
- To Learn More About Non-Toxic Pre-Cancer Therapies- click now
- To Learn More About Actinic Keratosis- click now
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Non-Melanoma Skin Cancer Risk Increases From Radiation
- Preventing Non-Melanoma Skin Cancer Relapse
- How to Identify Skin Cancer in 5 Steps
- Skin Cancer, Vitamin D3 and Sunlight
Actinic Keratosis and Non-Invasive Diagnostic Techniques: An Update
“Actinic keratosis (AK), the most common in situ cancerous skin lesion, was first described by Dubreuillh over one hundred years ago [1]. AKs are caused by chronic exposure to ultraviolet rays from sunlight [2,3]. The lesions have not yet acquired the full complement of chromosomal aberrations and invasive growth characteristics that are associated with invasive squamous cell carcinoma (SCC), and are considered the most important predisposing factor for SCC [4]…
Three different pathways have been described for AKs: regression, persistence, or progression toward in situ or invasive SCC. Although the actual risk for an individual AK progressing to invasive SCC is unclear, estimations vary from as low as 0.1% to as high as 20% [9,10]….
Even with a low individual rate of progression, patients with multiple AKs (i.e., more than 10) may have a 14% cumulative probability of developing an SCC, either within the AK or de novo, within 5 years [9].
The relative risk of SCC also increases with the number of AKs; around 1% for patients with 5 or fewer AK lesions and up to 20% for patients with more than 20 AK lesions [11]…
Whether it is cost-effective to treat all AK lesions for SCC prevention is unclear [14]…
Multiple lesions, both clinically observable and subclinical, may exist across the entire areas of sun-damaged skin as a result of UV-induced field cancerization. AK share many similar molecular and histological features with SCC, and it can sometimes be difficult to clinically distinguish between the two.
Clinical presentation of AK is often widely variable, and although several symptoms (e.g., bleeding, tenderness, and size) suggest more invasive disease, certain diagnosis requires histopathological examination of a biopsy sample. Multiple AKs would therefore require multiple biopsies which are not always feasible for timing, costs and aesthetic restriction due to scars that a biopsy leaves..
In 2007, a clinical classification for grading AK (grades 1, 2, and 3) was developed [15];
- grade 1 describes slightly palpable AKs (better felt than seen),
- grade 2 are moderately thick AKs (easily felt and seen), and
- grade 3 are very thick, hyperkeratotic, and/or obvious AKs.
A similar scheme for the dermoscopic, confocal, and histologic grading of AKs has also been established. The clinical diagnosis between grade 3 AK and early invasive SCC, however, is subject to variable clinical interpretation…
Dermoscopy permits the visualization of skin structures with polarized light at a 6- to 100-fold magnification, reaching the depth of the papillary dermis [16]. The usefulness of dermoscopy in differentiating melanocytic from non-melanocytic pigmented skin lesions, both benign and malignant, is widely recognized [17,18]…
Conclusions
A number of noninvasive diagnostic methods are nowadays available for assistance in AK diagnosis. The obvious advantage of noninvasive diagnostic tools is the option to examine tissue in vivo, potentially reducing the need for biopsy. Dermoscopy is extremely helpful in the diagnosis of melanoma and BCC but it is not as useful in AK diagnosis, especially in the case of pigmented AKs…
Histology remains the gold standard for skin cancer diagnosis, and consequently also for AK diagnosis. However, a biopsy represents a sample of a single lesion, usually about 4 mm. As a consequence, especially for larger lesions, the biopsy sampling may not be representative of the entire lesion. In the presence of two histologically different pathologies within the same lesion, the fact that only a small sample of tissue is excised, an incorrect diagnosis and subsequent unsuitable therapy can be the result.
In most cases the operator decides to excise the biopsy in the area considered most representative within the lesion; this decision is usually guided by dermoscopy but does not exclude evaluation error. RCM and OCT enable in vivo and noninvasive evaluation of the whole lesion. The study of the entire lesion makes the diagnosis more certain and consequently allows the best treatment choice…”