
Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Anterior Cervical Spine Surgery (ACSS), Radiation & Difficulty Swallowing/Dysphagia
Anterior Cervical Spine Surgery (ACSS), Radiation & Difficulty Swallowing/Dysphagia
“They include xerostomia, dysgeusia, fibrosis, lymphedema, dysphagia, dental caries, osteoradionecrosis, hearing loss, neuropathy, and changes in voice quality.”
I underwent anterior cervical spine surgery (ACSS) to my neck in early 1995. I then underwent radiation to the neck area in an effort to zap any remaining cancer cells. The two studies linked and excerpted below represent what I believe are causes of my dysphagia- difficulty swallowing.
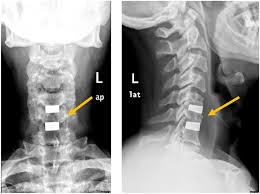
In the top article below, the side effect caused by my surgery is explained. As the x-ray in the upper right corner of the page indicates, I had a metal strut placed in my neck separating my fourth cervical vertebra and my C6.
I distinctly remember having lunch with my soon-ro-be-wife after leaving the hospital where I had undergone surgery to my neck just a week before.
My first bite of lunch resulted in a severe choking fit on my part. As the article explains, my dysphagia healed over the next few weeks and I believed that this was the end of this particular side effect… wishful thinking…
Approximately 8-10 years later I again began experiencing difficulty swallowing. Long-story short, I figured out that the local radiation to my C5 (neck surgery) was causing radiation-induced dysphagia.
The point of this post is to highlight two instances of the same side effect- dysphagia- yet caused by two different therapies- surgery and radiation- twice, years apart.
First and foremost, don’t expect your oncology nurse to educate you about the short, long-term and late stage side effects that you may develop based on your surgery and/or radiation therapy. Oncology nurses, in my experience anyway, are well-trained and well-meaning but often very busy people.
Further, again based on my experience, my surgery and radiation-induced side effects all were short, and then long-term and late stage, meaning they all took hold over days, weeks, months, years after I left the hospital.
Possible therapies-
- Physical Therapy-
- Hyperbaric Oxygen Therapy (HBOT)-
- Acupuncture-
To this day I exercise my neck muscles daily. Picture doing sit-ups with my head. I started slowly by holding my head up while lying prone on my back, for as long as I could. Only 20-30 seconds at first. After years of practice I can now do dozens of head sit-ups daily.
I do choke on occasion. I cannot speak loudly for any length of time. And you can forget any shouting on my part. My plan however, is to continue my head sit-ups daily so that I can eat and swallow normally most of the time. And to always have a glass of water/juice/etc. near-by.
This is a broad statement to make but I now believe that anyone undergoing radiation treatment should also undergo HBOT immediately following their radiation. Radiation damages normal cells in our bodies. HBOT can heal this damage.
I undergo acupuncture frequently primarily due to another side effect called radiation-induced xerostomia. Because this treatment seems of have helped my xerostomia, I have to believe that this procedure has a positive effect on my dysphagia as well.
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Prevent, Minimize, Heal Chemo brain
- Got Cancer? Chemotherapy is toxic- less is more
- Exercise Oncology for Myeloma Patients
Understanding swallowing difficulties after spine surgery can improve quality of life
“Difficulty swallowing is one of the most common complications of anterior cervical spine surgery (ACSS). Investigators who evaluated possible risk and contributing factors report in Advances in Communication and Swallowing that although most difficulties resolve within two months, the perception of swallowing difficulty can persist for longer, but this does not always correlate with test results.
More than 70% of patients report dysphagia symptoms within two weeks following ACSS. Contributing factors may include extent of surgery, prevertebral soft tissue swelling, or altered sensation secondary to nerve traction during surgery.
“We see many patients suffering with this problem after ACSS,” explained lead investigator Ashli K. O’Rourke, MD, Medical University of South Carolina. “The perception of swallowing difficulty can persist for more than two months following ACSS but often does not correlate with current gold standard testing. This can be a frustrating situation for patients who are given no specific explanation for their complaints…”
Medical records were then reviewed to ensure patients had new onset of subjective complaints of dysphagia after surgery (e.g., food sticking, coughing during meals) prompting a referral for VFSS. Patients with pre-existing documented dysphagic complaints, altered diets, or gastric tube placement were excluded…
Understanding the Management of Chronic AEs After Radiation Therapy
“Treatment techniques and comorbidities have a significant impact on the severity of chronic side effects,” said Haynes-Lewis, a nurse practitioner at Montefiore Einstein Center for Cancer Care. “Nurses should work with the patients to develop a plan to manage chronic side effects that optimize quality of life…”
To start, she added, knowing the difference between late AEs (those that occur or begin after therapy is completed and may occur months to year post-treatment) and long-term AEs (prolonged effects that begin during treatment and continue beyond the end of treatment) is important…
Central Nervous System- Disease sites under this category can include the brain and spinal cord, from which the tissue are late reacting. Therefore, these changes are found, not in the clinic, but through imaging.
AEs of the central nervous system include increased atherosclerosis of the blood vessels in the brain, increased incidence of secondary brain tumors, radiation necrosis, cognitive decline, hormonal deficits, vision changes, hearing loss, and radiation myopathy…
AEs associated with the central nervous system are often treated with steroids, bevacizumab (Avastin), hyperbaric oxygen therapy, surgical resection, memantine, donepezil (Aricept), cognitive rehabilitation, cochlear implants, hormonal replacement, and pentoxifylline…
Head and Neck-These AEs can occur in the nasopharynx, oral cavity, salivary glands, or neck. They include xerostomia, dysgeusia, fibrosis, lymphedema, dysphagia, dental caries, osteoradionecrosis, hearing loss, neuropathy, and changes in voice quality.
“These side effects affect every part of your life and your quality of life,” Haynes-Lewis said.
Management of these AEs can include acupuncture and massage, therapy (physical therapy, decongestive therapy, swallowing rehabilitation), and medications such as pentoxifylline, vitamin E, analgesics, saliva substitutes and stimulants, conservative debridement, hyperbaric oxygen, surgical resection and reconstruction, hearing aids, tympanostomy and aspiration, myringotomy and grommet insertion, voice therapy, and injection larynoplasty…
“Nurses should be at the forefront of chronic side effect management as part of survivorship care as the number of cancer survivors continue to increase,” she concluded.”

