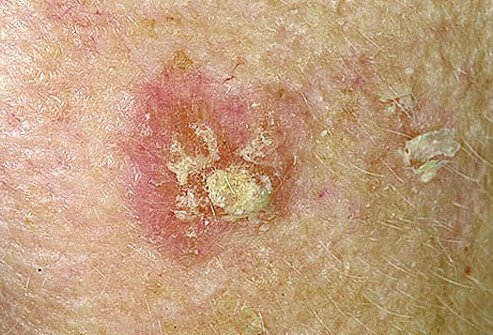
“Atypical Mole Syndrome is the most important phenotypic risk factor for developing cutaneous melanoma…”
If you have atypical mole syndrome (AMS) and if your family is affected by AMS then, according to the study linked and excerpted below, your risk of melanoma increases dramatically.
While the proposed solution to this increased risk, at least as far as the article is concerned, is to monitor your skin regularly.
My belief as a long-term cancer survivor and cancer coach is to also practice evidence-based, non-toxic therapies shown to both reduce your risk of mel. as well as reduce your risk of skin damage.

“Prospective studies show that the risk of melanoma in members of families affected by AMS and FAMMM is significant, with an estimated cumulative risk of 49% in individuals 10 to 50 years of age and 82% in individuals 72 years of age.32“
While I can’t say that I have that many moles (to the left), I do have many. I do keep an eye on my skin.
I just went to my dermatologist and had him remove several and biopsy them. The biopsy’s came back negative.
But my point is that I am vigilant. And I live an evidence-based but non-conventional, anti-skin cancer lifestyle. I eat a clean diet aka lots of fruits and veggies, nutritional supplementation shown to reduce my risk of melanoma and I no longer worship the sun.
Have you been diagnosed with AMS? Do you have dysplastic nevi? Scroll down the page, post a question or comment and I will reply ASAP.
Thanks,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
“Atypical Mole Syndrome is the most important phenotypic risk factor for developing cutaneous melanoma, a malignancy that accounts for about 80% of deaths from skin cancer. Because the diagnosis of melanoma at an early stage is of great prognostic relevance, the identification of Atypical Mole Syndrome carriers is essential, as well as the creation of recommended preventative measures that must be taken by these patients...”
Although it corresponds to only 4% of all skin cancers, it accounts for 80% of skin cancer deaths.4 Because early detection of the disease is implicit in its cure and only 14% of patients with metastatic disease survive beyond 5 years,4–6knowledge of factors that increase an individual’s risk for developing melanoma and diagnosis at an early stage of the disease have great prognostic relevance…
Clinical Diagnosis

Clinically, a dysplastic nevus is most often a spotted lesion of 5 mm or more in diameter, with irregular and poorly defined borders and variable shades of brown, and it may present a reddish hue, with bleaching accomplished using vitropressure.18 It often presents a central papule, surrounded by a pigmented macular ring, giving the appearance of a “fried egg”.18 Thus, there is considerable overlap with the ABCDE rule used for clinical diagnosis of melanoma, namely, A: asymmetry, B: irregular borders C: varied colors, D: diameter > 6 mm and E: elevation (simultaneous presentation of macular and papular components) ().3,12,18
CONCLUSION
AMS demonstrably increases the risk of developing melanoma, a malignant neoplasm for which incidence have increased significantly in recent decades and for which early diagnosis is of great importance in the prognosis of the disease.4,5“
“Atypical moles, also known as dysplastic nevi, are unusual-looking moles that have irregular features under the microscope. Though benign, they are worth more of your attention because individuals with atypical moles are at increased risk for melanoma, a dangerous skin cancer.
An atypical mole can occur anywhere on the body. The appearance of these moles can vary greatly. The best advice is to know your skin. Keep track of any and all moles you may have. This gives you the best chance to spot anything new, changing or unusual and bring it to the attention of your dermatologist…
- An atypical mole is not a skin cancer but having these moles is a risk factor for developing melanoma.
- Although rare, melanoma can arise in association with atypical moles. That is why it is important to be aware of these moles, get them checked by your dermatologist, and watch out for changing moles.
- If you have atypical moles plus a family history of melanoma, you have an increased risk of developing melanoma.
- If you have any common melanoma risk factors plus atypical moles, you must be particularly watchful:
- Fair skin, light eyes or hair
- Freckles
- Many moles
- A personal or family history of melanoma or nonmelanoma skin cancer
- Photosensitivity
- Inability to tan
- Repeated and intermittent sunburns
It’s important to note that even without a family history of melanoma, if you have atypical moles, you have an elevated risk of developing melanoma…'”