
Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Barrett’s Esophagus- W/, Without Dysplasia- Non-Toxic Therapy
Barrett’s Esophagus- W/, Without Dysplasia- Non-Toxic Therapy
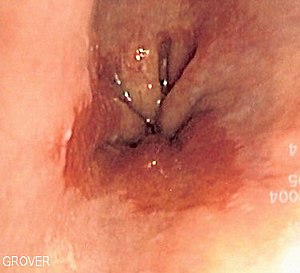
What is Barrett’s Esophagus? What does it mean to have dysplasia? High-grade? Low-grade? Is BE cancer? How can BE be healed?
If you’ve been diagnosed with Barrett’s Esophagus (BE), take a deep breath. The goal of this post is to address your questions and/or concerns in addition to offering evidence-based non-toxic GERD and BE therapies to manage your risk of GERD from becoming BE or BE from becoming EC.
If you have any questions after reading this post, scroll down the page and email a question or a comment to me. I will reply to you ASAP.
Gastrointestinal Reflux Disease (GERD)
According to research approximately 18.6 million Americans had symptoms of GERD (gastrointestinal reflux disease) in 2010. About 10%-15% percent of GERD patients will develop Barrett’s Esophagus (BE). Less than 1% of Barrett’s patients will develop esophageal cancer. A small percentage but a substantial number of people diagnosed diagnosed annually with an aggressive cancer.
Barrett’s Esophagus (BE)
First and foremost, Barrett’s esophagus is not cancer. BE does increase your risk of esophageal cancer (EC). And EC is a type of cancer with an especially poor five-year survival rate. So in my experience, you want to take every evidence-based, non-toxic step in order to reduce your risk of EC.
If you are diagnosed with BE with dysplasia, there are two levels of risk:
- Low-grade
- High-grade
As you can imagine, high-grade BE signals a greater risk of esophageal cancer.
- are age 50 years or older,
- male sex,
- white race,
- chronic GERD,
- hiatus hernia,
- elevated body mass index,
- and intra-abdominal distribution of body fat
I am a survivor of a completely different type of cancer called multiple myeloma. Long-story but I am at an increased risk of GERD, BE and EC due to long-term side effects I developed from chemotherapy and radiation. I study and write about MM as well as GERD, BE and EC because I want to “know my enemy” so to speak.
The same diet, nutritional supplementation and anti-cancer lifestyle therapies that I pursue daily to keep me in complete remission from my MM, also has kept me free of GERD, BE and EC according to the studies linked below.
My advice to anyone reading this post who has been diagnosed with either GERD, or BE (with, w/out dysplasia), is to get regular check-ups as well as pursue a clean, nutritious diet combined with anti-oxidant, anti-inflammatory supplements such as:
- Vitamins C, E, D and B complex
- Supplements such as Curcumin, Omega-3 fatty acids…
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
Barrett’s Esophagus with Dysplasia
“Barrett’s esophagus is a condition in which the tissue lining the esophagus – the tube that passes the food from the mouth to the stomach – is replaced by tissue similar to that of the intestinal lining. This occurs chiefly in the cells of the epithelial tissue which lines the lower end of the esophagus.
About 10% of the patients with gastroesophageal reflux (GERD) may be expected to develop Barrett’s esophagus, and in about 10% of the patients with Barrett’s esophagus, dysplasia occurs.
Dysplasia is a pre-cancerous stage in Barrett’s esophagus, where the cell develops abnormal features. However, these abnormal cells do not have the capability to spread to other parts of the body. Depending upon the grades of dysplasia, treatment options are available…
Characteristics of Dysplasia in Barrett’s Esophagus
There are two grades of dysplasia in Barrett’s esophagus:
- low-grade dysplasia and
- high-grade dysplasia.
These are identified through either endoscopy or biopsy…
Low Grade Dysplasia in Barrett’s Esophagus
If microscopic examination reveals the presence of a few cells with mildly abnormal features, it is termed “low-grade dysplasia” (LGD). This condition is considered as the earliest precancerous stage of the esophageal epithelium…
Diagnosis and Treatment
In low-grade dysplastic BE, the diagnosis might be difficult as there is little difference seen between “indefinite for dysplasia” and LGD in biopsies. However, there are substantial inter- and intra-observer differences in the diagnosis of both these conditions, which are thus combined into one as regards their clinical management.
LGD requires effective treatment of the gastroesophageal reflux with proton pump inhibitors, or PPIs. Maintaining a healthy and balanced diet can also help in reducing the reflux. Regular biopsies are suggested to make sure that the dysplasia will not progress or develop into malignancy…
In cases where the acid reflux drugs do not produce adequate response and fail to eliminate the dysplasia, endoscopic eradication therapy (EET) is suggested…
Radiofrequency Ablation (RFA)
- In the RFA technique, radiofrequency waves are passed through a catheter to remove the diseased tissue in the esophagus without causing too much damage to the healthy neighboring tissues.
- Replacement of abnormal Barrett’s tissue by healthy tissue takes about four weeks with the RFA treatment…
Endoscopic eradication therapy for Barrett’s Esophagus related neoplasia.
“Background and Aims- Long-term durability data for effectiveness of radiofrequency ablation (RFA) to prevent esophageal adenocarcinoma in patients with dysplastic Barrett’s esophagus (BE) are lacking.
Methods-We prospectively collected data from 2,535 patients with BE (mean length 5.2cm, range 1-20cm) and neoplasia (20% low-grade dysplasia, 54% high-grade dysplasia, 26% intramucosal carcinoma) who underwent RFA therapy across 28 UK hospitals. We assessed rates of invasive cancer and performed detailed analysis of 1,175 patients to assess clearance rates of dysplasia (CR-D) and intestinal metaplasia (CR-IM) within 2 years of starting RFA therapy. We assessed relapses and rates of return to CR-D (CR-D2) and CR-IM (CR-IM2) after further therapy. CR-D and CR-IM were confirmed by absence of dysplasia and intestinal metaplasia on biopsies taken at two consecutive endoscopies.
Results- Ten years after starting treatment, Kaplan Meier (KM) cancer rate was 4.1% with a crude incidence rate of 0.52 per 100 patient years. CR-D and CR-IM after 2 years of therapy were 88% and 62.6% respectively. KM relapse rates were 5.9% from CR-D and 18.7% from CR-IM at 8 years, with most occurring in the first 2 years. Both could be successfully retreated with CR-D2, 63.4% and CR-IM2, 70.0% two years after retreatment. EMR before RFA increased likelihood of rescue EMR from 17.2% to 41.7%, but did not affect the rate of CR-D, whereas rescue EMR after RFA commenced reduced CR-D from 91.4% to 79.7% (Χ2 p<0.001).
Conclusion- RFA treatment is effective and durable to prevent esophageal adenocarcinoma. Most treatment relapses occur early and can be successfully retreated…”
Curcumin: A Potent Protectant against Esophageal and Gastric Disorders
“In in vivo studies, curcumin was compared with lansoprazole, the proton pump inhibitor (PPI) commonly used as the recommended standard drug against GI-tract disorders including GERD [18,19].
In these reports, curcumin was shown to effectively prevent the esophageal mucosal damage induced by acute reflux esophagitis [18,19]. Although curcumin was documented as less potent than the proton pump inhibitor (PPI) lansoprazole in the inhibition of acid reflux esophagitis, it became superior to lansoprazole in the inhibition of mixed acid-bile reflux-induced esophagitis. This protective mechanism caused by curcumin in the esophagus has been attributed to the antioxidant nature of this turmeric derivative [18,19]…”
Dietary Supplement Use and Risk of Neoplastic Progression in Esophageal Adenocarcinoma
“In summary, results from this first prospective study of supplement use and neoplastic progression of Barrett’s esophagus suggest that risk of EA is reduced with daily use of multivitamins and supplements containing vitamins C and E.
Whether a specific nutrient on its own is responsible for this observation cannot be determined using current available data. These findings, which require replication, suggest that multivitamin supplement use may be an effective means of prevention progression to cancer in persons with Barrett’s esophagus…”

