Leave a Comment:
1 comment
[…] To Learn more about Elderly Breast Cancer- click now […]
Reply
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
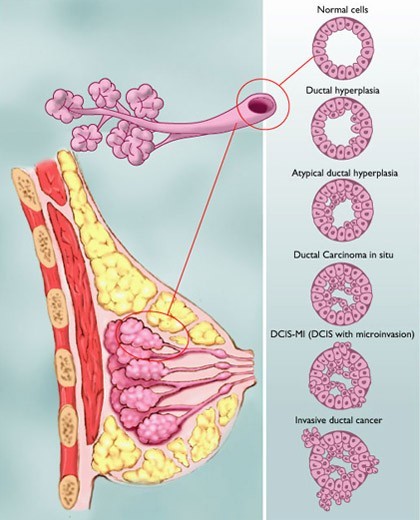
My mom, Mary, was given a mammorgram a couple of years ago. Mom was diagnosed with early breast cancer at the age of 75 in 2006 and had a lumpectomy, local radiation and five years of tamoxifen. Mom’s most recent mammorgram revealed more DCIS. So mom had another lumpectomy.
I am a long-term cancer survivor. I struggle with a host of long-term and late stage side effects. My cancer care was also from University Hospitals. I can’t help but wonder if both my mom and I were overrated.
While mom doesn’t exactly fit the profile below she is pretty close. Two years ago mom had a little dementia, not “severe cognitive impairment.” And though mom was in her eighties I can’t say that her life expectancy was “limited.” But I’m her son so I guess I’m not a good judge of that.
I’m no expert, of course, but I have wondered about mom’s atrial fibrillation. I wonder if the radiation she underwent for her original earlier breast cancer caused it.
In any case, the article linked below seems to question my mom’s mammorgram and lumpectomy. I wonder myself.
Did University Hospital of Cleveland overtreat my mom?
To Learn More about breast cancer in elderly patients- click now-
David Emerson
“Elena Altemus is 89 and has dementia. She often forgets her children’s names, and sometimes can’t recall whether she lives in Maryland or Italy.
Yet Elena, who entered a nursing home in November, was screened for breast cancer as recently as this summer. “If the screening is not too invasive, why not?” asked her daughter, Dorothy Altemus. “I want her to have the best quality of life possible.”
But a growing chorus of geriatricians, cancer specialists and health system analysts are coming forth with a host of reasons: Such testing in the nation’s oldest patients is highly unlikely to detect lethal disease, hugely expensive and more likely to harm than help since any follow-up testing and treatment is often invasive.
And yet such screening — some have labeled it “overdiagnosis” — is epidemic in the United States, the result of medical culture, aggressive awareness campaigns and financial incentives to doctors…
By looking for cancers in people who are unlikely to benefit, “we find something that wasn’t going to hurt the patient, and then we hurt the patient,” said Dr. Sei Lee, an associate professor of geriatrics at the University of California-San Francisco.
Nearly 1 in 5 women with severe cognitive impairment — including older patients like Elena Altemus — are still getting regular mammograms, according to the American Journal of Public Health — even though they’re not recommended for people with a limited life expectancy..
Among people in their 70s and 80s, cancer screenings often detect slow-growing tumors that are unlikely to cause problems in patients’ lifetimes. These patients often die of something else — from dementia to heart disease or pneumonia — long before their cancers would ever have become a threat…”
[…] To Learn more about Elderly Breast Cancer- click now […]
Reply