
Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- Skin Cancer »
- Can Dysplastic Nevi Result in Metastatic Melanoma?
Can Dysplastic Nevi Result in Metastatic Melanoma?
Excision of Dysplastic Nevi is prompted by an uncertain malignancy potential and the fear of undertreating an evolving malignant melanoma (MM)…
Rather than worrying about DN /atypical moles, consider evidence-based, non-toxic, therapies to reduce your risk of skin cancer. Or I should say, in addition to skin checks, biopsy, consider nutritional supplementation shown to reduce he risk of skin cancers.
According to the info posted and excerpted below, yes atypical moles are more likely than ordinary moles to become melanoma. So if you identify an atypical mole you may have it removed by your dermatologist.
 Fine. Problem solved… Maybe. The challenge, according to the Medscape article below, is that pathologists don’t agree on which moles may or may not be at risk for developing into melanoma.
Fine. Problem solved… Maybe. The challenge, according to the Medscape article below, is that pathologists don’t agree on which moles may or may not be at risk for developing into melanoma.
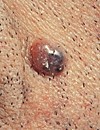
I have six of the melanoma risk factors listed below. My shoulders, chest and upper body look like the photo to the left.
Melanoma at a glance-
- Risks– UV Exposure, HPV, Genetics, Skin Pigment, Moles, Immunosuppression, Previous Skin Cancer Diagnosis,
- Symptoms- Mole, Shape (A,B,C,D,E), Itching, Bleeding,
- Diagnosis- Visual Inspection, Skin Biopsy,
- Prognosis– Staging, In-situ, I, II, III, IV, Five year survival rates
- Therapy– Conventional, Non-Conventional, Integrative, Alternative
I had a mole appear on my face seemingly out of nowhere a few years ago. After watching this mole grow and darken I got nervous and had it removed by my dermatologist. If it returns I will have it “re-excised” aka cut it off again. But rather than examine my skin repeatedly I have decided to add evidence-based, non-toxic therapies to my day. Nutrition, supplementation, lifestyle, etc.
That mole removal and biopsy was in 2005. Jump ahead to 2022- four more moles removed and biopsied. No non-melanoma skin cancer, no full melanoma. Two spots were frozen off aka cryoptherapied. Not a word but you get the idea.
I keep an eye on my skin, get anything suspicious biopsied and live an evidence-based, lifestyle directed at reducing my risk of skin cancer.
I am am both a long-term survivor of an incurable cancer called multiple myeloma and cancer coach. I have learned to rely on multiple evidence-based but non-conventional therapies to manage my blood cancer and possible secondary cancer including melanoma.
Scroll down the page, post a question or comment and I will reply to you ASAP.
Thanks,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Basal Cell Carcinoma Treatment
- Skin Cancer As You Age- Before, During and After Diagnosis
- The “BEST” Treatments for Basel Cell Carcinoma?
“A dysplastic nevus or atypical mole is a nevus (mole) whose appearance is different from that of common moles. An atypical mole may also be referred to as an
- atypical melanocytic nevus,[2]
- atypical nevus,
- B-K mole,
- Clark’s nevus,
- dysplastic melanocytic nevus, or
- nevus with architectural disorder.[3]
Cancer
According to the National Cancer Institute, researchers have shown that atypical moles are more likely than ordinary moles to develop into a type of skin cancer called melanoma. It is worth noting that the vast majority of atypical moles will never become malignant. However, numerous studies indicate that about half of melanomas arise from atypical moles. Evidence supporting this connection arises from clinical photodocumentation of evolving lesions, patient self-reports of changing lesions, pathology studies showing dysplastic nevi in histologic contiguity with melanoma, and epidemiology studies indicating that about half of individuals affected by melanoma also have atypical moles. Epidemiology studies have also shown that individuals with multiple dysplastic nevi are at much higher risk for developing melanomas…
Atypical (Dysplastic) NeviOutcomes of Surgical Excision and Association With Melanoma
“Objective To evaluate the effect of surgical excision, performed after biopsy diagnosis of dysplastic nevus, on final diagnosis, melanoma prevention, and melanoma detection…
Main Outcomes and Measures In dysplastic nevi cases, the rate of clinically significant change in diagnosis and the rate of melanoma detection as a result of excision. In melanoma cases, the rate and characteristics of association with dysplastic nevus.
Results Of dysplastic nevi, 196 of 580 (34%) showed a positive biopsy margin, increasing with grade of atypia (P < .001); 127 of 196 with positive biopsy margin received excision (65%), performed more often as grade of atypia increased (P < .001). Two excisions (2 of 127, 1.6%) resulted in a clinically significant change in diagnosis, from biopsy-diagnosed moderately-to-severely dysplastic nevi before excision to melanoma in situ after excision. In melanomas (n = 216), in situ and superficial spreading subtypes were more often associated with dysplastic nevi (20% and 18%, respectively) (P = .002), most often of moderate-to-severe or severe grade.
Conclusions and Relevance Excision of biopsy-diagnosed mildly or moderately dysplastic nevi is unlikely to result in a clinically significant change in diagnosis, and risk of transformation to melanoma appears very low. Moderately-to-severely and severely dysplastic nevi are more often associated with melanoma, and excision may be beneficial for melanoma detection or prevention.
Atypical nevi are common, with an incidence of 2% to 8% in white patients.4,5 Many are biopsied to evaluate for melanoma.4 Management of a biopsy-proven dysplastic (atypical) nevus with a positive histologic margin remains ill defined.6 Particularly after a biopsy finding of mildly or moderately dysplastic nevus with positive histologic margin, there is significant variation and lack of consensus in subsequent management.6
Surgical excision of the dysplastic nevus biopsy site with a 2- to 3-mm margin of normal skin is frequently performed. The goal of excision is to confirm the biopsy diagnosis, to ensure complete removal due to concerns of future malignant transformation, or both. These goals include melanoma detection and prevention. The lifetime transformation risk of an “average” dysplastic nevus into melanoma is estimated at 1 in 10 000, though risk likely varies with grade of atypia.7 In addition, excision is sometimes performed to eliminate risk of a recurrent nevus, a benign lesion that rarely may be difficult to distinguish from melanoma.8 Disadvantages of excision include risks of scarring and surgical complications and utilization of health resources…”
Are We Overtreating Severely Dysplastic Nevi?
” Dermatopathologists typically use these histopathologic features to grade “gray area” melanocytic neoplasms as mild, moderate, or severe. However, agreement among dermatopathologists is surprisingly low, ranging from 35% to 58%.[1]
Excision of DN is prompted by an uncertain malignancy potential and the fear of undertreating an evolving malignant melanoma (MM), but re-excised DN are rarely upgraded histologically to MM; data show that this happens in 0%-2.7% of cases.[4] In contrast, a consensus has evolved that mildly to moderately DN should be clinically followed rather than excised due to the negligible risk for recurrent or metastatic disease, even in cases with positive margins.[5]
Consistent with the 2015 recommendations by the MPWG, most severely dysplastic nevi (SDN) are re-excised, even when margins are negative. But is this necessary or over treatment?…”

