Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Catheter Ablation for Afib Hurts More Than Helps?
Catheter Ablation for Afib Hurts More Than Helps?
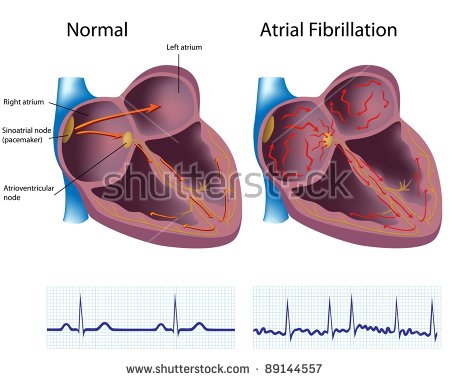
“In 2019, we do AF catheter ablation to improve quality of life. QOL is a reasonable endpoint, but it is more susceptible to the placebo effect.”
I’ve lived with atrial fibrillation since late 2010. I never had catheter ablation. I did see the risk/reward benefit of ablation.
The article linked and excerpted below questions the benefit of catheter ablation for people who have afib. Catheter ablation doesn’t cure Afib and catheter ablation causes side effects. Not many but there are there.
I think that there will always be AF patients who want to undergo catheter ablation even if they know that they will probably relapse and that there is a small risk of adverse events. The prospect of living without AF will push these patients to thrown caution to the wind. Quality of life is a strong predictor of behavior after all.
My point is that cardiology should be honest with patients and tell them what to expect. Risks, and costs, but probably quality of life. Not a cure for their AF.
I am calling for the elevation of quality of life (QOL) as the standard by which all therapies should be measured. If you can’t stand to have AF one more minute and you’ll risk anything and pay anything to take those risks, then go for either catheter ablation drug therapy.
To Learn More about chemotherapy-induced atrial fibrillation- click now
But if you find you can live with AF because you understand that all therapies offered by conventional medicine come with high costs- both financial as well as physical…well then live with AF.
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Catheter Ablation, Drugs or…Evidence-based Non-toxic therapies?
- Cancer Survivors’ and Falls- Prevention is Key to QOL
- Xarelto Lawsuit Highlights Risks of Conventional Blood Thinners
“Sobering” Long-Term Outcomes Following Ablation of Atrial Fibrillation
“Investigators report that most AF recurrences occur in the first six to 12 months and that there is a “slow but steady decline in arrhythmia-free survival” in the later years. Overall, the group contends that the ablation strategy–with repeat interventions as needed–provides “acceptable” long-term relief from the arrhythmia…
“The bottom line is that everybody’s results show the same thing, that atrial fibrillation is a complex arrhythmia, and that the longer you follow patients, the more recurrences they have,” said Calkins. He added that those arguing ablation “cures” atrial fibrillation have been disproven. “Catheter ablation treats atrial fibrillation, it doesn’t cure atrial fibrillation, at least in many patients,” added Calkins. “And yes, you have to continue to follow patients, and this has important implications in terms of anticoagulation…”
After a single ablation procedure, arrhythmia-free survival rates were 40%, 37%, and 29% at one, two, and five years. Most recurrences occurred within the first six months, while arrhythmias recurred in 10 of 36 patients who maintained sinus rhythm for at least one year. The only predictor of a recurrence in a univariate analysis was the type of atrial fibrillation, with long-standing atrial-fibrillation patients 1.9 times more likely to have a recurrence when compared with individuals who had the paroxysmal or persistent form of the arrhythmia…”
We Still Need a Sham-Controlled Trial for AF Ablation
Why Ablate?
We electrophysiologists have all had these cases: Before his ablation he was in and out of the hospital. He had multiple cardioversions and could not tolerate AF even for a few days. After the ablation he felt terrific. Only, at his 3-month check, he was in AFib (AF)…
This is no fluke. Nine years ago, the Mayo Clinic group published a prospective case series of more than 500 symptomatic patients who underwent AF ablation.[1] They reported on AF recurrence, quality of life (QOL), and AF symptoms.
Most patients improved. But get this: QOL improvement was not closely linked to ablative efficacy. While there was a trend toward better QOL in patients with AF elimination, improvement was also seen in patients with AF control on rhythm drugs, and in those with recurrent AF.
The researchers wrote that “the clinical relevance of these findings is substantial.” Yes, indeed. Since then, we have results from CABANA, which found that catheter ablation did not significantly reduce the primary composite of hard outcomes compared with medical management.[2]
In 2019, we do AF catheter ablation to improve quality of life. QOL is a reasonable endpoint, but it is more susceptible to the placebo effect.
In the Canadian-led DISCERN AF study,[3] 50 patients who had AF ablation also had implantable loop recordings from before and after the procedure. Crucially, the patients were blinded to the results. Ablation reduced AF burden but markedly increased the proportion of asymptomatic AF episodes. In fact, being postablation was the strongest predictor of having asymptomatic AF…
While AF ablation has become safer in recent years, you cannot do this procedure without the risk of harming or even killing a person. No procedure is totally safe, but putting people in harm’s way should come with a high bar of benefit. ..
We’ve all seen images from pacing devices showing that ablation has vanquished AF episodes. But as I’ve already noted, AF episodes are a poor surrogate marker for symptoms or stroke.”