Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Chemo-Induced Atrial Fibrillation, A Fib- Non-Toxic Therapy
Chemo-Induced Atrial Fibrillation, A Fib- Non-Toxic Therapy
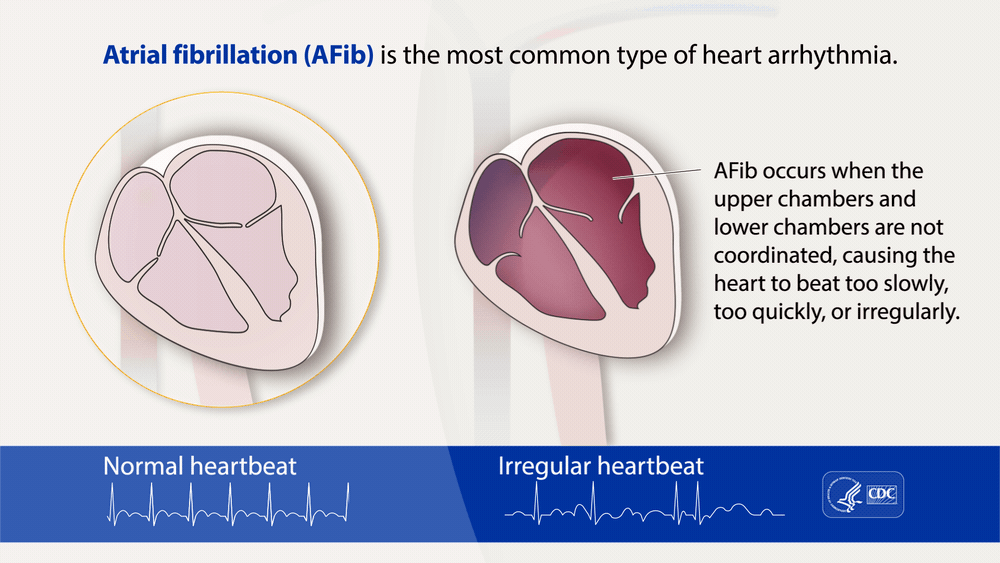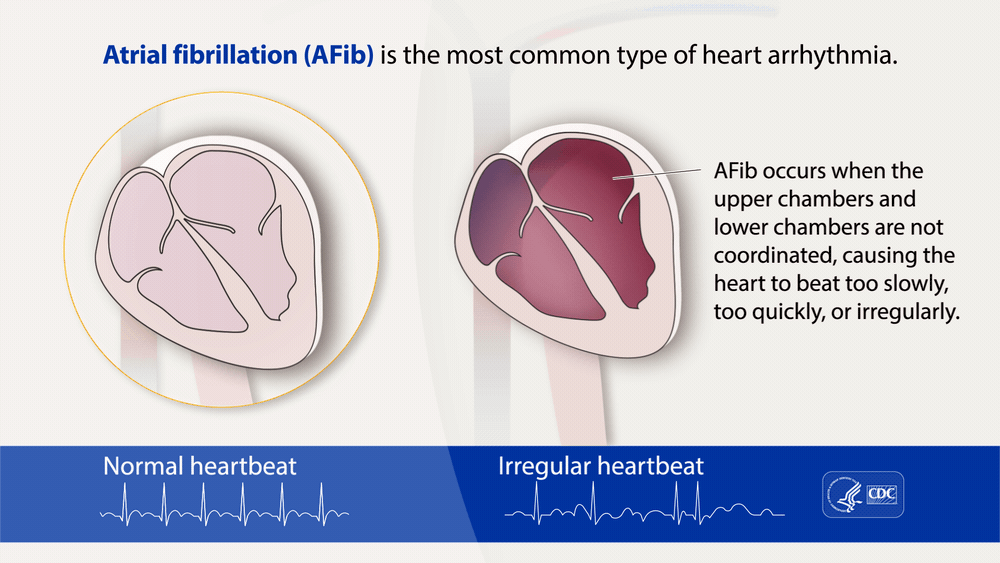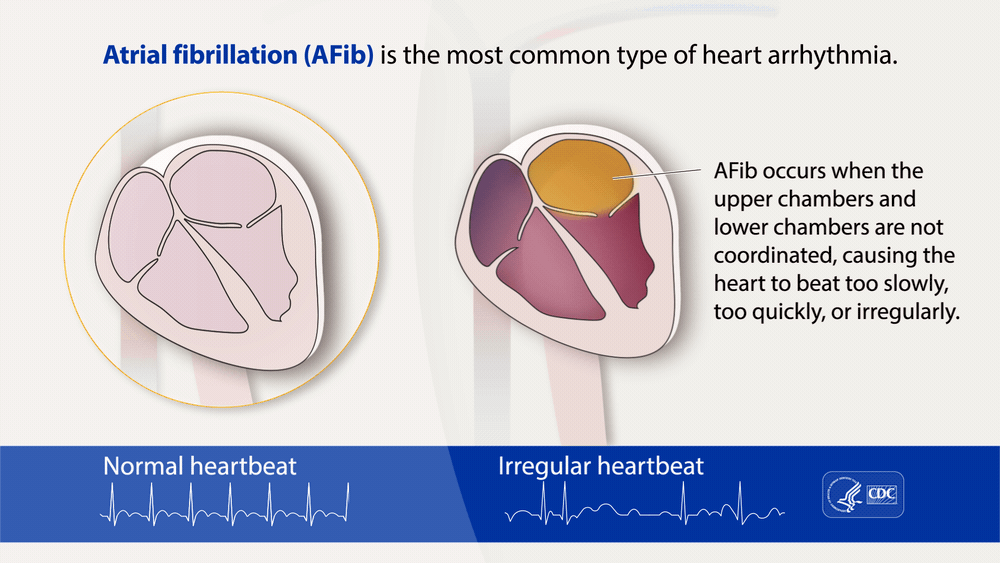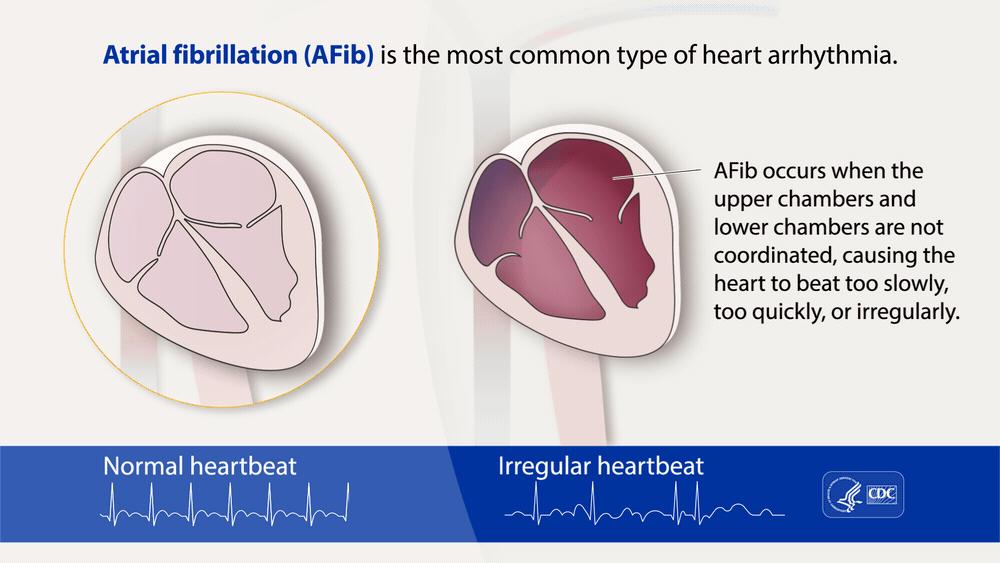
“Atrial fibrillation, often called AFib or AF, is the most common type of treated heart arrhythmia. An arrhythmia is when the heart beats too slowly, too fast, or in an irregular way.”
According to the research linked below, many different chemotherapy regimens are cardiotoxic. That is to say that many newly diagnosed cancer patients undergo chemotherapy that damages their heart muscle. This damage can be a short-term (immediate), long-term (weeks, months after therapy) or late stage side effect (years after chemotherapy).
It is important to understand that cardiotoxic chemotherapy can kill. It is also important to understand that there are many evidence-based but non-conventional, non-toxic therapies that can reduce or eliminate the damage done by cardiotoxic chemo regimens.
I developed atrial fibrillation aka AFib aka AF in late 2010. I underwent several different cardiotoxic chemotherapies during my active therapies in the years following my multiple myeloma diagnosis in early 1994.
My Afib is chronic meaning my heart beats irregularly all the time, 24/7. Some AFib goes in and out of normal heart beats.
When my Afib began I went to see an M.D. My guess is that Dr. Plana is what is now referred to as a cardio-oncologist. He is experienced in both cardiology and oncology. Smart, experienced doctor.
When I asked Dr. Plana if my Afib was caused by my chemotherapy, he was measured in his response simply saying that “yes, the damage you (me) are experiencing is the type of damage that we see resulting from chemotherapy.” My interpretation was that Dr. Plana wasn’t about to directly say that University Hospitals (where I had my cancer treatment) had caused my heart damage.
My point is that if you are undergoing chemotherapy you may develop heart damage now or years from now. The statistics listed below don’t say anything about late stage cancer survivors like me. Survivors that develop chemo-induced cardiomyopathy (CIC) years after their treatment with cardio-toxic chemo.
All of my cardiologists prescribed conventional heart medicines (metoprolol) when I met with each. No discussion of exercise, nutrition or supplementation such as CoQ10.
I’ve come to understand that conventional medicine simply does not think the way I do. Conventional medicine, both cardiology and oncology in this case, follow the instructions of the Food and Drug Administration. And the FDA says to prescribe metoprolol or some other therapy for me.
I have learned that most, if not all, conventional medications, whether chemotherapy or heart meds. have short, long-term and late stage side effects. I do not want to endure any more side effects.
My therapies then, in the case of chronic atrial fibrillation, is to exercise frequently but moderately, eat lots of fruits and veggies and supplement with lots of nutritional supplements that have been shown to enhance heart health.
- CoQ10
- Vitamin D3
- Cocoa
- Magnesium
- Omega-3 fatty acids
- PQQ
- N-acetylcysteine (NAC)
and others. As for my last echocardiogram, my ejection fraction had increased from 40-45 in 2018 to 50-55 in 2019. My blood pressure remains stable (120/80) and I have learned to live with chronic AFib. It feels weird and takes some getting used to but I’m fine now.
I’m not a doctor. I’m just a guy living with chemo-induced cardiomyopathy and chronic AFib. If you’d like more information about this, feel free to post a question or a comment. I will reply to you ASAP.
- Learn more about chemotherapy-induced cardiomyopathy- click now
- To Learn More about chemotherapy-induced atrial fibrillation- click now
Thanks,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director of PeopleBeatingCancer
Recommended Reading:
- Atrial Fibrilation-Catheter Ablation More Popular But Complications Rise
- Cardiac Rehab with Magnesium
- Can Atrial Fibrillation (AFIB) Patients Have Sex?
- Risk of Sudden Cardiac Death among Atrial Fibrillation Patients (me)
What is atrial fibrillation?
“Atrial fibrillation, often called AFib or AF, is the most common type of treated heart arrhythmia. An arrhythmia is when the heart beats too slowly, too fast, or in an irregular way.
When a person has AFib, the normal beating in the upper chambers of the heart (the two atria) is irregular, and blood doesn’t flow as well as it should from the atria to the lower chambers of the heart (the two ventricles). AFib may happen in brief episodes, or it may be a permanent condition….
Facts About AFib
It is estimated that 12.1 million people in the United States will have AFib in 2030.1,2
- In 2018, AFib was mentioned on 175,326 death certificates and was the underlying cause of death in 25,845 of those deaths.3
- People of European descent are more likely to have AFib than African Americans.
- Because the number of AFib cases increases with age and women generally live longer than men, more women than men experience AFib.
How is AFib related to stroke?
AFib increases a person’s risk for stroke. When standard stroke risk factors were accounted for, AFib was associated with a four- to fivefold increased risk of ischemic stroke.6 AFib causes about 1 in 7 strokes.7
Strokes caused by complications from AFib tend to be more severe than strokes with other underlying causes. Strokes happen when blood flow to the brain is blocked by a blood clot or by fatty deposits called plaque in the blood vessel lining.
How is AFib treated?
Treatment for AFib can include
- Medicines to control the heart’s rhythm and rate
- Blood-thinning medicine to prevent blood clots from forming and reduce stroke risk
- Surgery
- Medicine and healthy lifestyle changes to manage AFib risk factors
What are the consequences of AFib?
More than 454,000 hospitalizations with AFib as the primary diagnosis happen each year in the United States.4 The condition contributes to about 158,000 deaths each year.3 The death rate from AFib as the primary or a contributing cause of death has been rising for more than two decades.7
Introducing a new entity: chemotherapy-induced arrhythmia
“We reviewed published reports on chemotherapy-induced arrhythmias in English using the PubMed/Medline and OVID databases from 1950 onwards as well as lateral references.
Arrhythmias were reported as a side effect of many chemotherapeutic drugs. Anthracyclines are associated with atrial fibrillation (AF) at a rate of 2–10%, but rarely with ventricular tachycardia (VT)/fibrillation…
Arrhythmias induced by 5-fluorouracil, including VT, are mostly ischaemic in origin and usually occur in the context of coronary spasm produced by this drug.
Cisplatin—particularly with intrapericardial use—is associated with a very high rate of AF (12–32%).
Melphalan is associated with AF in 7–12% of cases, but it does not appear to cause VT. Interleukin-2 is linked to frequent arrhythmia, mostly AF…
Many cardiology consultations in cancer centres are generated by arrhythmias, which occur in two major settings: after surgery and after chemotherapy. Although post-operative arrhythmias—mostly atrial fibrillation (AF)—are a recognized entity, the relationship between chemotherapy and arrhythmias is not well established…
Another difficulty comes from the fact that, as a rule, more than one chemotherapeutic agent is used in each patient. Multiple chemotherapeutic drugs are administered simultaneously, making it difficult to decide which one caused this adverse effect…
Findings based on individual drugs:
- Anthracyclines
- Antimicrotubule agents
- Antimetabolites
- 5-Fluorouracil
- Capecitabine
- Gemcitabine
- Cytarabine
- Alkylating agents
- Cisplatin
- Melphalan
- Cyclophosphamide
- Tyrosine kinase inhibitors
- Arsenic trioxide
- Thalidomide
- Histone deacetylase inhibitors
- Amsacrine
- Interleukin-2
Sudden death with documented or suspected ventricular arrhythmias has been reported with almost all classes of chemotherapeutic drugs but rarely…
In general, chemotherapy-induced arrhythmia is an existing but poorly recognized and studied entity. Studies with prospective data collection and thorough analyses will be needed to establish a causal relationship between certain anticancer drugs and arrhythmias…”