
Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- Skin Cancer »
- Clearing Facial Actinic Keratosis-
Clearing Facial Actinic Keratosis-
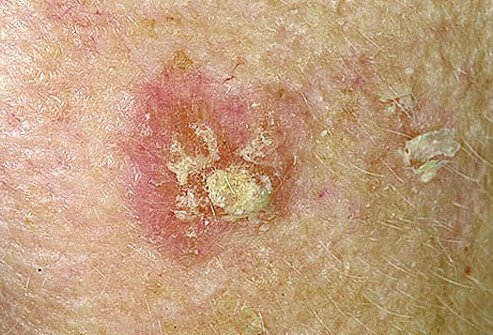
“High-dose VD3 supplementation (group 2) significantly improved the overall Actinic Keratosis lesion response (72.5% ± 13.6%) compared with that in group 1..”
Let’s be honest. Facial Actinic Keratosis is unsightly. AK is not skin cancer. It is pre-skin cancer. A stage before diagnoses of non-melanoma skin cancer- Squamous cell or Basal cell. The issue is that
- AK’s can become skin cancer (melanoma) and
- AK’s can look unsightly, especially one’s on the face. AK’s are generally dry patchy skin. I had several small AK patches on my face and bald pate (bald head) and chose to go to my dermatologist and get them removed.
After a diagnosis of an incurable blood cancer called multiple myeloma in 1994, induction and a stem cell transplant- I learned that I had an increased risk of skin cancer. I also sat in the sun way too often as a teen. Burning one’s skin also increases one’s risk of a diagnosis of skin cancer.
I am now all about skin health. The skin cancer guide at the top of this page outlines evidence-based but non-toxic, non-conventional therapies. Vitamin D3 supplementation has been shown to reduce the risk of a skin cancer diagnosis.
According to the study linked and excerpted below, vitamin D3 supplementation in advance of “blue light photodynamic therapy” improves the clearance of AK on the face.
Vitamin D3 supplementation is discussed frequently in my world. I mention this simply to clarify that vitamin D3 is less about how much you take daily and more about the amount you have in your blood. The study below cites VD3 deficiency (25-hydroxyvitamin D) level < 31 ng/dL. And normal blood levels of vitamin D3 as being above that.
I supplement with D3 daily and my blood levels are usually about 40 ng/dl.
Whether you undergo therapies such as nutrition, lifestyle or nutritional supplementation, an ounce of prevention really is worth a pound of cure as the saying goes.
If you have any questions or comments, please scroll down the page, write a post and I will reply to you ASAP.
Thank you for your time and attention,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Non-Melanoma Skin Cancer Risk Increases From Radiation
- Preventing Non-Melanoma Skin Cancer Relapse
- How to Identify Skin Cancer in 5 Steps
- Skin Cancer, Vitamin D3 and Sunlight
Significant improvement of facial actinic keratoses after blue light photodynamic therapy with oral vitamin D pretreatment: An interventional cohort-controlled trial
“In mouse models of skin cancer, high-dose oral vitamin D3 (VD3; cholecalciferol) combined with photodynamic therapy (PDT) can improve the clearance of squamous precancers (actinic keratoses [AKs])…
The baseline lesion counts and serum 25-hydroxyvitamin D3levels were determined. In group 1, 29 patients underwent gentle debridement and 15-minute aminolevulinic acid preincubation with blue light (30 minutes; 20 J/cm2). In group 2, 29 patients took oral VD3 (10,000 IU daily for 5 or 14 days) prior to debridement and PDT. Lesion clearance was assessed at 3 to 6 months…
In group 1, the mean clearance rates of facial AK were lower in patients with VD3 deficiency (25-hydroxyvitamin D3 level < 31 ng/dL; clearance rate, 40.9% ± 42%) than in patients with normal 25-hydroxyvitamin D3 levels (62.6% ± 14.2%).
High-dose VD3 supplementation (group 2) significantly improved the overall AK lesion response (72.5% ± 13.6%) compared with that in group 1 (54.4% ± 22.8%). No differences in side effects were noted.
Immediately following treatment, the area may be red, swollen, tender, and mildly bruised or blistered, especially when medication has been applied to the skin. The treated area may crust over or peel, but this is considered normal. Most people heal within 7 days, and the crusting resolves within 3 to 14 days.
If light-sensitive drugs are used for photodynamic therapy, as is the case in most cases, your skin will be very sensitive to light for several weeks after the procedure. Try to avoid bright, direct sunlight, though fluorescent lights are fine. Sunscreens won’t be effective, because they protect from UV light and not photosensitivity reactions.
When used properly, there are no significant long-term side effects of blue light therapy treatment. It’s much less invasive than surgery, and there’s usually either little or no scarring after the treated site heals.
Blue light therapy on its own, without the photosensitivity drugs added, is safe and has very few risks. The biggest risk is for a potential skin infection if any post-treatment blisters occur and are popped or not cared for.
You shouldn’t have blue light therapy if you have a rare condition called porphyria, which is a disorder of the blood that leads to heightened light sensitivity, or if you have allergies to porphyrins. You also shouldn’t use this therapy if you have lupus.
Photodynamic therapy for cancer treatment, however, may come with more potential risks and complications depending on the area of treatment. Swelling in the area of treatment, for example, can cause trouble breathing. If you experience these symptoms, seek emergency medical attention.
Blue light therapy is a painless, noninvasive procedure that can be used to treat different conditions in an outpatient environment. It has limited long-term side effects, and only a few mild, immediate side effects.
When photosynthesizing drugs are added, photodynamic therapy can be an effective alternative therapy for cancer that’s found beneath the skin, too.
To prepare your home for the days following your procedure, you can close the curtains before you leave so you’ll be limiting the amount of light that affects your skin. Avoid making plans that will require you to be outdoors immediately following treatment, and keep the area clean with soap and water.”


