Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
Financial Cost of DCIS Got You Worried? Read This

The cost of early stage breast cancer (DCIS) therapy is a concern that influences treatment decisions for many women, even when they have insurance and higher income…
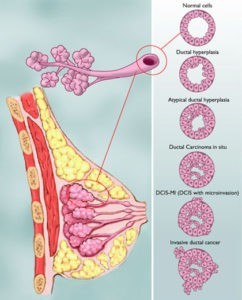
Though Ductal Carcinoma In-situ (DCIS) is not cancer it can be both scary and expensive. This diagnosis of “pre-breast cancer” or “breast cancer stage one” has a 10 year average survival rate of 98% but it increases your risk of a diagnosis of invasive breast cancer from 20% to 50% depending the study you read.
Your oncologist will probably recommend the standard-of-care treatment-surgery, local radiation and an aromatase inhibitor (tamoxifen) a type of chemotherapy. All three therapies have risks. All three therapies can cost thousands of dollars.
While I encourage all DCIS patients to listen carefully to their oncologists and proceed with that conventional therapy plan that feels right to you I also encourage you to add evidence-based, non-toxic, complementary therapies to your therapy plan.
Evidence-based, non-toxic therapies shown to reduce the risk of breast cancer or reduce the risk of DCIS becoming full-blown breast cancer.
Most importantly, understanding both the cost of a procedure and the therapeutic effect of that procedure on your future risks. Meaning, for example, a lower dose and shorter course of tamoxifen can still reduce the future risk of invasive breast cancer while reducing side effects and cost. Or the cost/benefit comparing a lumpectomy versus a mastectomy.
If you have been diagnosed with DCIS and would like to learn more about evidence-based, non-toxic therapies to reduce your risk of invasive breast cancer, scroll down the page, post a question or comment and I will reply to you ASAP.
Thank you,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Is it “you have cancer” or “you have IDLE?” Prevent Cancer Overtreatment
- Slash Your Breast Cancer Risk of Relapse Now!
- Breast Cancer Integrative Therapy Plan
Affluent, Insured, and Worried About Cancer Costs
“The cost of early stage breast cancer therapy is a concern that influences treatment decisions for many women, even when they have insurance and higher income than most Americans, a new survey suggests.
The 607 survey participants all had a history of breast cancer or ductal carcinoma in situ (stage 0-III). The majority had private insurance (70%) or Medicare (25%) and a higher annual household income (≥ $74,000) than the general US population.
Despite this relatively empowered socioeconomic status among participants, nearly half (43%) reported considering costs when making treatment decisions. Furthermore, 40% wanted their physicians to think about costs when making medical recommendations.
The survey participants also overwhelmingly reported that they wanted to understand costs prior to treatment (79%), report the study authors, led by Rachel Adams Greenup, MD, MPH, of Duke University Medical Center in Durham, North Carolina.
The study revealed this rarely happened, with 78% of the women saying that costs were never discussed with their caregivers…
Details of the Survey
The group was relatively young (median age at diagnosis, 49.6 years) and median time from diagnosis was 6.7 years.
Median reported out-of-pocket (OOP) costs were $3500. However, 25% had OOP costs ≥ $8000, 10% had OOP costs ≥ $18,000, and 5% had OOP costs ≥ $30,000.
The survey also asked women to characterize their financial burden as none, slight, somewhat, significant, and catastrophic. A total of 15.5% chose significant or catastrophic to describe their financial burden.
In view of the survey population’s demographics (insured, educated, and white), it is likely that other American women have an even greater risk of financial harm, according to ASCO.
In the study, women were more likely to report financial harm if they had bilateral mastectomy vs lumpectomy (odds ratio [OR], 1.9; P = 0.03), greater stage at diagnosis (stage 3 vs 0; OR, 3.9; P < 0.01), and discussed costs during the clinical encounter (OR, 2.3; P < 0.01).
Women who reported discussing costs were more likely to be stage 2 or 3 (56% vs 40%; P = 0.02), less likely to be depressed (24% vs 30%; P = 0.03), and had less insurance coverage (trend P = 0.02) compared with those who did not.
The researchers reported that decreased risk of financial harm was associated with older age (OR, 0.95; P < 0.01), increasing household income (overall P < 0.001), better insurance coverage (OR, 0.5; P < 0.001), and longer time since diagnosis (OR, 0.65; P < 0.001).
Greenup believes that knowing the price of treatments might be a clinical boon. “Cost transparency could improve the quality of treatment decisions patients make and has the potential to reduce the risk of financial harm,” she said in a Duke press statement…
The now ubiquitous term financial toxicity was coined in 2013 by Amy Abernethy, MD, PhD, who was a medical oncologist at the Duke Cancer Institute at the time. The term describes an “adverse event” increasingly experienced by patients with cancer, she and a colleague explained.