A total of 40 randomized trials comparing 18 interventions in 9 categories were identified and included in the study. A meta-analysis of mostly low-risk BCC patients was then conducted…”
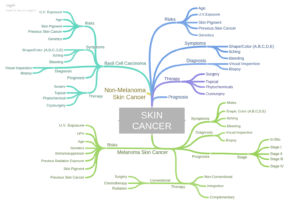
Non-melanoma skin cancer, specifically basel cell carcinoma (BCC) combined with squamous cell carcinoma (SCC) total more than 3 million diagnoses annually in the U.S. NMSC’s strength is also it’s weakness. The risk of either BCC or SCC developing into melanoma, a serious form of cancer, is quite low. As the study linked and excerpted below explains, this fact encourages BCC patients to gravitate toward therapies that are cosmetic more than curative.
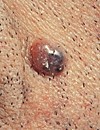
Mohs surgery is the “gold standard” for removing an unsightly BCC because it is more about physical appearance post-surgery, rather than reducing the risk of relapse. At least that’s what my 90 year old mom would tell you.
My mom spend a lifetime gardening, playing tennis, walking out doors, generally enjoying Cleveland, Ohio sunshine. I mention where we live because there less sunshine in Cleveland, Ohio compared to much of the rest of the United States.
Mom’s skin cancers, mostly basel cell carcinomas, began appearing in her late sixties. Like many of mom’s peers, the appearence of BCC’s or SCC’s were normal, almost expected. Sure, these freckle/moles were cancer but not cancers like breast or prostate cancer… No one ever died from skin cancer, right?
Please don’t misunderstand me. I’m not dissing my mom in any way. I too had a BCC removed from my face. Being a cancer survivor with an increased risk of skin cancer I worried about this cancer more than my mom worried about her skin cancers but I understand her thinking.
The takeaway from the article linked below in my opinion, is that non-melanoma skin cancers have a variety of therapies that are basically equal when it comes to treatment, however none are curative however. The key is more about reducing your risk of relapse than curing your cancer.
In addition to a person’s genetic make-up, he or she can be susceptable to BCC due to a number of lifestyle factors. In addition to spending lots of time in the sun, mom used to smoke. It is no wonder to me that she has had many BCC’s removed.
As a cancer survivor and cancer coach who has an increase risk of non-melanoma skin cancer I live an anti-BCC lifestyle based on nutrition, supplementation and other evidence-based therapies shown to reduce my risk of both BCC and SCC.
To Learn More About Basal Cell Carcinoma- click now
Have you been diagnosed with NMSC? Scroll down the page, post a question or a comment and I will reply to you ASAP.
Thank you,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
“Individuals who develop frequent basal cell carcinomas (BCCs) may have an increased prevalence of germline mutations in DNA repair genes as well as an increased malignancy risk…
Selecting the right therapy for BCC is challenging and should be based on many variables, including patient factors, tumor factors, and patient access to healthcare resources…
Limited knowledge of BCC treatments could straddle payers with more costly interventions that are not evidence-based, wrote the researchers. The purpose of their analysis was to assess what has been elucidated regarding the safety and efficacy of various BCC treatments by mining various English-language databases for comparative studies.
A total of 40 randomized trials comparing 18 interventions in 9 categories were identified and included in the study. A meta-analysis of mostly low-risk BCC patients was then conducted…
Drucker and colleagues found that the estimated recurrence rates were comparable for:
- excision,
- Mohs surgery,
- curettage and diathermy, and
- external beam radiation.
However, the recurrence rates were increased for cryotherapy, curettage and cryotherapy, 5-fluorouracil, imiquimod, and photodynamic therapy with either methyl-aminolevulinic acid or aminolevulinic acid...
A host of unavoidable and highly individualized confounders contribute to the development of non-melanoma skin cancer such as BCC, Savory added. Risk factors, such as
- skin type,
- genetic predisposition to photodamage,
- history of cigarette smoking,
- history of indoor tanning, and
- outdoor activities,
can influence skin cancer risk, she explained…
“The comparison of conventional surgery with Mohs micrographic surgery is flawed because Mohs is tissue-conserving by nature, which leads to superior cosmetic results for a given tumor,” he said. “The meta-analysis examined only low-risk superficial and nodular BCC. More aggressive subtypes are best treated with Mohs micrographic surgery, and this is widely regarded as the gold standard…”





