Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Hyperkeratosis Leukoplakia- Reduce Risk of Oral Cancer
Hyperkeratosis Leukoplakia- Reduce Risk of Oral Cancer
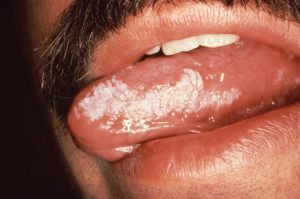
Hyperkeratosis is thickening of the stratum corneum (the outermost layer of the epidermis, or skin), often associated with the presence of an abnormal quantity of keratin,[1]
Hello David- I’ve been diagnosed with Hyperkenois (HYPERKERATOSIS) Leukoplakia for the past 4 years around 2 teeth on the gums. My Doctor removed some of the tissue during a biopsy of the leukoplakia but the white area continues to return.
I am 57 and and gave up smoking 20 years ago. I did drink moderately. The biopsy has been normal but now atypical cells were found.
I’ve been to an Ear, Nose and Throat doctor and he has recommended I take a “wait and see” approach. The ENT doctor does as not want to remove teeth at this stage.
I’ve always eaten healthy but I did drink. I take many vitamins as well. Any suggestions other then stopping alcohol to prevent the area from getting worse. Thank you. Kind regards. Dan
Hi Dan,
For the purposes of this reply, I am going to assume that you meant hyperkeratosis and not hyperkenois. Hyperkeratosis is associated with leukoplakia and makes more sense.
That said, please keep in mind that your diagnosis is pre-cancer and not malignant cancer. Serious to be sure, but your primary goal is to make sure that your pre-cancer does not become full-blown cancer.
Your efforts thus far are already reducing your risk of cancer.
- Quitting smoking
- nutritious eating, and
- nutritional supplementation
are all good. You are reducing your risk of an oral cancer diagnosis.
According to the articles linked below, you can reduce your risk of an oral cancer diagnosis even more by:
- urea containing creams
- carbon dioxide laser.
- curcumin, green tea extract supplementation
The bottom line is that you are already taking steps to reduce your risk of oral cancer and you can reduce your risk even further if you chose to.
To Learn More about non-toxic Leukoplakia therapies- click now
Let me know if you have any questions.
Hang in there,
David Emerson
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Hyperkeratosis
“Hyperkeratosis is thickening of the stratum corneum (the outermost layer of the epidermis, or skin), often associated with the presence of an abnormal quantity of keratin,[1] and also usually accompanied by an increase in the granular layer. As the corneum layer normally varies greatly in thickness in different sites, some experience is needed to assess minor degrees of hyperkeratosis…
It can be treated with urea-containing creams, which dissolve the intercellular matrix of the cells of the stratum corneum, promoting desquamation of scaly skin, eventually resulting in softening of hyperkeratotic areas.[3]
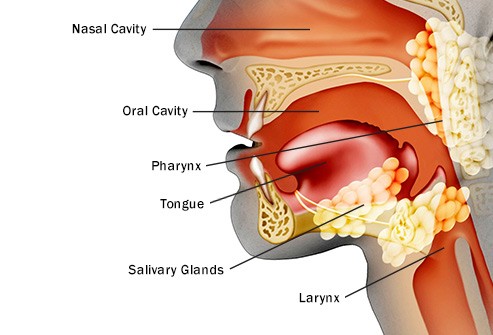
In mucous membranes[edit]
The term hyperkeratosis is often used in connection with lesions of the mucous membranes, such as leukoplakia. Because of the differences between mucous membranes and the skin (e.g. keratinizing mucosa does not have a stratum lucidum and non keratinizing mucosa does not have this layer or normally a stratum corneum or a stratum granulosum), sometimes specialized texts give slightly different definitions of hyperkeratosis in the context of mucosae. Examples are “an excessive formation of keratin (e.g., as seen in leukoplakia)”[12] and “an increase in the thickness of the keratin layer of the epithelium, or the presence of such a layer in a site where none would normally be expected.”[13]
White Oral Lesions: How to Distinguish the Benign From the Deadly
“Chronic irritation from smoking is the most common cause of white mucosal lesions. Because benign leukoplakic growths are virtually impossible to distinguish from carcinoma, biopsy is essential…
LEUKOKERATOSIS, HYPERKERATOSIS, AND LEUKOPLAKIA
The term “leukokeratosis” is often used generically to describe any white, plaquelike lesion of the oral cavity. “Leukoplakia” is similarly applied by some authors.6 Others reserve the term “leukoplakia” for lesions that show dyskeratosis on histologic examination…
Leukokeratosis, which can arise at any site in the oral cavity, occurs most often on the buccal mucosa and least often on the soft palate and gingiva (Figure 1). Peak incidence is in midlife, and men are more frequently affected. The lesions are generally asymptomatic, although patients may occasionally complain of burning or an area of roughness. In most cases, the lesion is discovered during a routine physical or dental examination…
Always attempt to identify and eliminate the irritant that caused the lesion. Many lesions involute when this is done, but new ones may appear. Periodic follow-up examination and repeated biopsy are essential. If oral disease is widespread, sample multiple areas…
- Hyperkeratosis (thickening of the outer keratin layers),
- parakeratosis (persistence of pyknotic nuclei in the outer epithelial layer),
- acanthosis (enlargement or edema of the spinous layer of the skin), and
- dyskeratosis
may be seen…
Treatment. After biopsy, residual lesions may be destroyed with a carbon dioxide laser…