- You are here:
- Home »
- Blog »
- non-conventional therapies »
- Leukoplakia- Prevent Oral, Mouth Cancer?
Leukoplakia- Prevent Oral, Mouth Cancer?
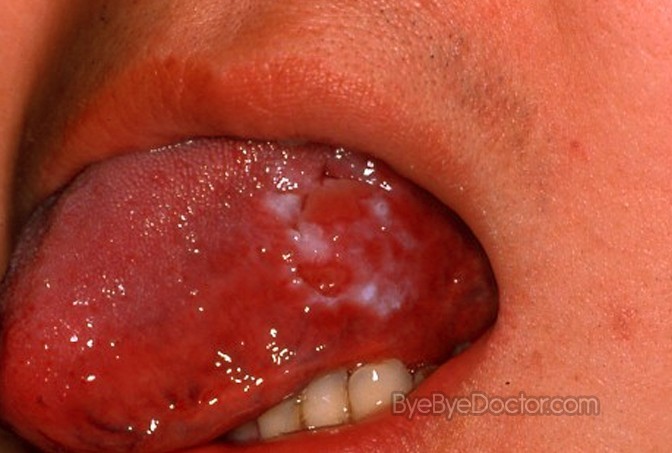
“Leukoplakia is a firmly attached white patch on a mucous membrane which is associated with an increased risk of (oral) cancer.[4][5] …”
Hi. I used to smoke. I smoked daily for about 6 to 8 years. The last two or three years I smoked a pack a day. I stopped at age 34 when I developed Leukaplakia and some Erythoplakia lesions on my tongue. I am hoping to not develop mouth cancer, oral cancer.
I have been taking Vitamin A, tumeric/curcumin and now green tea extract. I eat as much vitamin A rich fruits and vegetables as I can to try to regress the leukaplakia. I am going back to the doctor to see what I can do.
I had a biopsy 5 to 6 months ago and it came back benign. Any tips for reducing the leukaplakia? I read so many things you shouldn’t eat or drink and it’s always difficult because some antioxidant fruits are acidic and acidic isn’t good for lesions. Any help would be appreciated. Thanks- Jordan
Hi Jordan,
Several things. First of all, I am sorry for your leukoplakia and erythoplakia diagnoses. Leukoplakia and europlakia are pre-cancers. Or I should say that leukoplakia and erythoplakia are lesions that, according to research, can become a cancer called oral or mouth cancer.
I’ve tried to address your questions below. Let me know if you have any other questions.
If you have:
- stopped smoking, the probably cause of your pre-cancer diagnosis (tobacco) and
- you have had a biopsy that came back negative indicating your pre-cancer did not become cancerous (see the article linked below)
- you have surgically removed the leukoplakia and erythoplakia,
my understanding is that you have reduced your low risk of leukoplakia and erythoplakia from becoming full-blown oral cancer. Meaning, your lesions were pre-cancer. Leukoplakia and Erythoplakia are pre-cancer not cancer. The issue is pre-cancer becoming full-blown cancer.
According to research you cannot eliminate your risk of oral cancer completely. Therefore, you should see your doctor regularly to check on the leukoplakia and erythoplakia.
Examples of other types of pre-cancer are:
- colon polyps,
- barrett’s esophagus,
- non-melanoma skin cancers (freckles),
- DCIS (ductal carcinoma in-situ- pre-breast cancer),
- many others.
The risk is if the pre-cancerous lesion becomes a full-blown cancer diagnosis.
In the case of colon polyps, for example, the person can surgically remove the polyp therefore eliminating his/her risk of the polyps becoming colon cancer. DCIS is surgically removed by “lumpectomy” eliminating the risk of that lesion becoming cancerous.
Your consumption of fruits, veggies, curcumin, green tea extract should, according to research, reduce your risks or oral cancer further. I realize that you did not specify surgically removing your L and E but I am going to assume that you did.
According to the articles linked below, the other factor to reduce your risk further is to reduce or eliminate alcohol consumption.
I hope I have addressed your concerns and answered your questions. Let me know if you have any questions.
Hang in there,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Green Tea Extract, Curcumin and Leukoplakia
- Oral Submucous Fibrosis Identification and Therapy
- Head & Neck Cancer- An Integrative Therapy no-brainer-
Leukoplakia
“Leukoplakia is a firmly attached white patch on a mucous membrane which is associated with an increased risk of (oral) cancer.[4][5] …
The cause of leukoplakia is unknown.[6] Risk factors for formation inside the mouth include smoking, chewing tobacco, excessive alcohol, and use of betel nuts.[4][7] …
It is a precancerous lesion, a tissue alteration in which cancer is more likely to develop.[4] The chance of cancer formation depends on the type, with between 3–15% of localized leukoplakia and 70–100% of proliferative leukoplakia developing into squamous cell carcinoma.[4]—
Treatment recommendations depend on features of the lesion.[4] If abnormal cells are present or the lesion is small surgical removal is often recommended; otherwise close follow up at three to six month intervals may be sufficient.[4]People are generally advised to stop smoking and limit the drinking of alcohol.[3] In potentially half of cases leukoplakia will shrink with stopping smoking;[5] however, if smoking is continued up to 66% of cases will become more white and thick.[6] The percentage of people affected is estimated at 1–3%.[4]
Management[edit]
A systematic review found that no treatments commonly used for leukoplakia have been shown to be effective in preventing malignant transformation. Some treatments may lead to healing of leukoplakia, but do not prevent relapse of the lesion or malignant change.[8] Regardless of the treatment used, a diagnosis of leukoplakia almost always leads to a recommendation that possible causative factors such as smoking and alcohol consumption be stopped,[35] and also involves long term review of the lesion,[35] to detect any malignant change early and thereby improve the prognosis significantly….
Predisposing factors and review[edit]
Beyond advising smoking cessation, many clinicians will employ watchful waiting rather than intervene. Recommended recall intervals vary. One suggested program is every 3 months initially, and if there is no change in the lesion, then annual recall thereafter. Some clinicians use clinical photographs of the lesion to help demonstrate any changes between visits. Watchful waiting does not rule out the possibility of repeated biopsies.[3] If the lesion changes in appearance repeat biopsies are especially indicated.[2]
Precancerous lesions of oral mucosa
“Precancerous lesions of oral mucosa, known as potentially malignant disorders in recent years, are consists of a group of diseases, which should be diagnosed in the early stage. Oral leukoplakia, oral submucous fibrosis, and oral erythroplakia are the most common oral mucosal diseases that have a very high malignant transformation rate….”
“Oral cancer, also known as mouth cancer, is cancer of the lining of the lips, mouth, or upper throat.[6] In the mouth, it most commonly starts as a painless white patch, that thickens, develops red patches, an ulcer, and continues to grow. When on the lips, it commonly looks like a persistent crusting ulcer that does not heal, and slowly grows.[7] …
Risk factors include tobacco and alcohol use.[9][10] With both tobacco and drinking alcohol, the risk of oral cancer is 15 times greater.[11] Other risk factors include HPV infection,[12] chewing paan,[13] and sun exposure on the lower lip.[14] Oral cancer is a subgroup of head and neck cancers.[6] Diagnosis is made by biopsy of the concerning area, followed by investigation with CT scan, MRI, PET scan, and examination to determine if it has spread to distant parts of the body…
Causes
Oral squamous cell carcinoma is a disease of environmental factors, the greatest of which is tobacco. Like all environmental factors, the rate at which cancer will develop is dependent on the dose, frequency and method of application of the carcinogen (the substance that is causing the cancer).[20] Aside from cigarette smoking, other carcinogens for oral cancer include alcohol, viruses (particularly HPV 16 and 18), radiation, and UV light.[7]
Tobacco
Tobacco is the greatest single cause of oral and pharyngeal cancer. It is a known multi-organ carcinogen, that has a synergistic interaction with alcohol to cause cancers of the mouth and pharynx by directly damaging cellular DNA.[20] Tobacco is estimated to increase the risk of oral cancer by 3.4[20]–6.8[9] and is responsible for approximately 40% of all oral cancers.[21]
Premalignant lesions
Oral leukoplakia (white patch) on the left tongue. Proven to be severe dysplasia on biopsy
A premalignant (or precancerous) lesion is defined as “a benign, morphologically altered tissue that has a greater than normal risk of malignant transformation.” There are several different types of premalignant lesion that occur in the mouth. Some oral cancers begin as white patches (leukoplakia), red patches (erythroplakia) or mixed red and white patches (erythroleukoplakia or “speckled leukoplakia”).