Leave a Comment:
1 comment
[…] Melanoma Survivors Risk Secondary Cancers […]
Reply
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
Identifying a problem is easy. Identifying a problem AND a solution is much more difficult. Giving the solution that the study below gives, “melanoma survivors should remain under surveillance not only for recurrence but also for future primary melanomas and other cancers…,” is not a real solution. Advising cancer survivors to get checked for other cancers really carefully is hardly being helpful…
I am both a cancer survivor and cancer coach. Two of my therapies for my first cancer diagnosis, radiation and an autologous stem cell transplant, increased my risk of skin cancer. Further, I was a sun worshiper in my youth. Lots of us were. We didn’t know that repeated sunburns and blistering would be a real problem later in life.
I had a basel cell carcinoma removed from my face a few years ago. I have six of the skin cancer risks listed below. Fortunately I live an evidence-based, non-conventional lifestyle to reduce my risk of a second cancer. You can too.
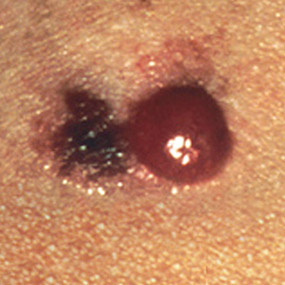
The study linked and excerpted below explains that melanoma survivors have their risk of a second cancer (referred to as a “secondary primary cancer”) increase by 28% over people who never been diagnosed with melanoma. 28% is a substantial increase.
To be clear, when the study talks about skin cancer patients getting another skin cancer, they are talking about a skin cancer different from the first skin cancer.
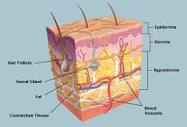
Melanoma at a glance-
The bottom study linked below explains that immunotherapy can increase this already increased risk of second primary cancer after a melanoma diagnosis.
Have you been diagnosed with skin cancer? Have you been diagnosed with a secondary primary cancer such as breast or prostate cancer as well? Scroll down the page, post a question or a comment and I will reply to you ASAP.
Thank you,
“Objective– To quantify the risk of subsequent primary cancers among patients with primary cutaneous malignant melanoma….
Of the patients diagnosed, 10 857 (12.1%) developed 1 or more subsequent primary cancers. The overall risk of a subsequent primary cancer increased by 28%…
Although melanoma is a potentially lethal form of skin cancer, survival rates are high, with a 5-year survival rate of 92.3% and 86.9% for white women and men, respectively.2 Hence, the risk of subsequent cancer is an important issue for melanoma survivors.
Conclusions- Melanoma survivors have an approximately 9-fold increased risk of developing subsequent melanoma compared with the general population. The risk remains elevated more than 20 years after the initial melanoma diagnosis. This increased risk may be owing to behavioral factors, genetic susceptibility, or medical surveillance. Although the percentage of subsequent primary melanomas thicker than 1 mm is lower than for the first of multiple primary melanomas, it is still substantial. Melanoma survivors should remain under surveillance not only for recurrence but also for future primary melanomas and other cancers.
“Question When compared with prior therapies, are immune checkpoint inhibitors for metastatic melanoma associated with development of second primary cancers?
Findings In this cohort study of 5016 patients with metastatic melanoma between 2005 and 2016, the overall risk of second primary cancers increased after the introduction of immune checkpoint inhibitors. Risks for cancer of the small intestine and myeloma were higher than before the era of immune checkpoint inhibitors.
Meaning In this study, a change in the incidence of second primary cancers was found; screening for these cancers may be warranted in patients treated with immune checkpoint inhibitors for metastatic melanoma.
Importance To date, the risk of developing second primary cancers (SPCs) after the first primary melanoma has not been studied in the era of immune checkpoint inhibitors (ICIs).
Objective To assess differences in the risk of SPCs in patients with primary melanoma before (2005-2010) and after (2011-2016) the introduction and approval of ICIs.
Design, Setting, and Participants Population-based cohort study using the Surveillance, Epidemiology, and End Results database from January 2005 to December 2016 of patients diagnosed with metastatic melanoma. Data were analyzed from January 4 to June 30, 2020.
Exposures Receipt of immunotherapy or other anticancer agents.
Main Outcomes and Measures The primary outcome was the development of second primary cancers in patients with melanoma. Standardized incidence ratios (SIRs) were calculated for the development of SPCs before and after the introduction of ICIs.
Results Among 5016 patients with diagnosed metastatic melanoma, 2888 (58%) were younger than 65 years at the time of diagnosis, and 3441 (69%) were male. From 2005 to 2010, SIRs were 3.24 (95% CI, 0.08-18.04) for small intestine cancer, 1.93 (95% CI, 1.14-3.05) for lung and bronchus cancer, 2.77 (95% CI, 1.02-6.03) for kidney cancer, and 7.29 (95% CI, 2.93-15.02) for myeloma. From 2011 to 2016, SIRs were 9.23 (95% CI, 1.12-33.35) for small intestine cancer, 1.54 (95% CI, 0.71-2.93) for lung and bronchus cancer, 2.66 (95% CI, 0.73-6.82) for kidney cancer, and 5.90 (95% CI, 1.61-15.10) for myeloma. The overall risk of developing SPCs in individuals who survived the first primary melanoma was 65% higher (SIR, 1.65; 95% CI, 1.35-2.00) in the pre-ICIs period and 98% higher (SIR, 1.98; 95% CI, 1.57-2.45) in the post-ICIs period than the overall cancer incidence rate in the general population.
Conclusions and Relevance In this study, an increase in the overall risk of second primary cancers after melanoma after the introduction of immune checkpoint inhibitors was observed. The pattern of SPCs has been altered in the era of systemic therapy. Close monitoring and screening for SPCs may be warranted in patients with metastatic melanoma.
[…] Melanoma Survivors Risk Secondary Cancers […]
Reply