Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- Skin Cancer »
- Metastatic Melanoma- Surgery Must be Part of the Plan
Metastatic Melanoma- Surgery Must be Part of the Plan
Median Overall Survival was Superior in Surgical vs Nonsurgical Patients with Metastatic Melanoma
A diagnosis of melanoma skin cancer largely depends on your stage of diagnosis. It is when a simple diagnosis of melanoma becomes diagnosis of metastatic melanoma (MM) that the patient needs help. A diagnosis of cancer that has metastasized or spread requires a more elaborate therapy plan.
In my research and experience, when conventional oncology has few if any curative therapies, consider combining the best of conventional with evidence-based non-conventional therapies such as:
- Nutrition
- Supplementation
- Lifestyle Therapies
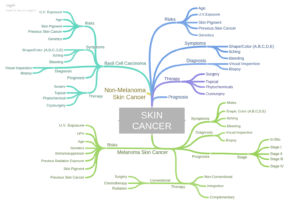
As you can see from the illustration to the left, skin cancer is complicated. Skin cancer that has spread beyond the original site lowers the patient’s five year survival average substantially.
As complicated as MM can be, the article linked and excerpted below clearly states that when MM patients surgically debulk their cancer, they live longer. The study does not say that surgery cures MM patients.
It says that surgery helps MM patients live longer.
That is correct. In this age of elaborate systemic chemotherapy, it is the patient who surgically removes as many mets as possible who lives longer.
I am both a long term cancer survivor and cancer coach. Though my cancer, multiple myeloma, is completely different from Metastatic Melanoma, both cancers are considered to be incurable by conventional oncology. I have remained in complete remission from my incurable cancer since April of 1999 by learning about and pursuing a host of evidence-based, non-conventional therapies.
To learn more about evidence-based, non-conventional therapies for MM, scroll down the page, post a question or comment and I will reply to you ASAP.
Thank you
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Basal Cell Carcinoma Treatment
- Skin Cancer As You Age- Before, During and After Diagnosis
- The “BEST” Treatments for Basel Cell Carcinoma?
Association of Surgical Treatment, Systemic Therapy, and Survival in Patients With Abdominal Visceral Melanoma Metastases, 1965-2014: Relevance of Surgical Cure in the Era of Modern Systemic Therapy.
“Importance: Systemic therapy for metastatic melanoma has evolved rapidly during the last decade, and patient treatment has become more complex.
Objective: To evaluate the survival benefit achieved through surgical resection of melanoma metastatic to the abdominal viscera in patients treated in the modern treatment environment.
Design, setting, and participants: This retrospective review of the institutional melanoma database from the John Wayne Cancer Institute at Providence St Johns Health Center, a tertiary-level melanoma referral center, included 1623 patients with melanoma diagnosed as having potentially resectable abdominal metastases before (1969-2003) and after (2004-2014) advances in systemic therapy.
Main outcomes and measures: Overall survival (OS).
Results: Of the 1623 patients identified in the database with abdominal melanoma metastases, 1097 were men (67.6%), and the mean (SD) age was 54.6 (14.6) years. Of the patients with metastatic melanoma, 1623 (320 [19.7%] in the 2004-2014 period) had abdominal metastases, including 336 (20.7%) with metastases in the gastrointestinal tract, 697 (42.9%) in the liver, 138 (8.5%) in the adrenal glands, 38 (2.3%) in the pancreas, 109 (6.7%) in the spleen, and 305 (18.8%) with multiple sites. Median OS was superior in surgical (n = 392; 18.0 months) vs nonsurgical (n = 1231; 7.0 months) patients (P < .001).
The most favorable 1-year and 2-year OS was seen after surgery for gastrointestinal tract (52% and 41%) and liver (51% and 38%) metastases, respectively. Multivariable analysis found increasing age (hazard ratio [HR], 1.01; 95% CI, 1.00-1.01; P = .02) and the presence of ulceration (HR, 1.21; 95% CI, 1.01-1.45; P = .04) were associated with a worse OS.
Alternatively, treatment with metastasectomy (HR, 0.59; 95% CI, 0.46-0.74; P < .001) and metastases involving the gastrointestinal tract (HR, 0.65; 95% CI, 0.48-0.87; P = .004) were associated with a better OS. The systemic treatment era did not significantly affect outcomes (HR, 0.82; 95% CI, 0.67-1.02; P = .15). Overall, patients with gastrointestinal tract metastases undergoing complete, curative resection derived the greatest benefit, with a median OS of 64 months.
Conclusions and relevance: To our knowledge, this series is the largest single-institution experience with abdominal melanoma metastases, demonstrating that surgical resection remains an important treatment consideration even in the systemic treatment era.”
Dietary compounds and cutaneous malignant melanoma: recent advances from a biological perspective
“Cutaneous malignant melanoma is a heterogeneous disease, being the consequence of specific genetic alterations along several molecular pathways. Despite the increased knowledge about the biology and pathogenesis of melanoma, the incidence has grown markedly worldwide, making it extremely important to develop preventive measures.
The beneficial role of correct nutrition and of some natural dietary compounds in preventing malignant melanoma has been widely demonstrated. This led to numerous studies investigating the role of several dietary attitudes, patterns, and supplements in the prevention of melanoma, and ongoing research investigates their impact in the clinical management and outcomes of patients diagnosed with the disease. This article is an overview of recent scientific advances regarding specific dietary compounds and their impact on melanoma development and treatment…
A great number of studies have been published recently investigating the roles of several dietary compounds in the prevention, development, and therapy of melanoma. Several foods and nutrients have been shown to have protective effects against melanoma-genesis or synergic effects with the medications used for CMM treatment.
Recent literature reviews and data from the World Cancer Research Fund describe the epidemiological aspects of the interactions between diet and melanoma [154, 155]. In the present review, we focused mainly on recent advances regarding the biological mechanisms which lay under such interactions, involving specific compounds of current active research. Numerous encouraging results emerged, alone with conflicting outcomes, especially when basic research data are transferred to humans. This may depend on the heterogeneity of the compounds studied, their concentration, preparation, and administration, as well as on the heterogeneity of the methodological approaches and laboratory techniques employed. Further studies, at both the basic research and epidemiological level, performed with standardized approaches are needed to better comprehend the value of a wide range of nutrients in the prevention and clinical management of melanoma.”