Diagnosed with SMM, SPB, or MGUS?
Learn how you can stall the development of full-blown Multiple Myeloma with evidence-based nutritional and supplementation therapies.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- Pre-Myeloma »
- MGUS- Kidney, Bone, Blood, Skin Damage
MGUS- Kidney, Bone, Blood, Skin Damage
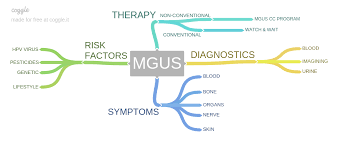
For people with MGUS, there is an increased incidence of fracture, kidney damage, bacterial infections and thromboembolic complications aka blood clots-
I must be slow. I don’t understand the study linked below. Study after study refers to MGUS as being asymptomatic yet they launch into a lengthy description of all the different health problems that can occur to MGUS patients. The main MGUS symptoms, according to the study below are bone, kidney damage, bacterial infections and blood clots.
For the record, an MGUS patient can have a fracture, a bacterial infection, a blood clot or kidney damage and still be considered MGUS or a low concentration of monoclonal immunoglobulin in serum. CRAB symptoms that come with a full-blown MM diagnosis are, in my experience, more extensive.
The other problem I have with studies that cite all of the different symptoms and health challenges that can occur because of concentration of monoclonal immunoglobulin in serum is that both MGUS and the various symptoms discussed below can be treated with evidence-based but non-toxic therapies.

Variety of dietary supplements, including capsules of Garlic, Evening Primrose Oil; Artichoke Leaf; Olive Leaf; Magnesium and Omega 3 Fish Oil.Selective focus. Taken in daylight.
For example, if a diagnostic test identified that you had both MGUS and thick blood, you could take omega-3 fatty acids, drink lots of water and get a little exercise each day all to reduce your risk of a blood clot.
If you have MGUS as well as osteoporosis/osteopenia, you could take bone strength building nutritional supplements such as vitamin D3, exercise daily (moderately) and eat more green leafy veggies, all non-toxic therapies shown to enhance bone mineral density.
And lastly, to fight bacterial infections with evidence-based, non-toxic therapies you could eat garlic, onions, grapefruit seed extract, vitamin C, ginger and apple cider vinegar. I’ll include moderate, daily exercise to be consistent.
Full transparancy- I have undergone a lot of toxicity in my journey from SBP to MM. A lot. In my thinking, MGUS patients should do, pursue every non-toxic therapy they can because they might need to have chemo or radiation some day.
My experience is that conventional medical doctors turn to FDA approved therapies first before they prescribe exercise, nutrition, etc. I think the other way around. Non-toxic therapies first, toxic second.
The final decision is up to you, the patient. To learn more about evidence-based, non-toxic therapies shown to reduce the risk of not only full-blown MM but also reduce the risk of blood clots, bone damage, kidney damage, etc. scroll down the page, post a question or comment and I will reply to you ASAP.
- To Learn More about Monoclonal Gammopathy of Undetermined Significance (MGUS)- click now
- To learn more about kidney involvement in pre-myeloma stages- click now
- To Learn More about Monoclonal Gammopathy of Skin Significance- click now
Thanks and hang in there,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- MGUS, IP6 and Inositol
- Multiple Myeloma Chemotherapy – Antioxidants Enhance Action
- Smoldering Multiple Myeloma- Early Treatment?
[Monoclonal gammopathy of undetermined significance and asymptomatic multiple myeloma in the year 2014]
“Presence of monoclonal immunoglobulin in serum or urine is a relatively common event affecting about 3.2 % of people over 50. Isolated increase of only one type of free light chain, either κ or λ, is detected in 0.7-0.8 % of people over 50.
Most people with monoclonal immunoglobulin meet the criteria of the so-called “mono-clonal gammopathy of undetermined significance (MGUS)”. MGUS is defined by-
- concentration of monoclonal immunoglobulin in serum < 30 g/l,
- number of plasma cells in the bone marrow < 10 % and
- the absence of symptoms of multiple myeloma and other lymphoproliferative diseases.
A proportion of people with MGUS gradually progresses from asymptomatic into symptomatic myeloma or other malignant lymphoproliferative disease requiring treatment. Therefore, MGUS is considered to be one of the most common premalignant conditions with an average risk of transformation into malignant disease of 1 % per year.
Monoclonal gammopathy of IgG and IgA subtype can develop into multiple myeloma. Light chain monoclonal gammopathy can develop not only into light chain multiple myeloma but also into AL-amyloidosis and light chain deposition disease (amorphous deposits of light chains damaging organs)…
For people with MGUS, there is an increased incidence of-
- osteoporosis and increased fracture risk
- kidney damage
- bacterial infections and
- thromboembolic complications
compared with the same age population without MGUS.
Clonal plasma cells, which are the basis of MGUS, may in some cases produce toxic monoclonal immunoglobulin which can damage the body’s own antibody activity by binding to specific antigens (such as cold agglutinin disease), or their deposits in organs (e.g. kidney damage) or physical properties (e.g. cryoglobulinemia).
Therefore, it is recommended that this group of people is regularly checked with the aim to capture not only transformation into symptomatic multiple myeloma or another malignant disease, but also the formation of the above-mentioned complications.
Moreover, it is recommended to monitor patients with asymptomatic myeloma and to initiate treatment only after symptoms of multiple myeloma are observed.
In 2014, discussion of subdivision of subgroups of patients with asymptomatic myeloma with high ( 80 %) probability of early (within 2 years) transformation in multiple myeloma which would be beneficial for early initiation of treatment is ongoing.
According to first proposals, patients with asymptomatic myeloma that meet at least one of the three conditions:
- more than 30 % of plasma cells in the bone marrow,
- ratio of free light kappa and lambda chains is greater than 100 or less than 0.01, or
- multiple focal lesions on whole-body MRI of the skelet…”
Cryoglobulinemia
“Cryoglobulinemia is a medical condition in which the blood contains large amounts of pathological cold sensitive antibodies called cryoglobulins – proteins (mostly immunoglobulins themselves) that become insoluble at reduced temperatures.[1] This should be contrasted with cold agglutinins, which cause agglutination of red blood cells.
Cryoglobulins typically precipitate (clumps together) at temperatures below normal body temperature – 37 degrees Celsius (99 degrees Fahrenheit) – and will dissolve again if the blood is heated. The precipitated clump can block blood vessels and cause toes and fingers to become gangrenous. While this disease is commonly referred to as cryoglobulinemia in the medical literature, it is better termed cryoglobulinemic disease for two reasons: 1) cryoglobulinemia is also used to indicate the circulation of (usually low levels of) cryoglobulins in the absence of any symptoms or disease and 2) healthy individuals can develop transient asymptomatic cryoglobulinemia following certain infections.[2]
In contrast to these benign instances of circulating cryoglobulins, cryoglobulinemic disease involves the signs and symptoms of precipitating cryoglobulins and is commonly associated with various pre-malignant, malignant, infectious, or autoimmune diseases that are the underlying cause for production of the cryoglobulins.[2][3]
Cutaneous manifestations of monoclonal gammopathy
“Monoclonal gammopathy associated with dermatological manifestations are a well-recognized complication. These skin disorders can be associated with infiltration and proliferation of a malignant plasma cells or by a deposition of the monoclonal immunoglobulin in a nonmalignant monoclonal gammopathy.
These disorders include POEMS syndrome, light chain amyloidosis, Schnitzler syndrome, scleromyxedema and TEMPI syndrome. This article provides a review of clinical manifestations, diagnostics criteria, natural evolution, pathogenesis, and treatment of these cutaneous manifestations..”