
Recently Diagnosed or Relapsed? Stop Looking For a Miracle Cure, and Use Evidence-Based Therapies To Enhance Your Treatment and Prolong Your Remission
Multiple Myeloma an incurable disease, but I have spent the last 25 years in remission using a blend of conventional oncology and evidence-based nutrition, supplementation, and lifestyle therapies from peer-reviewed studies that your oncologist probably hasn't told you about.
Click the orange button to the right to learn more about what you can start doing today.
- You are here:
- Home »
- Blog »
- Multiple Myeloma »
- Multiple Myeloma Diagnosis, Prognosis- READ THIS FIRST-
Multiple Myeloma Diagnosis, Prognosis- READ THIS FIRST-
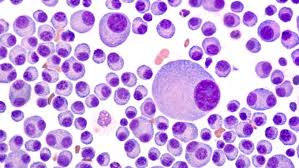
Explaining a multiple myeloma diagnosis as an “incurable cancer” is misleading. “Cancer isn’t a disease anymore, it is a collection of them.”
If you are struggling with a multiple myeloma diagnosis, prognosis, etc. please read this post and article below, before you do anything else. I am asking you to do this because the article linked and excerpted below outlines what I went through when I was first diagnosed with multiple myeloma. In short, I was diagnosed with incurable cancer with an average life expectance of 5-7 years and here I am writing this blog post more than 25 years later…
My experience as a myeloma survivor since 1994 combined with the article below can aid your struggle with your multiple myeloma diagnosis, prognosis.
- Multiple Myeloma is a combination of blood, urine, bone and genetic diagnostic information- your mm diagnosis, prognosis depends on dozens of variables-
- Conventional oncology does not explain MM or your options thoroughly. There is a lot that oncology doesn’t know about MM treatment and management-
- Regardless of your stage at diagnosis, your prognosis can vary by years-
I was originally diagnosed with a single bone plasmacytoma (SBP). I was told I had a form of ‘pre-myeloma,” really, a form of pre-cancer. Looking back at my symptoms, diagnostic testing, etc. knowing what I know now, I’m sure I had full-blown multiple myeloma.
My doctors got it wrong. I was mis-diagnosed. I should have immediately undergone anti-MM
- nutrition,
- supplementation,
- local radiation,
- bone therapies,
- mind-body therapies, etc.
to address my situation.
Oncology works hard to provide the right care for your incurable cancer but the fact remains that there is just too much that oncology doesn’t understand about your diagnosis.
I’m not trying to tell you that I am a “board certified oncologist.” I am telling you that my perspective and experience, while very different from an oncologist’s, offers a different perspective. I may be able to see therapies for you that your conventional oncologist would not consider.
Remember the main point of the article linked below: “cancer isn’t a disease anymore, it is a collection of them.” Consider a collection of therapies to manage your mm diagnosis, stage.
Are you struggling with a multiple myeloma diagnosis, prognosis? Scroll down the page, post a question or comment and I will reply to you ASAP.
Hang in there,
David Emerson
- MM Survivor
- MM Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Multiple Myeloma Nutrition, Supplementation- A How-To Guide
- Multiple Myeloma Diet- Before, During, After Therapy
- Living w/ Post-Cancer Fear As a Myeloma Survivor-
- Multiple Myeloma Diagnosis- Can’t Trust Conventional Cancer Research
When’s the Right Time to Mention the ‘C’ Word?
“I had been asked to see a young woman on the general medicine service. Earlier her mother had wheeled her into the emergency room where she then described a history of back pain lasting several weeks that had gotten steadily and significantly worse. She could not think of an inciting event—no trauma, no fall, no sports injury…
…A CT scan showed a lesion in her lumbar spine, which the radiology report commented was “consistent with metastatic disease.” She was admitted for further evaluation and management.
“Well, the workup sounds about right,” I said. “They really need a biopsy.”
“Does she know it might be cancer?” I added.
“Yes. Apparently she started crying when told that we were going to be seeing her,” the fellow said.
“What do you want to tell her now?” I asked, beginning to prep for our eventual conversation with the patient.
She paused for a moment. “I am not really sure where to go with this, especially without a diagnosis,” she said. “I’m curious to see what you’re going to say.”
En route, we stopped at radiology to personally review the films. We also pressed the radiologist as to what else this might be…
Even now, I think it is important to entertain a differential diagnosis. Many times in my career someone was told they had cancer, only to find out after a workup that this was not the case: It was Paget’s disease, not bone metastases; sarcoidosis rather than lung cancer…
“I’m Dr Dizon and I specialize in women’s cancers. Do you know why we are here?”
“Yes. It’s because I have terminal cancer—bone metastases. I’ve read about it on Google since they told me. It means I’m going to either become very sick due to chemo or I’m going to die. Or maybe both,” she said.
I could hear the anguish in her voice, see that “deer in headlights” look in her eyes. I sensed how her life had suddenly and dramatically changed with one word: cancer.
“Right now,” I continued, “all bets are off. It could be cancer, but it might not be. We need more information, so for right now, let’s do the workup that’s needed. We’ll follow you closely until we know more.”



