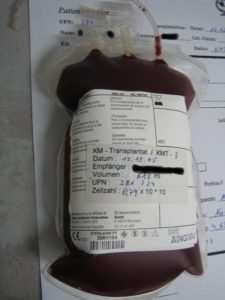
Recently Diagnosed or Relapsed? Stop Looking For a Miracle Cure, and Use Evidence-Based Therapies To Enhance Your Treatment and Prolong Your Remission
Multiple Myeloma an incurable disease, but I have spent the last 25 years in remission using a blend of conventional oncology and evidence-based nutrition, supplementation, and lifestyle therapies from peer-reviewed studies that your oncologist probably hasn't told you about.
Click the orange button to the right to learn more about what you can start doing today.
- You are here:
- Home »
- Blog »
- Multiple Myeloma »
- Multiple Myeloma Diagnosis- SPB, RVd Lite? MM Specialists?
Multiple Myeloma Diagnosis- SPB, RVd Lite? MM Specialists?
“Previous studies have shown that maximal-dose RVD leads to excellent overall response rates (ORR)… but has also been associated with toxicity and frequently requires dose reductions in older patients…”
Hi David- My husband had a plasma cytoma which has now metastasized into a multiple myeloma diagnosis and he has a fracture in his spine. He is in skilled nursing care right now undergoing local radiation for pain, then he will begin chemotherapy.
He is so wiped out already I am very worried about the chemo but has to have it for a shot at more life. Any suggestions? Thanks. Liz
Hi Liz-
A single plasma cytoma is considered pre-MM. I mention this because even if your husband’s pre-cancer grew into full multiple myeloma, I am thinking that he is early stage MM. He has just barely stepped into MM.
A diagnosis of early stage disease is fundamentally different from stage 2 or 3 MM. According to research, 95% of all MM is diagnosed at stage 2 or 3.
A general oncologist or hematologist-oncologist may not know this. Are you working with a MM specialist?
MM specialists, on average, achieve much better five-year survival averages, much longer survival statistics.
I agree with his undergoing local radiation in order to stabilize the lesion. Please ask his oncologist about kyphoplasty/vertibroplasty to further stabilize his spine after he has completed his radiation therapy.
Yes, your husband will continue with chemotherapy after his local radiation. However, please understand that the “standard-of-care” (SOC) induction chemotherapy regimen called Velcade-Revlimid-Dexamethasone (VRd, sometimes called RVd), will be much too much chemo for early stage MM.
And an autologous stem cell transplant is way too much toxicity.
In other words, the SOC is designed for the average MM patient. The average MM patient is relatively advanced MM (stage 2,3).
By undergoing VRd induction therapy your husband will be dealing with lots of toxicity and experiencing or at least risking many short, long-term and late stage side effects.
While stabilizing MM is certainly important for the newly diagnosed MM patient, it is important to understand that MM is incurable and all MM patients reach what is called “multi-drug resistance” (MDR).
By moderating your husband’s chemo at the beginning, you will increase his time to MDR.
At the very least consider an induction chemotherapy called RVd Lite. This is the same chemo cocktail yet at lower doses. Less chemo, less toxicity.
I have thrown a lot of info at you. I do not mean to overwhelm you. It’s just that few patients/caregivers reach out to me 1) that are stage 1 and 2) that have not yet begun SOC chemotherapy.
Lastly, I will link the nutrition and questions guides below.
Do you know your husband’s diagnostic info such as his 
- m-spike (monoclonal protein)
- immunoglobulins (IgG, IgA, IgM)
- freelight chains (Kappa, Lambda, K/L ratio)
- how old is your husband? What are your goals?
I can provide more info if I know more about your situation.
Let me know if you have any questions.
Hang in there,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Beating Myeloma: “If I Knew Then What I Know Now”
- Stage 1 Multiple Myeloma, Fendenzabole, Chemotherapy…
- Ask A Multiple Myeloma Survivor
RVD-Lite Has Comparable Efficacy, Improved Toxicity in Transplant-Ineligible MM
“Previous studies have shown that maximal-dose RVD leads to excellent overall response rates (ORR) and prolongs overall survival (OS) and progression-free survival (PFS) for transplant-ineligible patients with newly diagnosed MM (NDMM), but has also been associated with toxicity and frequently requires dose reductions in older patients…
The most frequently observed adverse effect was peripheral neuropathy, which occurred in 31 (62%) of 53 patients. Only 1 patient reported grade 3 symptoms.
The outcomes observed with RVD-lite was not significantly different from standard dose RVD, and had comparable efficacy, improved toxicity, and may be the new treatment standard for this patient population.”
Who are the GREAT EIGHT of Multiple Myeloma Specialists?
“Since this post was first published I have gotten a number of comments about specialists who were not selected. I also placed a lot of weight on those who had published or provided exceptional survival rates. I did this because I believe you can not manage that which you do not measure. However, many facilities that do not supply survival statistics use clinical trial results as a surrogate or substitute for actual survival data and treatment guidance. I also did not allow more than one from each facility. The most important takeaway for a myeloma patient is to have a myeloma specialist on your team, and you can find a listing of well over 200 if you CLICK HERE…
Choosing A Multiple Myeloma Specialist
“Looking back, I now realize that I developed a set of six questions that I eventually used to select my new multiple myeloma specialist.
- Is the doctor a Teller or an Asker?
- Is the doctor well established?
- Does the doctor have ties to the area?
- Is the doctor certified in hematology?
- Is the doctor covered by your insurance?
- How much are you willing to do to get the doctor you want?
Association Between Treatment Facility Volume and Mortality of Patients With Multiple Myeloma
“Purpose- To determine the association between the number of patients with multiple myeloma (MM) treated annually at a treatment facility (volume) and all-cause mortality (outcome)…
Results– There were 94,722 patients with MM treated at 1,333 facilities. The median age at diagnosis was 67 years, and 54.7% were men. The median annual facility volume was 6.1 patients per year (range, 0.2 to 109.9). The distribution of patients according to facility volume was: Q1: 5.2%, Q2: 12.6%, Q3: 21.9%, and Q4: 60.3%. The unadjusted median overall survival by facility volume was: Q1: 26.9 months, Q2: 29.1 months, Q3: 31.9 months, and Q4: 49.1 months (P < .001). Multivariable analysis showed that facility volume was independently associated with all-cause mortality. Compared with patients treated at Q4 facilities, patients treated at lower-quartile facilities had a higher risk of death (Q3 hazard ratio [HR], 1.12 [95% CI, 1.08 to 1.16]; Q2 HR, 1.17 [95% CI, 1.12 to 1.21]; Q1 HR, 1.22 [95% CI, 1.17 to 1.28]).
Conclusion– Patients who were treated for MM at higher-volume facilities had a lower risk of mortality compared with those who were treated at lower-volume facilities.”