Recently Diagnosed or Relapsed? Stop Looking For a Miracle Cure, and Use Evidence-Based Therapies To Enhance Your Treatment and Prolong Your Remission
Multiple Myeloma an incurable disease, but I have spent the last 25 years in remission using a blend of conventional oncology and evidence-based nutrition, supplementation, and lifestyle therapies from peer-reviewed studies that your oncologist probably hasn't told you about.
Click the orange button to the right to learn more about what you can start doing today.
- You are here:
- Home »
- Blog »
- Multiple Myeloma »
- Multiple Myeloma Prognosis- Upfront Radiation Therapy a Negative?
Multiple Myeloma Prognosis- Upfront Radiation Therapy a Negative?
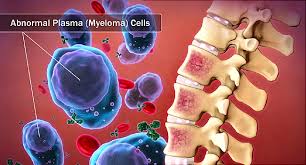
“We hypothesized that upfront Radiation Therapy (RT) is a marker of more aggressive disease associated with worse long‐term survival outcomes…”
As is often the case, I disagree with the finding of the study linked below. While the hypothesis is logical, I don’t think a newly diagnosed MMer who undergoes Radiation Therapy should worry that he/she automatically has a worse prognosis. Bone involvement, in my experience, does not indicate a worse multiple myeloma prognosis.
I say this mainly because of my own experience. Just like the study below indicates, I presented with bone damage to my spine. My fifth cervical vertebra had been eaten away by my MM. But this bone damage was not indicative of more aggressive disase. I was diagnosed in early 1994…
In my experience, radiation therapy is a marker of late diagnosis not necessarily of more aggressive disease. Picture an average 65 year old on the golf course. This guy, let’s call him Bob, has lived with pain in his spine, off and on, for years. Bob when to several different doctors trying to find a reason for his pain but no doctor ever was able to help Bob. After all, MM is difficult to diagnose when you don’t know what you’re looking for.
Then one day on the golf course, mid-swing, Bob cracks his spine, is rushed to the hospital and is told that he has MM growing in his spine. Bob undergoes RT to his spine. In this story, Bob’s MM is relatively slow growing and induction therapy and an ASCT puts Bob into MRD negative status and Bob enjoys a long progression-free survival aka remission for the next 7 years.
Bob also changes his diet, supplements with evidence-based non-toxic antioxidants such as curcumin, resveratrol and omega-3 fatty acids, and lives an anti-MM lifestyle of massage, whole body hyperthermia and frequent, moderate exerise.
Yes, bone damage is a serious complication for the newly diagnosed MMer. However MM therapy, both conventional and non-conventional can prove a long and growing list of therapies that have been shown to provide a longer overall survival and higher quality of life than ever before.
Have you been diagnosed with MM? Did you experience bone damage upon diagnosis and undergo RT? Are you worried that bone involvement leads to a worse multiple myeloma prognosis?
To learn more about evidence-based, non-toxic therapies to enhance your bone health or fight your MM, scroll down the page, post a question or comment and I will reply to you ASAP.
Thank you,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Multiple Myeloma-Adverse Events Since 1994-My Cancer Story
- C-B-D Strength/Dosing Info for Relapsed Myeloma
- Five Truisms of Incurable Disease from IBD to Myeloma
Prognostic significance of upfront radiation therapy in patients with multiple myeloma
“Skeletal complications of multiple myeloma (MM), including osteolytic lesions, fractures, and spinal cord compression, are a major source of morbidity and mortality for patients with this disease. Approximately 80% of MM patients present with radiographic evidence of skeletal lesions…
The degree of bone involvement in MM may correlate with specific cytogenetic lesions (trisomies or t[11;14]), a higher‐risk gene expression profile, and other markers of disease aggressiveness like β2‐microglobulin or serum lactate dehydrogenase.1..
We hypothesized that upfront RT is a marker of more aggressive disease associated with worse long‐term survival outcomes. Using a nationwide registry, our objectives were to examine patterns of use, associated factors, and survival among MM patients treated with upfront RT…
We defined “upfront RT” as RT delivered after myeloma diagnosis, within the timeframe from 90 days before up to 14 days after the start of first‐line chemotherapy…
Our observations in this large nationwide cohort indicate that nearly one in five of newly diagnosed MM patients in the United States received upfront RT, predominantly to the spine.
Receipt of upfront RT portends worse prognosis which persists even among long‐term survivors or patients undergoing transplantation, who often achieve excellent systemic control of their myeloma. We found that treatment in a community‐based rather than academic facility was the strongest factor associated with upfront RT in a multivariable model…
However, while worse OS among recipients of upfront RT might be due to more advanced disease or poorer tolerance of subsequent chemotherapy, persistence in sensitivity analyses raises a hypothesis that bone complications leading to urgent RT at diagnosis might reflect a more aggressive myeloma biology affecting long‐term outcomes…
In conclusion, our data provide a novel insight on the prognostic significance of upfront RT among MM patients, and underscore the need to address disparities that affect timely diagnosis, initial therapy, and subsequent outcomes in this population.”