
Recently Diagnosed or Relapsed? Stop Looking For a Miracle Cure, and Use Evidence-Based Therapies To Enhance Your Treatment and Prolong Your Remission
Multiple Myeloma an incurable disease, but I have spent the last 25 years in remission using a blend of conventional oncology and evidence-based nutrition, supplementation, and lifestyle therapies from peer-reviewed studies that your oncologist probably hasn't told you about.
Click the orange button to the right to learn more about what you can start doing today.
- You are here:
- Home »
- Blog »
- non-conventional therapies »
- Multiple Myeloma- Zinc
Multiple Myeloma- Zinc
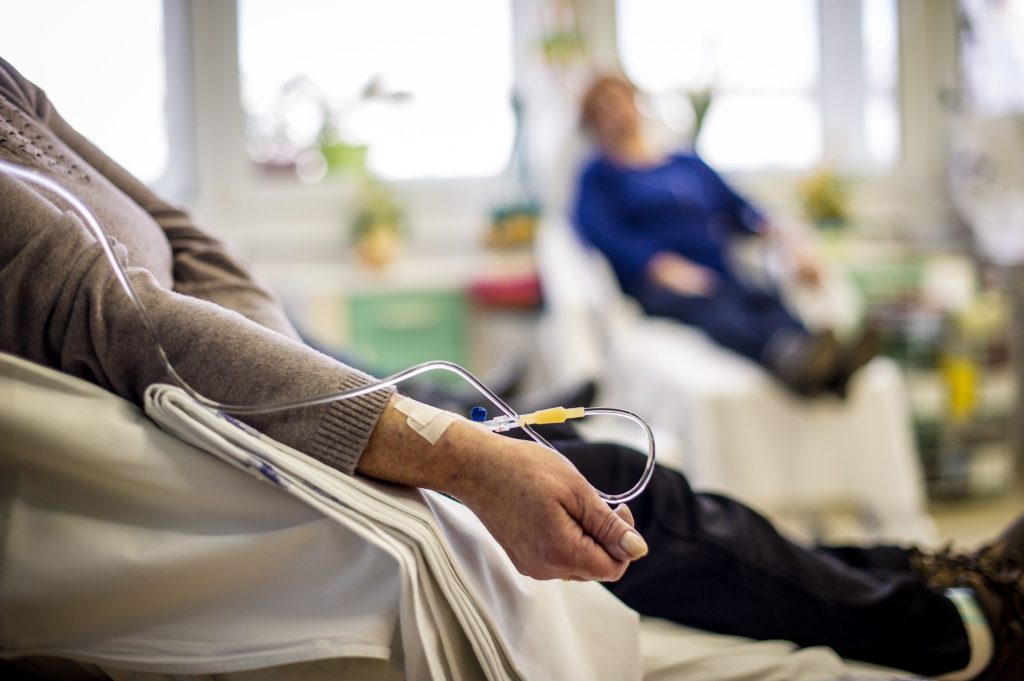
“Iovino, who’s also a blood stem cell transplant physician, had shown in a previous study that zinc could boost immune recovery in patients undergoing stem-cell transplants for the blood cancer multiple myeloma…”
Consider your immune health. Consider zinc as therapy after your autologous stem cell transplant for multiple myeloma.
A prognosis for multiple myeloma focuses on how long a newly diagnosed MM (NDMM) patient lives, on average, once he/she is diagnosed with this incurable blood cancer. NDMM patients’ understand that conventional MM oncology focuses on:
- Surgery
- Radiation and
- Chemotherapy
These conventional therapies are what the FDA focuses on. That’s what they do. Fine.
Inevitably, NDMM patients are at a loss for what to do before and after their surgery, radiation and chemo. Everyone agrees that chemo and radiation can hammer their immune system. Yet their oncologist doesn’t offer therapies to bring their immune system back to normal.
As a long-term mm survivor myself, I would argue that
- multiple myeloma diet and nutrition
- anti-mm supplements
- managing the patient’s autologous stem cell transplant experience
is/are every bit as important to the prognosis of the mm patient as killing the patient’s monoclonal proteins are.
According to the articles linked and excerpted below, zinc is needed to boost immune function (T-cells in particular) for the patient who has undergone chemo, radiation and especially aggressive chemo in the form of an autologous stem cell transplant.
According to the research linked below, zinc can be viewed as a myeloma therapy.
As a long-term mm survivor, I tend to focus on healthy, clean nutrition to bolster my immune system. I admit, however, that I do add nutritional supplements to my regimen when I think my diet isn’t enough.
Numerous studies confirm that curcumin, resveratrol, green tea extract, omega-3 fatty acids and more kill monoclonal proteins. Zine boosts the bodies production of t-cells.
To learn more about both conventional and evidence-based non-conventional therapies for the newly diagnosed mm patient, click the blue bar at the top of the page. Learn about the MM cancer coaching program. I think you’ll be glad that you did.
Let me know if you have any questions.
Hang in there,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Surviving Multiple Myeloma- Post-Cancer Fear
- A Long-term Multiple Myeloma Survivor’s Diet, Nutrition Plan-
- Multiple Myeloma Survivor- Chemotherapy, Heart Failure-
- Multiple Myeloma Chemotherapy = Accelerated Aging
Burst of accumulated zinc shows how the mineral boosts immune function, suggesting ways to improve health
In mice, zinc helps thymus of the immune system regrow and immune-cell recovery after bone marrow transplant
“Using mice, the team discovered that zinc is needed for the development of disease-fighting immune cells called T cells and prompts regeneration of the thymus, the immune organ that produces T cells…
Thymic regeneration and immune function, and zinc…
Since the scientists knew that low levels of zinc are linked to fewer infection fighting T cells and a shrunken thymus, where T cells develop…
Iovino, who’s also a blood stem cell transplant physician, had shown in a previous study that zinc could boost immune recovery in patients undergoing stem-cell transplants for the blood cancer multiple myeloma…
Zinc is critical for T-cell development and thymic regeneration…
He also found that zinc deficiency slows recovery of T-cell numbers after mice receive immune-destroying treatments akin to those given to patients about to receive a blood stem cell transplant.
Conversely, extra zinc speeds this process, and T cells recover faster than normal…
“What we think is going on is, as you give zinc supplementation, that gets accumulated within the developing T cells. It gets stored and stored and stored, then the damage comes along and the zinc is released…”
Zinc and Cancer
Zinc is an essential mineral important for growth and development, immune function, protein synthesis, DNA synthesis, cell division, and wound healing.1
Supplementation with zinc has been studied primarily as a component of a multivitamin for chemoprevention against several different cancer types. Zinc supplementation alone has also been evaluated as a preventative for radiotherapy-induced side effects among patients with head and neck cancer (HNC). This fact sheet is a review of study data about the relationship between zinc supplementation and cancer incidence and outcomes.
Cancer Prevention
SU.VI.MAX Study
The double-blind Supplementation in Vitamins and Mineral Antioxidants (SU.VI.MAX) study evaluated the effect of a multivitamin on health outcomes, including the risk of developing skin cancer or prostate cancer.2
The study randomly assigned 13,017 participants aged 35 to 60 to an antioxidant supplement comprised of zinc (20 mg), selenium, β-carotene, and vitamins C and E, or placebo once daily for a median follow-up of 7.5 years.
The study demonstrated a significant decrease in total cancer incidence and total mortality among men, but not women, with antioxidant supplementation compared with placebo.3 This benefit was, however, no longer evident 5 years after supplement discontinuation.
In the SU.VI.MAX study, the incidence of any type of skin cancer was significantly higher with antioxidant supplementation compared with placebo among women (1.3% vs 0.7%; P = .02), which was driven by a higher number of melanomas (0.3% vs 0.08%; P = .01), whereas the number of nonmelanoma skin cancers was similar between groups (0.8% vs 0.5%; P = .15).2
Among men, there was no significant difference in incidence of any type of skin cancer between the antioxidant and placebo arms.
The SU.VI.MAX study demonstrated a nonsignificant decrease in prostate cancer incidence among men who received the antioxidant supplement compared with placebo (hazard ratio [HR], 0.88; 95% CI, 0.60-1.29), which was particularly evident among men with a normal prostate-specific antigen (PSA) at baseline (HR, 0.52; 95% CI, 0.29-0.92).4 The benefit was not observed among men with an elevated PSA at baseline (HR, 1.54; 95% CI, 0.87-2.72). This finding is in contrast with a systematic review and meta-analysis that included 3 different studies, which demonstrated no associated with prostate cancer and zinc supplementation (odds ratio [OR], 1.18; 95% CI, 0.71-1.96).5



