Leave a Comment:
2 comments
[…] Myeloma Chemotherapy Blood Side Effects […]
Reply[…] Myeloma Chemotherapy Blood Side Effects […]
Reply
Multiple Myeloma an incurable disease, but I have spent the last 25 years in remission using a blend of conventional oncology and evidence-based nutrition, supplementation, and lifestyle therapies from peer-reviewed studies that your oncologist probably hasn't told you about.
Click the orange button to the right to learn more about what you can start doing today.
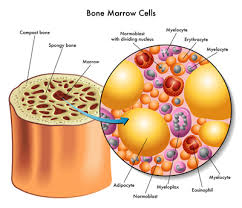
The good news is that conventional oncology has gotten pretty good at putting myeloma patients into remission. The bad news is achieving remission usually involves a lot of myeloma chemotherapy. Doublets, triplets, ASCT (single or double), and maintenance therapies mean toxicity bringing short, long-term and late stage collateral damage.
Unfortunately chemotherapy damages your bone marrow and therefore your blood. The more chemo you undergo, the more toxicity your body has to process. Most of the time MM patients heal the damage done by chemotherapy.
Depending on your age and how much toxicity you’ve had to process, your bone marrow may be permanently damaged.
The life of a MM patient and survivor is to balance the damage done by your cancer, multiple myeloma, with the damage done by your “life-saving” therapies. Too much or one or the other and the MM survivor can be in real trouble…
The challenge of myeloma patients and survivors is to identify and manage their side effects…again and again if necessary.
In general, the term myelosuppression means that chemotherapy can damage a person’s red blood cells, white blood cells and platelets. If the damage is severe enough a myeloma patient may have to alter his/her therapy plan and can even die. As I say, it is in the MMer’s interest to manage this probable side effect.
While the article linked and excerpted below lists conventional therapies to heal your blood levels of red and white cells and platelets if chemotherapy causes myelosuppression of any kind, I want to link several evidence-based non-conventional therapies for you to consider.
Folic Acid & Chemotherapy- “Many people receiving chemotherapy for cancer experience drops in their folic acid levels and blood counts due to the effect of certain drugs.”
Vitamin B12 & Chemotherapy “There are many side effects of chemotherapy, depending on the combination and types of drugs being used..”
Starting Chemotherapy: 15 Nutrition Tips ““Chemotherapy and radiation treatments place their own burdens on the nutrition system in addition to the cancer itself,”
Please watch the video below to learn more about the evidence-based, integrative therapies to combat treatment side effects and enhance your chemotherapy.
My experience and research as a long-term MM survivor is evidence-based but non-conventional therapies such as anti-angiogenic, anti-inflammatory nutrition and supplementation. Curcumin, Black Seed oil and other non-conventional therapies have been shown to not only fight MM but heal much of the damage done by multiple myeloma itself- heal bone damage, heal kidney damage, heal heart damage, and more.
Are you undergoing chemotherapy? Do you have
I am both a MM survivor and MM Cancer Coach. Please scroll down the page, post a question or comment and I will reply to you ASAP.
Thank you,
David Emerson
“Background: Oncologic emergencies associated with multiple myeloma include myelosuppression (anemia, neutropenia, and thrombocytopenia), bone-related emergencies, and acute renal failure…
Myelosuppression -The hematologic toxicities of anemia, neutropenia, and thrombocytopenia are a direct result of the various degrees of myelosuppression caused by treatment with immunomodulatory agents, proteosome inhibitors, or monoclonal antibodies. Myelosuppression is defined by the National Cancer Institute ([NCI], 2017) as a condition in which bone marrow activity is decreased, resulting in fewer red blood cells, white blood cells, and platelets. The range of these myelosuppressive hematologic toxicities can vary from minor inconveniences to life-threatening complications.
Anemia -Anemia is defined by the NCI (2017) as a condition in which the number of red blood cells is below normal. This results in a reduction in hemoglobin, which decreases the oxygen-carrying capacity of the blood (Miller, 2010).
Neutropenia -Neutropenia is defined by the NCI (2017) as a condition in which there is a lower-than-normal number of neutrophils (a type of white blood cell). All grades of neutropenia severity can lead to OEs, such as neutropenic fever, pneumonia, and sepsis in patients who already harbor functional immunoglobulin deficiency (Miceli et al., 2008). In patients with MM, neutropenia may be caused by the disease or by its treatment.
Thrombocytopenia –Thrombocytopenia is defined by the NCI (2017) as a condition in which there is a lower-than-normal number of platelets in the blood and is the primary cause of bleeding in patients with all types of cancer.

“Chimeric antigen receptor (CAR) T-cell targeted multiple myeloma antigens such as CD138, kappa-light chain, and B-cell maturation antigen (BCMA) as well as CD19 had been widely adopted. More and more CAR-T clinical trials for MM presented encouraging results [1,2,3].
However, current CAR-T treatment still faces the adverse reactions as cytokine release syndrome (CRS), myelosuppression, and other complications, especially, severe myelosuppression is often a fatal threat to patients.
We adopted the stem cell infusion to promote hematopoietic recovery for a relapsed MM patient developing severe and persistent myelosuppression after CAR-T cell therapy…”
[…] Myeloma Chemotherapy Blood Side Effects […]
Reply[…] Myeloma Chemotherapy Blood Side Effects […]
Reply