- You are here:
- Home »
- Blog »
- pre-cancer »
- Nocturnal Gastroesophageal Reflux (GERD) Therapies
Nocturnal Gastroesophageal Reflux (GERD) Therapies
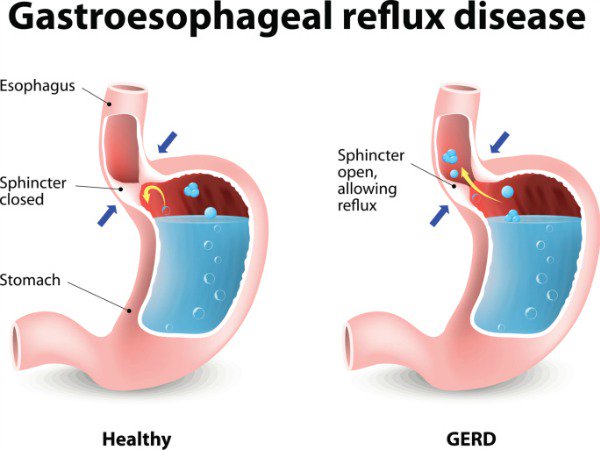
“Sleep disturbances are frequently encountered in up to 25% of the GERD patients, likely due to nocturnal gastroesophageal reflux (GER).”
Gastrointestinal reflux disease is not cancer. However, GERD increases your risk of barrett’s esophagus (BE) which increases your risk of esophageal cancer.
GERD and BE really affect your quality of life. My point in all this is that it is in your best interest to heal/prevent GERD. Especially when the therapies are cheap and easy.
I am a survivor of a cancer called multiple myeloma. I have been researching and writing about GERD because radiation to my neck in 1996 weakened my swallowing muscles allowing stomach acid to leak into my throat occasionally. I don’t want to develop GERD, or BE and I certainly don’t want anything to do with esophageal cancer.
In addition to foods shown to heal GERD, consider supplementing with curcumin. Curcumin supplementation has been shown to protect against barrett’s esophagus, others.
It has happened only a couple of times in the past year but I recently experienced nocturnal gastrointestinal reflux disease and thought I should study this challenge and see if I could fix it.
It turns out, according to the article linked and excerpted below, that I can influence night time GERD. Not only to, as the article discusses, sleep in my left side when possible. But I also make sure my head is tilted upward as much as is comfortable. Gravity…
- To Learn More About Non-Toxic Therapies for Pre-Cancer- click now
- To Learn More About GERD- click now
Do you have GERD? Ever experience symptoms at night? Scroll down the page, post a question or comment and I will reply to you ASAP.
Thanks,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- I have Barrett’s Esophagus- what are my options?
- Barrett’s Esophagus- Diagnosis, Prognosis and Treatment
- Ask the Cancer Coach-“Stage 4 esophageal cancer diagnosis and treatment”
What to know about the advanced stages of GERD
“Gastroesophageal reflux disease, commonly called GERD, is a chronic condition that happens when the acids in the stomach back up into the esophagus. There are several stages of GERD, ranging from mild to severe.
This article discusses the advanced stages of GERD, how it progresses, the diagnosis process, and more.
Nocturnal Gastroesophageal Reflux Disease (GERD) and Sleep
An Important Relationship That Is Commonly Overlooked
“Gastroesophageal reflux disease (GERD) is a prevalent, chronic medical condition that affects 13% of the adult population globally at least once a week. Sleep disturbances are frequently encountered in up to 25% of the GERD patients, likely due to nocturnal gastroesophageal reflux (GER).
With advance in diagnostic techniques allowing for an improved understanding of involved physiological mechanisms of nocturnal reflux, there is growing evidence of a bidirectional relationship between GERD and sleep disturbances.
Furthermore, nocturnal GER is associated with more complicated GERD. Obstructive sleep apnea (OSA) and GERD also have been linked, but to what degree remains controversial. Treatment of nocturnal GER has been shown to improve both subjective and objective sleep measures.
The therapeutic approach includes lifestyle modifications and medication individualization and optimization with proton-pump inhibitors serving as the mainstay of treatment. Antireflux surgery and newer endoscopic procedures have been demonstrated to control nocturnal GER…”
Left lateral sleep position may alleviate nocturnal esophageal acid exposure, symptoms
“Among patients who experience nocturnal gastroesophageal reflux, the left lateral decubitus sleep position correlated with significantly shorter esophageal acid exposure time and faster esophageal acid clearance, according to research.
“Up to 80% of the patients with gastroesophageal reflux disease experience burdensome symptoms at night, which can have a negative effect on sleep quality,” Jeroen M. Schuitenmaker, MD, of the department of gastroenterology and hepatology at Amsterdam University Medical Centers, and colleagues wrote in the American Journal of Gastroenterology. “The aim of this study was to investigate the effect of spontaneous sleep positions on the occurrence of nocturnal gastroesophageal reflux by combining pH-impedance and sleep position monitoring in a large prospective cohort of patients with reflux symptoms.”
Schuitenmaker and colleagues included 57 patients who were referred for ambulatory pH-impedance reflux monitoring with supine esophageal acid exposure of 0.5% or higher. They used a sleep position measurement device to measure concurrent sleep positions (left, right, supine and prone) and evaluated composition, type and proximal extent of reflux episode and sleep position for each nocturnal gastroesophageal reflux episode.
Researchers observed a shorter acid exposure time in the left lateral position (median 0%) vs. right lateral (median 1.2%, P = .022) and supine positions (median 0.6%, P = .022). They also observed a shorter esophageal acid clearance time in the left lateral decubitus position (median 35 seconds) compared with supine (median 76 seconds, P = .030) and right lateral positions (median 90 seconds, P = .002).
“These findings provide a rationale for interventions aiming to promote the left lateral decubitus sleep position to alleviate nocturnal esophageal acid exposure and reflux symptoms,” Schuitenmaker and colleagues wrote.”
Can a Wearable for Sleep Positioning Help With Nocturnal Reflux?
“Patients with gastroesophageal reflux disease (GERD) who experience nighttime heartburn had symptom alleviation with a wearable electronic sleep positioning device, a Dutch randomized trial found.
In the sham-controlled trial of 100 such patients using the wearable nightly for 2 weeks, 44% of those assigned to the active arm — where the devices vibrated throughout the night if they rolled onto their right side, a position associated with higher esophageal acid exposure — had a reduction in GERD symptoms, reported Jeroen Schuitenmaker, MD, of the University Medical Centers Amsterdam, and colleagues.
The reduction was significantly higher compared to those whose sham devices were only set to vibrate during the first 20 minutes (24%; P=0.03).
At 2 weeks, those using the active device had more reflux-free nights (9 vs 6 nights in the sham group; P=0.01), according to the findings in Clinical Gastroenterology and Hepatology.
“Nocturnal gastroesophageal reflux symptoms, such as heartburn and regurgitation, have a negative impact on sleep quality,” Schuitenmaker told MedPage Today. “Current treatment strategies, including acid suppressive medication, often do not provide sufficient relief.”
In the study, patients in the active arm were significantly less likely to end up sleeping in the right lateral decubitus position than those in the sham group (2% vs 24%), and they spent more of their time in the left lateral decubitus position (61% vs 39%), which is associated with less esophageal acid exposure and quicker acid clearance time (P<0.001 for both)…
The primary outcome was defined as a 50% or greater reduction in the Nocturnal Gastroesophageal Reflux Disease Symptom Severity and Impact Questionnaire (N-GSSIQ) score.
For inclusion, patients had to have nocturnal heartburn and/or acid reflux symptoms occurring at least three times per week and a total reflux symptom score of ≥8. Those with obstructive sleep apnea and prior gastric/esophageal surgery were excluded, among others…
Average participant age was 52, nearly two-thirds were women, and about half consumed alcohol. About half (47%) were on proton pump inhibitors (PPIs), and 60% were on antacids. One-third only had nighttime symptoms while the remaining had both daytime and nighttime symptoms.
After 2 weeks of treatment, average total N-GSSIQ scores were lower in the active device group (18.8 vs 23.7 in the sham group, P=0.04).
A post-hoc analysis showed that even those on PPIs who did not have a diaphragmatic hernia achieved success with the device…”


