
Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Primary Cervical Cancer-Secondary Cancer
Primary Cervical Cancer-Secondary Cancer
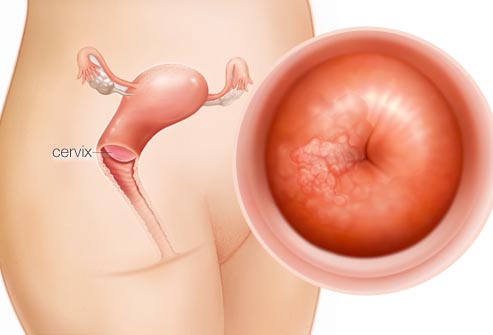
“…a small subset of women who developed Primary Cervical Cancers (PCC) will develop second malignancies after their initial diagnosis. Little is known about these women.”
The study linked and excerpted below astounds me. Primary Cervical Cancer does not astound me. What is surprising is that women who develop PCC are at higher risk of a secondary cancer once they undergo either/or/both chemotherapy or radiation.
The only new information contained in the study below is that those PCC patients who have HPV can develop another HPV related cancer.
The reason for my blogging about treatment-related secondary cancers is not simply to agonize over this fact. I am a cancer survivor who has lived without treatment-related secondary cancer occurrence since my aggressive chemo and radiation from ’94-’97.
- I have eliminated my HPV.
- I avoid my increased risk of skin cancer
- I remain in complete remission from my original cancer multiple myeloma
- I have avoided all other cancer diagnoses.
Because it is impossible to prove a negative, I guess I simply could be lucky in avoiding all treatment-related secondary cancers. But I don’t think so…
I live an evidence-based but non-conventional, non-toxic anti-cancer lifestyle through
- Nutrition
- Supplementation
- Lifestyle therapies (exercise, sauna, etc.)
Examples of what I mean by “living an anti-cancer lifestyle” would be daily moderate exercise, regular saunas, acupuncture, eating lots of fruits and veggies, limited red meat, minimal alcohol, curcumin/vitamin D/omega-3.
Have you been diagnosed with primary cervical cancer? Would you like to reduce your risk of a secondary cancer? Scroll down the page, post a question or a comment and I will reply to you ASAP.
- Click now to learn more about cervical cancer.
- To Learn More about Treatment-related Secondary Cancers- click now
Thank you,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- HPV Variable Risk Factor in Cervical Cancer
- Anti-angiogenesis Extends Cervical Cancer Survival
- Treat HPV Naturally Before Cancer Strikes
Second Malignancies Following Primary Cervical Cancer Diagnosis: Analysis of the SEER Database
“Introduction- While mortality following primary cervical cancers (PCCs) continues to decline due to advancements in screening and treatment, a small subset of women who developed PCCs will develop second malignancies after their initial diagnosis. Little is known about these women.
Objective-This study aims to determine the common second malignancies among patients with primary cervical cancers and the factors associated with improved overall survival.
Methodology– We conducted a retrospective analysis of all PCCs in the SEER database between 1975 and 2016. We identified a subset of patients who subsequently developed secondary malignancies after a primary cervical cancer diagnosis. We then determined the factors associated with a prolonged latency interval, defined as the time between the PCC diagnosis and a subsequent secondary malignancy diagnosis. In a sub-analysis, we also determined the commonest secondary malignancies following a PCC diagnosis.
Results- A total of 1,494 patients with cervical cancers developed a second malignancy during the study period. The mean age at diagnosis of the PCCs was 56.0 ± 14.0 years. The mean latency interval between PCC and a subsequent secondary malignancy was 9.6 ± 9.3 years.
- Cytoreductive surgery
- and radiotherapy
during the PCC are associated with a prolonged latency interval.
Patients who received chemotherapy were more likely to develop second malignancies within 10 years after a PCC diagnosis.
The most common second malignancies were-
- abdominal malignancies with rectal cancers (12.2%),
- pancreatic cancers (10.1%),
- stomach cancers (9.2%),
- cecum cancers (8.4%), and
- sigmoid colon cancers (8.3%).
Conclusion-There is a significant association between Hispanic ethnicity and a shorter latency interval among patients with PCC. The findings from this study may help optimize screening for secondary cancers among cervical cancer survivors…
After their initial diagnosis of primary cervical cancer (PCC), survivors may be at increased risk for subsequent secondary malignancies with poorer outcomes [5]. Earlier studies have reported a correlation between secondary malignancies with radiotherapy for PCCs [5-8]. The associated risk factors such as HPV infection and cigarette smoking in cervical cancer survivors can also predispose this population to a greater risk for secondary malignancies [5,6,9]…
Similar to cervical cancers, other HPV infection-related cancers of the pharynx, anorectum, and other genital sites are also risk factors for a secondary malignancy [6,9]…
Other risk factors for the development of secondary malignancies include
- women’s age at the time of the diagnosis of PCC,
- administration of radiotherapy versus chemotherapy,
- surgical intervention,
- HPV infection,
- and cigarette smoking.
These factors may determine the latency interval, defined as the time in years from a primary malignancy diagnosis to the diagnosis of a subsequent second malignancy. The temporal risk of secondary cancer in cervical cancer survivors has been reported to persist after 40 years [5]…
Study population- We studied patients with a diagnosis of primary cervical cancer (PCC) who developed second malignancies between January 2007 and December 2016…
Conclusions- In conclusion, understanding the clinicopathological features of second cancers after a prior cervical cancer diagnosis is important given the increasing number of survivors. There is a significant disparity in the occurrence of a second malignancy among women with a primary cervical cancer diagnosis.
This is unusual considering the fact that these women had undergone some form of treatment and active surveillance following a prior cancer diagnosis…”


