
Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- non-conventional therapies »
- Recurrent, HPV, Head, Neck Cancer- Therapies
Recurrent, HPV, Head, Neck Cancer- Therapies
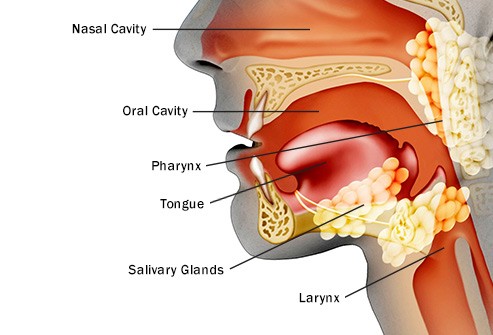
“However, all current treatment regimens for head and neck cancer have adverse effects. Therefore, continuing investigations have been undertaken to seek less toxic therapies to reduce treatment morbidity for head and neck cancer.”
My fiance is about to start Keytruda therapy for recurring head and neck squamous hpv cancer. 3 lymph nodes involved. We would like more info on grapeseed extract and alternative therapies. Sherry-
Hi Sherry-
- If your fiancé undergoes Keytruda, he should consider adding fiber to his diet as fiber is shown to enhance the efficacy of immunotherapy.
- As you read in the blog post that you came in on, grapeseed extract has been shown to kill head and neck cancer. I would also consider curcumin supplementation also.
- I would also consider a nutrient-dense diet.
- I was also HPV positive when I was diagnosed with my cancer (myeloma is different, I know, I’m just saying…) and I supplemented with AHCC for two months- shown to clear the virus.
- Click now to learn more about hyperbaric oxygen therapy-
- To Learn More about HPV and Cancer, click now
- To Learn more about H&N radiation side effects- click now
- To Learn More about the cancer killing ability of Grape Seed Extract- click now
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
Immunotherapy for head and neck cancer: Recent advances and future directions
Concentration effects of grape seed extracts in anti-oral cancer cells involving differential apoptosis, oxidative stress, and DNA damage-
Grape seeds extract (GSE) is a famous health food supplement for its antioxidant property. Different concentrations of GSE may have different impacts on cellular oxidative/reduction homeostasis. Antiproliferative effect of GSE has been reported in many cancers but rarely in oral cancer.
Methods- The aim of this study is to examine the antioral cancer effects of different concentrations of GSE in terms of cell viability, apoptosis, reactive oxygen species (ROS), mitochondrial function, and DNA damage.
Results-High concentrations (50–400 μg/ml) of GSE dose-responsively inhibited proliferation of oral cancer Ca9-22 cells but low concentrations (1–10 μg/ml) of GSE showed a mild effect in a MTS assay. For apoptosis analyses, subG1 population and annexin V intensity in high concentrations of GSE-treated Ca9-22 cells was increased but less so at low concentrations. ROS generation and mitochondrial depolarization increased dose-responsively at high concentrations but showed minor changes at low concentrations of GSE in Ca9-22 cells. Additionally, high concentrations of GSE dose-responsively induced more γH2AX-based DNA damage than low concentrations.
Conclusions-Differential concentrations of GSE may have a differentially antiproliferative function against oral cancer cells via differential apoptosis, oxidative stress and DNA damage.
Anti-cancer effects of curcumin on head and neck cancers-
“Head and neck cancer is the sixth large type of cancer in the world. The treatment regimens for head and neck cancer encompass surgery, radiotherapy and chemotherapy. However, all current treatment regimens for head and neck cancer have adverse effects. Therefore, continuing investigations have been undertaken to seek less toxic therapies to reduce treatment morbidity for head and neck cancer.
Substantial evidence has demonstrated that curcumin inhibited proliferation, migration, invasion and metastasis and induced apoptosis via modulating multiple signaling pathways in head and neck cancer. Curcumin also suppressed the growth of xenograft derived from head and neck cancer in vivo in animal models.
This review summarizes the evidence demonstrating potential use of curcumin as a single chemotherapeutic agent or in combination with other chemotherapeutic agents and radiation to minimize their toxicity in head and neck cancer. Although curcumin has been shown to be safe at doses of 8 g/d in both phase I and phase II clinical trials, its bioavailability is poor. Overcoming the poor bioavailability of curcumin in the near future would facilitate its clinical use.
Effects of Immunonutrition in Head and Neck Cancer Patients Undergoing Cancer Treatment – A Systematic Review-
In conclusion, the present review found that supplementation with immunonutrient-enriched formulas in HNC patients during radiotherapy and chemotherapy may improve or maintain nutrition status. Supplementation with glutamine during HNC radiotherapy and chemotherapy may delay the onset of oral mucositis and reduce the incidence of severe oral mucositis. However, these findings are not conclusive, given the studies heterogeneity. Therefore, further investigations are encouraged in the future, focusing on the timing, dosage and duration of immunonutrition required for nutrition optimisation.

