
Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- non-conventional therapies »
- The Melanoma Paradox-
The Melanoma Paradox-
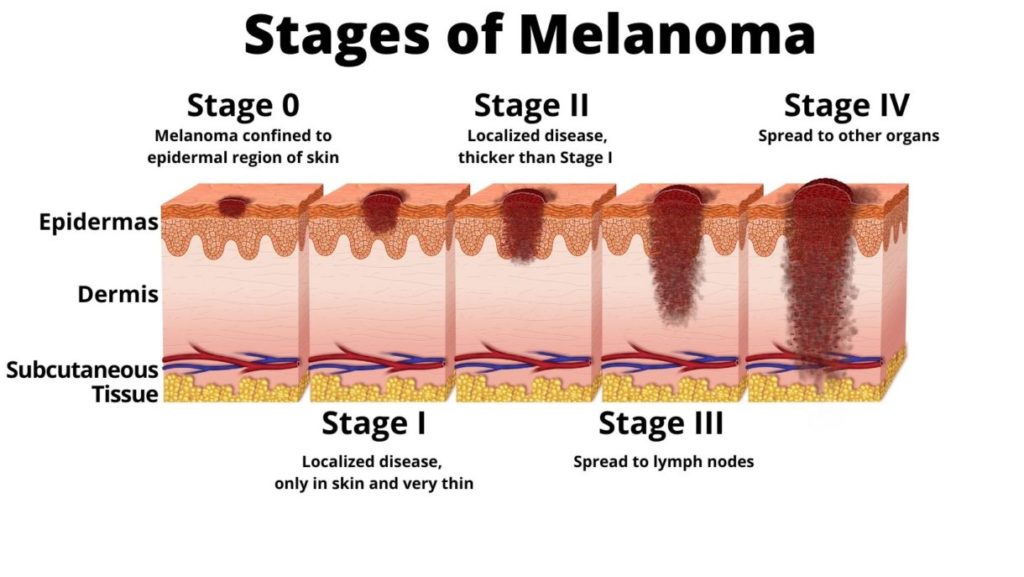
While the number of skin cancer cases—specifically for melanoma—is anticipated to increase by 14 percent this year, the number of deaths from melanoma is decreasing by 4 percent.1
There is no paradox here. Analysis without bias is what is required. Sherlock Holmes (Sir Arthur Conan Doyle) said “Once you eliminate the impossible, whatever remains, no matter how improbable, must be the truth.” Applying this philosophy to the melanoma paradox,
- Melanoma (Mel.)diagnoses will increase by 14% in 2017
- Melanoma deaths will decrease by 4% in 2017
- Melanoma is incurable with an average five-year survival rate of less than 10%– current standard-of-care therapies don’t help much-
Based on the assumptions above I believe that melanoma is over diagnosed and under-treated.
This over diagnosis may be a matter of “better safe than sorry” for the patient. While over diagnosis will cost insurers and patients more money, over diagnoses may save lives in the long run.
The real issue is possible over-treatment. Undergoing chemo for a diagnosis of melanoma can be rough on the patient. Especially if the patient doesn’t have cancer.
My idea and experience of under-treatment is exhibited by nutrition, supplementation and lifestyle therapies. Therapies that are rarely discussed by oncology.
It is important to understand that there are evidence-based, non-toxic therapies that studies have shown will reduce the risk of melanoma becoming metastatic.
I am a cancer survivor of a different but incurable cancer. I have learned that cancer patients must look beyond conventional oncology when it comes to managing their own incurable cancers.
Have you been diagnosed with melanoma? What stage? Please scroll down the page, post a question or comment and I will reply to you ASAP.
Thank you,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Non-Melanoma Skin Cancer Risk Increases From Radiation
- Preventing Non-Melanoma Skin Cancer Relapse
- How to Identify Skin Cancer in 5 Steps
- Skin Cancer, Vitamin D3 and Sunlight
THE SKIN CANCER PARADOX
“Recent statistics from the American Cancer Society revealed a paradox about skin cancer: While the number of skin cancer cases—specifically for melanoma—is anticipated to increase by 14 percent this year, the number of deaths is decreasing by 4 percent.1,2 How can it be that while new cases are on the rise, so is the number of survivors?
We asked skin cancer experts Ivor Caro, M.D. and Josina Reddy, M.D., Ph.D., to help make sense of this puzzling statistic and point to ways that may help reduce skin cancer rates…
In instances where surgery alone can’t treat skin cancer, medicines targeting specific gene mutations that cause skin cancers are now available to patients, as well as treatments that stimulate the immune system to recognize skin cancers and mount an attack on them.9 These types of therapies used to treat advanced forms of skin cancer may slow the growth of the cancer or make it shrink...1,6″
Melanoma risk perception and prevention behavior among African-Americans: the minority melanoma paradox
“Introduction-
Mel. is the most deadly type of skin cancer with 75% of all skin cancer deaths within the US attributed to it. Risk factors for mel. include ultraviolet exposure, genetic predisposition, and phenotypic characteristics (eg, fair skin and blond hair). Whites have a 27-fold higher incidence of melanoma than African-Americans (AA), but the 5-year survival is 17.8% lower for AA than Whites. It is reported continuously that AA have more advanced melanomas at diagnosis, and overall lower survival rates. This minority melanoma paradox is not well understood or studied.
Objective
To explore further, the possible explanations for the difference in mel. severity and survival in AA within the US.
Methods
Qualitative review of the literature.
Results
Lack of minority-targeted public education campaigns, low self-risk perception, low self-skin examinations, intrinsic virulence, vitamin D differences, and physician mistrust may play a role in the melanoma survival disparity among AA.
Conclusion
Increases in public awareness of mel. risk among AA through physician and media-guided education, higher index of suspicion among individuals and physicians, and policy changes can help to improve early detection and close the melanoma disparity gap in the future.


