Leave a Comment:
2 comments
[…] Will Ductal Carcinoma In-Situ (DCIS) Patients Accept Some Risk? […]
Reply[…] Will Ductal Carcinoma In-Situ (DCIS) Patients Accept Breast Cancer Risk? […]
Reply
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
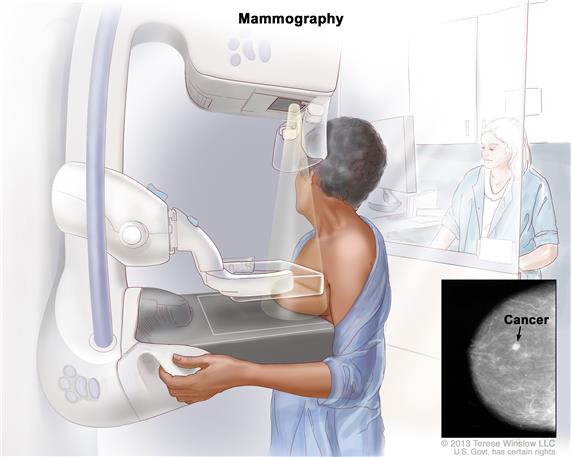
One of the first thoughts of someone diagnosed with DCIS is about her increased risk of breast cancer (BC). This thought is followed by the risk of adverse events aka side effects from therapies to reduce the risk of breast cancer. Tamoxifen, local radiation, and lumpectomy can all cause short, long-term and late stage side effects.
Oncologists spend most of their time talking about reducing the risk of BC. The study discussed below is about DCIS patients thinking more about side effects and less about their risk of breast cancer.
I am a long-term cancer survivor of a blood cancer called multiple myeloma. I live with several serious treatment-related adverse events. At this point in my life, it is much more likely that I die of a treatment-related side effect than my “incurable cancer.”
One of my problems with conventional oncology is that they can prescribe only FDA approved therapies. Therapies that can cause short, long-term and late stage side effects.
But what if a therapy could reduce a person’s risk of breast cancer but not cause side effects?
I understand how and why the FDA works. And I understand the importance of FDA approved therapies. At the same time, as a cancer survivor with an “incurable cancer” I understand the value of evidence-based non-conventional therapies.
When I use the phrase evidence-based non-conventional therapies, I’m talking about nutrition, supplementation and lifestyle therapies shown by studies to reduce the risk of breast cancer. And most of us, cancer survivors or not, understand the health benefits of nutrition, supplementation and life style to our health. The key is to provide a list of those therapies as well as the studies that support them as BC therapies.
I am not saying for a moment that conventional oncology isn’t first and foremost in the lives of cancer patients. What I am saying is that evidence-based, non-conventional therapies can reduce your risk of breast cancer.
To learn more about DCIS and the evidence-based therapies that can help you prevent its spread into invasive breast cancer, please watch the video below:
To download the DCIS Guide, click here.
Have you been diagnosed with DCIS? Are you a risk dominator or a nonrisk dominator? Why or why not? Readers of this blog post will learn from your answer.
Scroll down the page, post a question or a comment.
Thank you,
David Emerson
“While some patients are unwilling to accept any degree of breast cancer risk as a trade-off for less invasive treatment of ductal carcinoma in situ, the majority of participants in one recent experiment were willing to shoulder some degree of risk if it meant mitigating some treatment-related side issues.
There has been a lot of discussion about potentially de-escalating therapy for DCIS, but little is known about patient preference and how many women would choose surveillance if it were offered. To investigate what attributes of treatment women consider most important and evaluate the degree of risk they might accept, researchers at one institution surveyed healthy women from their screening mammography clinic. The survey was designed as a discreet choice experiment, a type of instrument used in marketing research that allows researchers to weigh the intensity of a preference.
Of the 194 women who completed the survey, 57 were considered risk dominators, meaning they were unwilling to choose any trade-offs that might raise their risk. But 137 were nonrisk dominators, meaning they were willing to accept some level of exchange between risk and other attributes of treatment…
“We were also able to calculate the surgical trade-offs that nonrisk dominators were willing to make, and the 10-year absolute breast cancer risk at which they were willing to make them…”
Of note, the nonrisk dominators were more likely to be women who had witnessed a loved one endure breast cancer treatment or death. “Our thought is that seeing loved ones go through the severe side effects associated with breast cancer made them think about how they would incorporate that into their own life,” Ms. Chapman said.
The findings suggest that the majority of women are willing to accept some breast cancer risk to lessen the attributes associated with treatment, including a change in breast appearance after surgery, but also that there is significant variability in how women view treatment attributes and to what degree that influences their final decision.“As such,” Ms. Chapman said, “our research highlights the importance of patient-centered decision making and the necessity of discussing treatment trade-offs with our patients rather than solely focusing on breast cancer risk.”
[…] Will Ductal Carcinoma In-Situ (DCIS) Patients Accept Some Risk? […]
Reply[…] Will Ductal Carcinoma In-Situ (DCIS) Patients Accept Breast Cancer Risk? […]
Reply