- You are here:
- Home »
- Blog »
- Non-Melanoma Skin Cancer »
- Clearing Actinic Keratosis-Photodynamic + Topical Therapies
Clearing Actinic Keratosis-Photodynamic + Topical Therapies

When compared with monotherapy, photodynamic therapy in combination with a topical treatment had significantly higher complete clearance rates and partial clearance rates (of actinic keratosis).
It makes sense. Combining two conventional topical therapies to clear actinic keratosis is more effective than one. As long as there are no additional side effects to manage, and as long as your health insurance or medicare covers the therapies then the patient benefits. It also makes sense is to undergo evidence-based non-toxic therapies shown to reduce the risk of skin cancer.
The facts are overwhelming. According to SkinCancer.org, actinic keratosis affects more than 53 million Americans. I’m not one of those yet but because:
- I live with in increased risk of non-melanoma skin cancer (NMSC) and
- I’ve already had one small basel cell cancer removed and
- I sat in the sun way too much as a teen/young person and
- because I am bald…
I am sure I will develop actinic keratosis some day. I’m not saying all the above to brag, I’m saying all the above to state the size of the problem and then offer possible solutions- both conventional (FDA approved) and evidence-based non-conventional therapies.
Actinic keratosis, by itself, may be unsightly but is not life threatening. But, according to skincancer.org, it does increase your risk of NMSC by up to 20%. NMSC is not life threatening either. But both basel cell and squamous cell carcinomas (NMSC) increase your risk of melanoma. And melanoma is definately life threatening!
If you have been diagnosed with either actinic keratosis and/or NMSC, in addition to conventional therapies such as photodynamic therapy (AK) or Mohs surgery (NMSC) please consider non-toxic therapies such as green tea extract, vitamin e oil, coffee, curcumin, omega-3 fatty acids and others.
To Learn More About Actinic Keratosis- click now
To learn more about non-toxic AK and NMSC therapies scroll down the page, post a question or comment and I will reply to you ASAP.
Thank you,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Chemo Cream Prevents Non-Melanoma Skin Cancer?
- Preventing Non-Melanoma Skin Cancer Relapse
- The “BEST” Treatments for Basel Cell Carcinoma?
- Melanoma and Basel Cell Non-Toxic, Heart-healthy Therapy
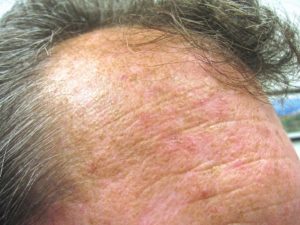
Actinic keratosis
“Actinic keratosis (AK) is a pre-cancerous[2] area of thick, scaly, or crusty skin.[3][4] These growths are more common in fair-skinned people and those who are frequently in the sun.[5] They are believed to form when skin gets damaged by ultraviolet (UV) radiation from the sun or indoor tanning beds, usually over the course of decades. Given their pre-cancerous nature, if left untreated they may turn into a type of skin cancer called squamous cell carcinoma.[4] Untreated lesions have up to a 20% risk of progression to squamous cell carcinoma,[6] so treatment by a dermatologist is recommended…”
Combination of Photodynamic, Topical Therapy Improves Outcomes in Actinic Keratosis
“The combination of photodynamic therapy and another topical treatment may be superior to monotherapy for treatment of actinic keratoses, according to a meta-analysis published in the Journal of The European Academy of Dermatology and Venereology…
Researchers completed a systematic literature review of Medline, Embase, and CENTRAL databases to assess the efficacy and tolerability of adding photodynamic therapy to topical interventions in patients with actinic keratoses. Randomized control trials with patients who were clinically or histopathologically diagnosed with actinic keratoses, used an intervention of field-direct photodynamic therapy treatment or daylight photodynamic therapy or a combination of both, and contained a comparison group were included in this meta-analysis.
Outcomes were:
- clearance rates,
- pain from treatment, and
- local skin reactions.
When compared with monotherapy, photodynamic therapy in combination with a topical treatment had significantly higher complete clearance rates and partial clearance rates. Reports of pain from treatment were mixed, with one study reporting no patients experiencing pain from treatment and one study reporting that combination therapy was more painful than monotherapy. Local skin reactions were reported in only one study with very low quality of evidence…
Limitations of this study include a high clinical heterogeneity of interventions, short-term efficacy follow-ups, the outcome quality of evidence was rated as low or very low, and there was a high estimated risk for bias.
The researchers concluded, “the combination of [photodynamic therapy] with another topical modality may offer efficacy benefits compared to one field-directed treatment alone.”