
Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Cryoablation Outperforms Radical Prostatectomy
Cryoablation Outperforms Radical Prostatectomy

“for PCa (cryoablation) using individualized cryoneedle delivery based on biopsy-proven cancer mapping achieved acceptable oncologic and functional outcomes with low rates of incontinence and complications.”
You’ve been diagnosed with prostate cancer (PCa). Based on your discussions with your oncologist/urologist, the PCa is advanced enough that you want to undergo more than active surveillence and more the other early stage therapies.
Your goal is to undergo a therapy that will both eradicate your PCa, while minimizing your risk of short, long-term and late stage side effects that can be associated with radical prostatectomy such as incontinence and impotence. According to the article linked below, cryoablation might just be that therapy.
The most important sentence in the study below is “achieve acceptable oncologic and functional outcomes with low rates of incontinence and complications.” In laymen’s terms, this means you want the best chance of killing your PCa with the lowest risk of complications such as incontinence and impotence.
As always, studies like the one below must be broken down aka translated. In order for the study to mean something to you, you want to see if your situation applies to the study-
 The median follow-up was 5 years. Patients had a
The median follow-up was 5 years. Patients had a- median age of 71 years and
- median PSA level of 7.5 ng/mL.
- The clinical stage was
- T1c in 48% of men,
- T2 in 44%,
- and T3 in 8%)
In terms of getting rid of your PCa forever, according to the article below, ” PSA level above 0.2 ng/mL, was 39% for the cryoablation cohort and 79% for the RP cohort- meaning the risk of rising PSA levels after cryotherapy was 40% less than prostatectomy. A big difference. The risk of
The main finding of the study focused on patients’ PSA after five years. 39% of the cryotherapy patients experienced post-treatment PSA levels above 0.2 ng/mL and 79% of the radical prostatectomy patient had post-treatment PSA levels above 0.2 ng/mL. Cryo PCa patients had less than half the risk of PSA rising after the procedure.
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
PCa Cryoablation Achieves Acceptable Outcomes
“Primary whole gland cryoablation for prostate cancer (PCa) based on targeted biopsy-proven cancer mapping, achieves acceptable oncologic and functional outcomes at 5 years, investigators reported at the Society of Urologic Oncology 17th annual meeting in San Antonio, Texas.
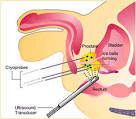
Alfredo Maria Bove, MD, and colleagues at the University of Southern California in Los Angeles reviewed the records of 102 patients undergoing whole gland cryoablation for localized PCa. At entry, image-based cancer mapping using staging biopsy guided by transrectal ultrasound and Doppler were digitally documented. All procedures were performed under TRUS guidance with individualized cryoneedle delivery based on preoperative cancer mapping. The researchers defined biochemical failure as post-treatment PSA level above 0.2 ng/mL and a PSA nadir + 2 (the Phoenix definition).
The median follow-up was 5 years. Patients had a median age of 71 years and median PSA level of 7.5 ng/mL. The clinical stage was T1c in 48% of men, T2 in 44%, and T3 in 8%). The D’Amico group risk was low in 24% of men, intermediate in 50%, and high in 26%. In 65 patients (66%) PSA declined to below 0.2 ng/mL. The estimated biochemical failure-free survival (EBFFS) rate was 84% by the Phoenix definition. In addition, 73 biopsies were performed in 43 (44%) patients, with 5 (5%) positive for PCa.
Complications developed in 13 patients (12.7%). The incontinence rate was 4%. Potency recovered in 12% of patients.
The researchers compared the cryoablation cohort with 102 men who underwent open radical prostatectomy (RP), matching the patients by preoperative PSA level, Gleason score, and clinical stage. The 5-year EBFFS, based on patients who had a post-treatment PSA level above 0.2 ng/mL, was 39% for the cryoablation cohort and 79% for the RP cohort, a statistically significant difference between the groups. Metastases developed in 5 (5%) of the cryoablation patients and 4 (4%) of the RP patients. Eight cryotherapy and 12 RP patients required salvage treatment.
Dr Bove and colleagues concluded that cryoablation “for PCa using individualized cryoneedle delivery based on biopsy-proven cancer mapping achieved acceptable oncologic and functional outcomes with low rates of incontinence and complications. Regarding metastases and need for salvage treatment, cryoablation provided median 5-year oncologic outcomes comparable to that of pair-matched open RP.”
Cancer prehabilitation is emerging as a method of better preparing patients for the often toxic and disabling effects of cancer treatment. Its place within the continuum of cancer care is rapidly being established.
If you were about to go on a ski trip but you hadn’t been on the slopes for a few years you might head to the gym to get your legs in shape. I have lots of friends who try to lose a few pounds before summer in an effort to look better when they put on a swimsuit. Both of these examples are prehabilitation.
Granted, a cancer diagnosis is much more serious than a ski trip or the beach but the idea is the same.
Cancer Prehabilitation is one or more therapies that each of us understands intuitively. Performing a certain exercise to prepare for surgery, chemotherapy and/or radiation to improve the healing or the recovery time just makes sense. Learning about your cancer diagnosis in order to prepare emotionally and reduce anxiety and stress also makes sense.
For information about you or a loved one can pre-habilitate for his/her induction initial cancer therapy whether it’s surgery, chemotherapy or radiation, scroll down the page, post a question or comment and I will reply ASAP.
thank you,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Nutrition- Before, During and After Cancer Therapy-
- Immunotherapy, Antibiotics and Cancer
- Supplements and Cancer Care- A How-To Guide
Prehab Offers Faster Track to Recovery From Ca Treatment
“Early data suggest that this “bundled” approach is effective. In a study published last October, colorectal cancer patients who took part in a prehab program that included regular aerobic exercise and strength training, a personalized nutrition program and protein supplementation, and guided relaxation, performed better on the six-minute walk test both before and after surgery than patients who received only standard postsurgical rehabilitation (Anesthesiology 2014;121[5]:937-947, PMID: 25076007)
Cancer Prehabilitation Improves Outcomes
“Prehabilitation is one or more interventions performed in a newly diagnosed cancer patient that are designed to improve physical and mental health outcomes as the patient undergoes treatment and beyond. Cancer prehabilitation uses a multidisciplinary approach combining exercise, nutritional, and psychological strategies to prepare patients for the challenges of cancer treatment, such as surgery, chemotherapy, immunotherapy, and radiation therapy…
In addition to improved physical and psychological health outcomes for oncology patients, cancer prehabilitation can reduce morbidity, increase treatment options, prevent hospital readmissions, and lower both direct and indirect healthcare costs attributed to cancer treatment...
Family conflicts, other non-physical worries before cancer surgery raise patients’ complication risk
“Meeting non-medical needs and improving quality of life ahead of operations can aid recovery and cut health care costs, a new study suggests. Quality of life as measured in the study is about more than happiness and how well people feel physically, a researcher says. It also includes the financial, spiritual, emotional, mental and social aspects of their lives and whether their needs are being met.”
10 Ways to Prepare for Surgery
- Be your best.
- Familiarize yourself with the surgery.
- Speak up.
- Learn about anesthesia.
- Ask about your diet.
- Know what to expect after surgery.
- Practice relaxation techniques.
- Plan for medications.
- Prepare your home.
- Pack a bag.
Effects of a combination of whey protein intake and rehabilitation on muscle strength and daily movements in patients with hip fracture in the early postoperative period
“Elderly patients can be at risk of protein catabolism and malnutrition in the early postoperative period. Whey protein includes most essential amino acids and stimulates the synthesis of muscle protein. The purpose of this study was to investigate the effect of resistance training in combination with whey protein intake in the early postoperative period…”
Understanding Prehabilitation, with Arash Asher, MD, and An Ngo-Huang, DO
“After cancer treatment, our rehabilitation program can help a person regain strength, physical functioning, and independence. However, there has recently been a new interest in prehabilitation, which is a personalized program of nutrition, exercise, and emotional support to help a person diagnosed with cancer prepare for treatment, such as surgery or radiation therapy…”


