
Recently Diagnosed or Relapsed? Stop Looking For a Miracle Cure, and Use Evidence-Based Therapies To Enhance Your Treatment and Prolong Your Remission
Multiple Myeloma an incurable disease, but I have spent the last 25 years in remission using a blend of conventional oncology and evidence-based nutrition, supplementation, and lifestyle therapies from peer-reviewed studies that your oncologist probably hasn't told you about.
Click the orange button to the right to learn more about what you can start doing today.
- You are here:
- Home »
- Blog »
- Multiple Myeloma »
- Young Myeloma- Longer OS, Shorter LifeSpan-
Young Myeloma- Longer OS, Shorter LifeSpan-
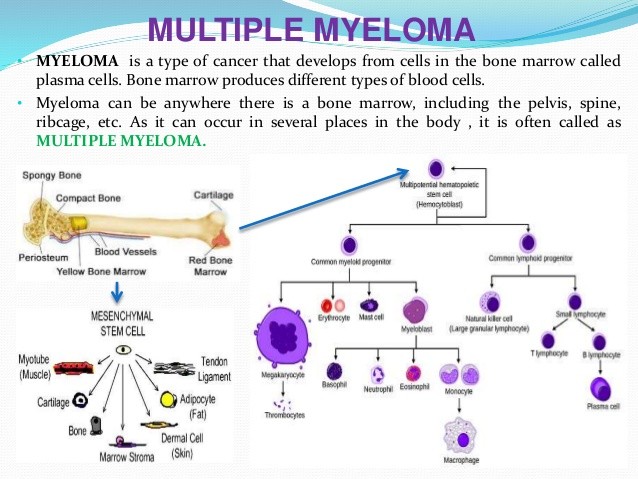
“Ninety percent of patients received intensive chemotherapy followed by autologous stem cell transplant, and 25% of patients had allogeneic stem cell transplant predominantly at time of relapse.”
The young multiple myeloma patient faces different challenges than the typical MM patient.
The first two studies linked and excerpted below are the strongest possible arguments I have every come across for the control side of the debate in Dr. Vincent Rajkumar’s Cure vs. Control Debate in Multiple Myeloma (the third link below).
In his essay linked and excerpted below, Dr. Rajkumar, a world renowned MM Specialist at the Mayo Clinic in Rochester, MN, asks the question if newly diagnosed myeloma patients should be treated with
“multidrug, multitransplant combinations with the goal of potentially curing a subset of patients, recognizing that the risk of adverse events and effect on quality of life will be substantial?”
For the record, MM is an incurable blood cancer. I think the “curing” that Dr. Rajkumar is referencing is what conventional oncology is calling a “functional cure.” Not the actual cure that normal people think of.
The demographic of newly diagnosed myeloma (NDMM) patients in the study below are an extreme example of what Dr. Rajkumar is questioning.
Should young NDMM patients, young people with their entire adult lives ahead of them, be given aggressive, high dose therapies knowing that, according to the research, they will live- at best- about 15 years. And according to the study linked and excerpted below that, those 15 years will be damaged with short, long-term and late stage side effects such as:
- endocrinopathies,
- musculoskeletal disorders,
- cardiopulmonary compromise and
- subsequent malignancies.
The solution, in my experience, is the control side of what Dr. Rajkumar posits. That is to say,
“Or should we address myeloma as a chronic incurable condition with the goal of disease control, using the least toxic regimens, emphasizing a balance between efficacy and quality of life, and reserving more aggressive therapy for later?”
I work with MM patients who stumbled on to this control approach because of negative reactions to their induction therapy. In essence, these NDMM patients demanded a low-dose of chemo (often the low-dose of revlimid/lenalidomide, the standard-of-care for elderly, transplant Ineligible patients) for as short a duration as possible. Only enough chemo to reduce their diagnostic metrics, stop chemo until their numbers increase again necessitating a little more chemo.
And these MM patients are not even the young, early stage (ISS-1) NDMM patients who have every reason to expect DECADES of life ahead of them. Decades without the fear of serious long-term and late stage side effects.
Let it be clearly understood that all conventional oncologists should understand what I understand. I am not a board certified oncologist. Far from it. I am a long-term MM survivor. A survivor living with all of the long-term side effects discussed below that result from aggressive, high-dose chemotherapy. I had an ASCT in 1995.
My point is, this is not theoretical for me. The studies below simply establish what I know to be true from my own life since my MM diagnosis in 1994.
If you are a newly diagnosed MM patients- at whatever age, or stage of MM, and you would like to learn more about the control side of Dr. Rajkumar’s Cure vs. Control Debate, scroll down the page, post a question or comment and I will reply to you ASAP.
Thanks for your time and attention,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- PeopleBeatingCancer- Side Effects Program
- Myeloma Therapy- Deeper Response or longer PFS, OS, Fewer Side Effects?
Epidemiological landscape of young patients with multiple myeloma diagnosed before 40 years of age: the French experience
“Multiple myeloma (MM) is rare in young patients, especially before age 40 years at diagnosis, representing <2% of all patients with MM…
In this study, we examined 214 patients diagnosed with MM at age ≤40 years over 15 years, in the era of modern treatments.
Among them, 189 patients had symptomatic MM. Disease characteristics were similar to older patients:
- 35% had anemia,
- 17% had renal impairment, and
- 13% had hypercalcemia.
The staging was
- ISS-1 in 52.4%,
- ISS-2 in 27.5%, and
- ISS-3 in 20.1%.
Overall, 18% of patients had high-risk cytogenetics [del 17p and/or t(4;14)]. Ninety percent of patients received intensive chemotherapy followed by autologous stem cell transplant, and 25% of patients had allogeneic stem cell transplant predominantly at time of relapse.
The median follow-up was 76 months, the estimated median overall survival was 14.5 years, and the median progression free-survival was 41 months. In multivariate analysis, bone lesions, high ISS score, and high-risk cytogenetics were significant risk factors for poor outcomes.
Among predefined time-dependent covariables, onset of progression significantly shortened overall survival. At 5 years, relative survival compared with same age- and sex-matched individuals was 83.5%, and estimated standardized mortality ratio was 69.9, confirming that MM dramatically shortens the survival of young patients despite an extended survival after diagnosis…
Long-term health impacts of hematopoietic stem cell transplantation inform recommendations for follow-up
“However, hematopoietic stem cell transplantation (HSCT) survivors are at risk of developing long-term complications, such as
- endocrinopathies,
- musculoskeletal disorders,
- cardiopulmonary compromise and
- subsequent malignancies.
These complications have a direct impact on the morbidity and mortality experienced by HSCT survivors.
Two-thirds of HSCT survivors develop at least one chronic health condition; while a fifth develop severe or life-threatening conditions.
HSCT patients who have survived for at least 5 years post-transplantation are at a fourfold to ninefold increased risk of late mortality for as long as 30 years from HSCT, producing an estimated 30% lower life expectancy compared with the general population…
Treatment of Myeloma: Cure vs Control
“Although not often openly acknowledged, “cure vs control” is the dominant philosophical difference behind many of the strategies, trials, and debates related to the management of myeloma. Should we treat patients with myeloma with multidrug, multitransplant combinations with the goal of potentially curing a subset of patients, recognizing that the risk of adverse events and effect on quality of life will be substantial?
Or should we address myeloma as a chronic incurable condition with the goal of disease control, using the least toxic regimens, emphasizing a balance between efficacy and quality of life, and reserving more aggressive therapy for later?
To be sure, if cure were known to be possible (with a reasonable probability) in myeloma, it would undoubtedly be the preferred therapeutic goal of most patients and physicians. But this is not the case. Myeloma is generally not considered a curable disease; however, new definitions of cure have been suggested, including operational cure, which is defined as a sustained complete response (CR) for a prolonged period.1,2 Cure vs control is debated because the strategies currently being tested are not truly curative but rather are intended to maximize response rates in the hope that they will translate into an operational cure for a subset of patients…”


