Recently Diagnosed or Relapsed? Stop Looking For a Miracle Cure, and Use Evidence-Based Therapies To Enhance Your Treatment and Prolong Your Remission
Multiple Myeloma an incurable disease, but I have spent the last 25 years in remission using a blend of conventional oncology and evidence-based nutrition, supplementation, and lifestyle therapies from peer-reviewed studies that your oncologist probably hasn't told you about.
Click the orange button to the right to learn more about what you can start doing today.
- You are here:
- Home »
- Blog »
- Multiple Myeloma »
- Myeloma Relapse – Extramedullary Tumors-
Myeloma Relapse – Extramedullary Tumors-
Daratumumab is a first-in-class myeloma therapy, human immunoglobulin G1 kappa (IgG1κ) monoclonal antibody that binds malignant cells expressing CD38 with high affinity and induces tumor cell death
Hi David- My mom is 68 and was diagnosed with multiple myeloma 2 years ago. Mom’s induction therapy at was RVd (revlimid, velcade and dexamethasone). Mom achieved a relatively short remission and the RVd eventually stopped working. Mom was just told that her multiple myeloma relapsed.
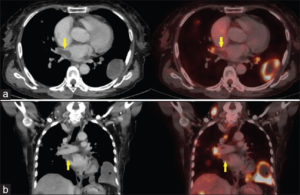
Currently extramedullary tumors are growing in mom’s abdominal cavity. Her oncologist is unable to radiate these tumors because of where they are and the tissue/placement of them. Mom has now completed one cycle with pomalyst instead of revlimid.
The tumors still grew so they want to stop the Pomalyst and switch to possibly Darzelex. Not sure if the name but it was FDA approved Monday. Any suggestions? Recommendations? We are desperate
Hi Caregiver- I am sorry to read of your mom’s Multiple Myeloma relapse. I think the MM therapy that you are considering is called darzelex aka daratumumab.
Pease confirm this with your mom’s oncologist but I believe that your mom should undergo both SOC chemo (darzelex) and would have had local radiation if she could. Also consider non-conventional therapies such as nutrition, exercise, whole body hyperthermia, etc.
Please watch the video below to learn more about the evidence-based, integrative therapies to combat treatment side effects and enhance your chemotherapy.
Thanks,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
How I treat extramedullary myeloma.
“Extramedullary myeloma (EMM) is defined by the presence of plasma cells (PCs) outside the bone marrow in a patient with multiple myeloma (MM).
Using sensitive imaging techniques including magnetic resonance imaging and positron emission tomography/computed tomography, EMM may be found in up to 30% of MM patients across the overall disease course.
The molecular mechanisms underlying the hematogenous spread of PCs outside the bone marrow are only partially known and involve hypoxia and an altered expression of adhesion molecules.
Extramedullary disease is associated with adverse prognostic factors (ie, high lactate dehydrogenase level, 17p deletion, and high-risk gene expression profile). The prognosis of EMM is poor, and the median overall survival of patients who experience an extramedullary relapse is <6 months.
The adverse prognosis is less pronounced in patients with bone-related plasmacytomas than in those with hematogenous EMM. EMM patients should be considered as having high-risk myeloma and treated accordingly. However, EMM clinical situations are extraordinarily heterogeneous, and their management is particularly challenging. In the present review, a case-and-comment format is used to describe our approach to the management of EMM.”