Post-traumatic growth, like post-traumatic stress, is not universal. Research shows that some people are more likely than others to have this experience.
According to the article below “The positive life changes that develop as a result of a stressful, frightening experience are called “post-traumatic growth.” Because I’ve written recently about PTSD and my cancer, multiple myeloma, I zoomed in on this article linked below wondering if there is a sort of flip side to my PTSD.
I’m self-diagnosing of course, but I believe I exhibit symptoms of both PTSD as well as symptoms of PTG. I am hyper vigilant and I am confident that positive life changes have come out of my myeloma survival.
I wonder if there is less post-traumatic growth among survivors of cancers with dismal five-year average survival rates. Pancreatic and lung cancer, for example, are considered incurable. As is my cancer, multiple myeloma.
My thinking is that because MMers are often consumed with their diagnosis, treatment, relapse, etc. during the years following their diagnosis, I think MMers have no time to breath much less have time to gain a greater appreciation for life and grow spiritually.
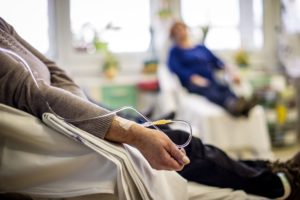
And let’s face it. Chemotherapy and radiation can make your life miserable. Myeloma patients are continually in and out of chemotherapy. Often aggressive chemotherapy.
I wonder if MMers develop a sense of fatalism, they may not allow themselves to grow? Don’t misunderstand me. I’m not saying that MMers don’t have the capacity to grow, spiritually, because of their cancer. I’m saying that that they don’t allow themselves and don’t have a chance to grow.
I think I’m trying to say that confronting our own mortality and reaching complete remission can impart positive life experiences. I appreciate the little things more. I smile more.
However, I think post-traumatic growth may be difficult for the cancer patient who relapses continually like many myeloma patients do.
Are you a multiple myeloma survivor? What do you think- PTSD or PTG?
Scroll down the page, post a question or comment and I will reply to you ASAP.
Thanks,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading-
“The concept that suffering can be a source of positive personal change has deep roots in many ancient thoughts and traditions. But scientific research trying to explain it is quite new. Studies show that after a traumatic event, reports of personal growth are more common than those of psychiatric disorders.
Some people may find, after enough time has passed, that living through or with cancer has helped them to make some positive changes in their lives. The positive life changes that develop as a result of a stressful, frightening experience are called “post-traumatic growth.” Researchers note that post-traumatic growth is not the same as resilience. Resilience describes people “bouncing back” or returning to their previous levels of functioning. On the other hand, post-traumatic growth refers to positive personal change of some kind.
Types of personal growth
People may experience different types of change while coping with cancer, including:
- Improved relations with others. Living with cancer may increase feelings of closeness or intimacy with family or friends. It may make it easier to connect with others who have had a traumatic event.
- New life experiences. Having cancer may change your priorities, causing you to make different life choices. You may be motivated to make a career change, overcome a fear, or fulfill a life goal.
- A greater appreciation for life. A cancer survivor may have an increased regard for life’s value or a new sense of vulnerability to death. This awareness may help you appreciate the world in new ways.
- A sense of personal strength. Living with cancer can help you develop increased mental strength and a sense of empowerment. You can be proud of what you have accomplished.
- Spiritual development. Some people living with cancer find they gain an increased interest in practicing religion or adding spiritual depth to their daily lives.
Having post-traumatic growth does not mean that you have completely overcome the stress and other feelings about having cancer. Growth and suffering can happen at the same time. In fact, most people who report post-traumatic growth also report having struggles. A person may grow in one area of their life and not another, or in a number of areas at different times.
Post-traumatic growth, like post-traumatic stress, is not universal. Research shows that some people are more likely than others to have this experience. Those who are generally open to new experiences and who sustain a mostly cheerful outlook may be more likely to benefit. It may also help to be able to handle trauma, have a strong support network, and be adaptable to life’s challenges.
“Cancer survivors often report posttraumatic growth (PTG). The aims of this study were to assess the presence of PTG in Italian long-term disease-free cancer survivors (LCS) and to explore the association between the dimensions of PTG and clinical, demographic variables, various agents of perceived social support and psychological distress…
Results– Mean age was 57.08 years, mean survival was 11.04 years (range 5–32), and the most common cancer diagnosis was breast cancer (56.9%). The PTGI average total score was higher in more educated LCS, in those employed, in LCS with longer time from diagnosis, and in those with no comorbidities. In this study, PTG was not found correlated with distress, but it correlated with perceived social support, age, education, and employment.
Conclusions- The absence of a correlation between PTG and psychological distress and the low levels of PTG found let us question the importance of talking about PTG when working as psychotherapists with LCS. It may be suggested that the need of finding benefit and PTG in LCS has been overcome by other experiences or worries happened after the cancer, and LCS may not focus anymore on positive changes occurred. The relevance of work and of perceived social support as linked to PTG stresses the need to protect the LCS’s relationship with work and to promote and sustain their social network, and this can help them to experience sharing and closeness to others...”




