Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- non-conventional therapies »
- SPB – Prognosis, Treatment
SPB – Prognosis, Treatment
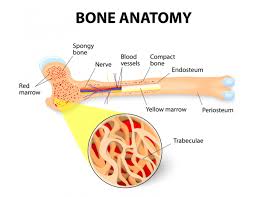
“According to the guidelines for the treatment of SPB, radiation remains the mainstay of the treatment.1, 18, 19 And radiotherapy provides long‐term local control in patients with SPB.18“
Single Plasmatytoma of Bone. Solitary Plasmacytoma of Bone and even Single Bone Plasmacytoma- SPB or SBP. I’ve seen this diagnostic term all three ways. I’ve been paying attention to this stage of pre-mm because this is how my multiple myeloma journey began in January of 1994.
I won’t bore you with the details of how I began life as a MM patient. But I will encapsulate the long study linked below into the key elements for you to understand if you or a loved one has been diagnosed with a SPB or SBP.
- This diagnosis is not cancer. It is pre-multiple myeloma. This diagnosis increases your risk of a full MM diagnosis.
- The most effective therapy for a SPB, SBP is local surgery to remove the monoclonal protein cells and then radiate the area.
- The majority of SPB, SBP patients eventually develop frank multiple myeloma.
- Solitary plasmacytoma is relatively rare, accounting for only 3% of all plasma cell neoplasms.
- If the single lesion is INSIDE the bone it is a SPB- if it is OUTSIDE the bone, it is referred to as an extramedullary plasmacytoma (SEP).1
Like the two other diagnoses of pre-myeloma- monoclonal gammopathy of undetermined significance (MGUS) and smoldering multiple myeloma (SMM) this issue is the risk of full-blown multiple myeloma- an incurable blood cancer.
As an aside, my oncologist wasn’t sure if I had a lesion in my skull back in early 1994. According to the study below, SPB’s in the skull are a positive prognostic indicator. Interesting…
According to research, local resection and local radiation is standard therapy. My experience is to assume a diagnosis of multiple myeloma someday and pursue all forms of evidence-based but non-toxic therapies including:
- antiangiogenic nutrition,
- anti-MM nutritional supplementation such as curcumin,
- anti-MM lifestyle therapies such as exercise, whole body hyperthermia.
Don’t be surprised if your oncologist doesn’t consider therapies that haven’t been approved by the Food and Drug Administration (FDA) to be legitimate. This is your call of course but I have been pursuing the anti-MM therapies above and I’m doing pretty well. Non-conventional MM therapies work.
To Learn More About Solitary Bone Plasmacytoma- click now
If you have any questions about your diagnosis of an SPB, SPB, pre-myeloma, multiple myeloma, etc. scroll down the page, post a question or comment. I will reply to you ASAP.
Hang in there,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Arthritis, Joint Pain MGUS Symptom, Therapies
- Beating Myeloma: “If I Knew Then What I Know Now”
- Smoldering Multiple Myeloma- When to Treat?
Survival trends and prognostic factors in patients with solitary plasmacytoma of bone: A population‐based study
“Solitary plasmacytoma of bone (SPB) is a single, isolated plasmacytoma originated from the bone. The survival trends of patients with SPB in recent years remain unknown. And the prognostic system of SPB may also need to be refined.
…And the prognostic impacts of baseline characteristics and use of surgery was studied. A total of 4103 (from 1976 to 2016) cases of SPB were identified. The median age was 65 years old. Patients in time period‐2 (2008–2016) show better survival as compared to those in time period‐1(1976–2007) (median overall survival: 88 months vs. 73 months, p = 0.0332).
Age ≤ 65 years and being male were associated with better outcomes.
The widowed individuals had significantly inferior survival and myeloma‐specific survival than the single, married, or divorced individuals (p values all <0.0001).
Patients with lesions in bones of skull and face and associated joints had longer survival as compared with those with bone lesions in other sites (median overall survival: 107 months vs. 79 months, p = 0.0694).
The use of surgery was significantly associated with improved survival (median survival: surgery performed 98 months vs. not performed 73 months, hazards ratio [HR]: 0.7623, 95% CI: 0.7009–0.8472; p < 0.0001) and myeloma‐specific survival (median myeloma‐specific survival: surgery 160.0 months vs. no surgery 143.0 months, HR: 0.8469, 95% CI: 0.7493–0.9572; p = 0.0078)…
Solitary plasmacytoma refers to a single localized tumor consisting of monoclonal plasma cells without any clinical evidence of PCM or physical or radiographical evidence of additional plasma cell neoplasms.
Solitary plasmacytoma is relatively rare, accounting for only 3% of all plasma cell neoplasms. Based on the site of lesion, solitary plasmacytoma is classified into solitary plasmacytoma of bone (SPB) and solitary extramedullary plasmacytoma (SEP).1 SPB is a single, isolated plasmacytoma originated from the bone,2, 3 while solitary extramedullary plasmacytoma is characterized by the presence of plasma cells infiltrating in soft tissue mass.4, 5…
SPB accounts for 1–2% of plasma cell tumors. It shows male predominance, with 65% of patients being male. The median age at disease onset is approximately 55 years. Bones with active hematopoiesis are the most common sites involved by SPB. The most frequently affected bone is the vertebrae, which is followed by ribs, skull, and pelvic bones.
The standard therapy for SPB is radiotherapy, even in patients in whom the tumor is completely resected. Despite the high local control rate with radiotherapy, the rate of recurrence of SPB is high, with approximately two‐thirds of cases eventually progress to PCM or additional solitary or multiple plasmacytomas.
Therefore, it is important to find robust prognostic factors to identify patients who are at higher risk of relapse to use risk‐adapted therapy for treating patients with SPB. The risk factors for progression include older age, tumor size > 5 cm, and persistence of M protein for >1 year following radiation…
The effects of sites of lesions on patient outcomes
The specified information regarding locations of lesions was available for 3839 patients. Among these patients, the most frequently involved site was the vertebral column (1670, 43.5%), which was followed by bones of the pelvis (631, 16.4%) and bones of the chest (605, 15.8%). The sites of bone lesions had no significant impacts on the survival..
Surgery and outcomes
We then analyzed the impact of surgery on survival in patients with SPB. We found that the use of surgery was significantly associated with improved survival (median survival: surgery 98 months vs. no surgery 73 months..
DISCUSSION
Solitary bone plasmacytoma is a rare, malignant plasma cell disorder with a relatively high incidence of recurrence.11, 12…
According to the guidelines for the treatment of SPB, radiation remains the mainstay of the treatment.1, 18, 19 And radiotherapy provides long‐term local control in patients with SPB.18
Surgery without radiotherapy was associated with inferior outcomes in patients with SPB.20The added benefit of surgery to radiation in patients with SPB remains controversial. Some previous studies suggest that radiotherapy combined with surgery was associated with better outcomes in patients with SPB.20, 21 In our analysis, we found that patients who were treated with surgery had better survival and myeloma‐specific survival than those who did not receive surgery, suggesting surgery might improve the prognosis of patients with SPB. In patients with SPB in vertebral column, we found that use of surgery was associated with improved survival…