Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Gastrointestinal endoscopic ultrasound
Gastrointestinal endoscopic ultrasound
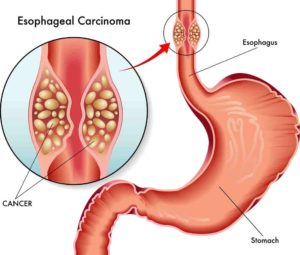
When Is Gastrointestinal endoscopic ultrasound (EUS) Necessary for a Newly Diagnosed Cancer of the Esophagus, Stomach, Colon, or Pancreas?
If you have been diagnosed with either Esophageal, Stomach, Colon, or Pancreatic cancer determining an accurate stage of your cancer is critical. It is your cancer’s stage that determines your prognosis and therapy plan. So the real question is not when is EUS necessary but when is it not necessary for newly diagnosed patients?
An important issue for cancer patients is to determine if their oncologist and the associated cancer center is well-versed, experienced in managing your type and stage of cancer. The local community hospital may not have handled many cases of your specific type of cancer.
Your community hospital may not offer certain types of diagnostic testing required give you the important information that you need.
I am both a cancer survivor and cancer coach. Have you been diagnosed with cancer? What type? What stage? My mission is to provide cancer patients with the information they need to manage their cancer.
Please scroll down the page, post a question or comment and I will reply to you ASAP.
Thank you,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- I have Barrett’s Esophagus- what are my options?
- Barrett’s Esophagus- Diagnosis, Prognosis and Treatment
- Ask the Cancer Coach-“Stage 4 esophageal cancer diagnosis and treatment”
Understanding EUS (Endoscopic Ultrasonography)
“What is EUS?
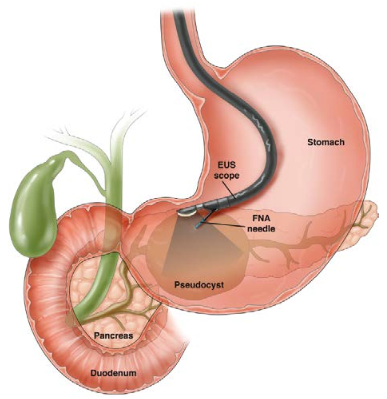
Endoscopic ultrasonography (EUS) allows your doctor to examine your esophageal and stomach linings as well as the walls of your upper and lower gastrointestinal tract. The upper tract consists of the esophagus, stomach and duodenum; the lower tract includes your colon and rectum. EUS is also used to study other organs that are near the gastrointestinal tract, including the lungs, liver, gall bladder and pancreas.
Endoscopists are highly trained specialists who welcome your questions regarding their credentials, training and experience. Your endoscopist will use a thin, flexible tube called an endoscope that has a built-in miniature ultrasound probe. Your doctor will pass the endoscope through your mouth or anus to the area to be examined. Your doctor then will use the ultrasound to use sound waves to create visual images of the digestive tract.
Why is EUS done?
EUS provides your doctor with more information than other imaging tests by providing detailed images of your digestive tract. Your doctor can use EUS to diagnose certain conditions that may cause abdominal pain or abnormal weight loss.
EUS is also used to evaluate known abnormalities, including lumps or lesions, which were detected at a prior endoscopy or were seen on x-ray tests, such as a computed tomography (CT) scan. EUS provides a detailed image of the lump or lesion, which can help your doctor determine its origin and help treatment decisions. EUS can be used to diagnose diseases of the pancreas, bile duct and gallbladder when other tests are inconclusive or conflicting.
Why is EUS used for patients with cancer?
EUS helps your doctor determine the extent of spread of certain cancers of the digestive and respiratory systems. EUS allows your doctor to accurately assess the cancer’s depth and whether it has spread to adjacent lymph glands or nearby vital structures, such as major blood vessels. In some patients, EUS can be used to obtain a needle biopsy of a lump or lesion to help your doctor determine the proper treatment.
EUS Utility Varies Among Gastrointestinal Cancers
“A: Gastrointestinal endoscopic ultrasound (EUS) is an important tool for cancer staging because many treatment algorithms are determined by EUS tumor staging…
Computed tomography (CT) scan should generally be obtained before EUS to determine whether there is any metastatic disease that would make the patient a nonsurgical candidate…
If there is no evidence of metastatic disease, then EUS should be performed for locoregional staging. The tumor-node-metastases (TNM) staging system is used for luminal GI and pancreatic cancer. The EUS accuracy for staging GI and pancreatic cancer is approximately 85% for T-staging and 75% for N-staging…
The time to use EUS in cancer staging is before the patient receives any chemoradiation. Staging accuracy significantly decreases after chemoradiation because EUS cannot distinguish between peritumoral inflammation/edema and the actual tumor…