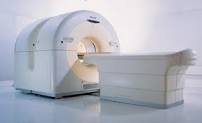
The new technology, known as photon-counting detector CT, debuted in the clinic in 2021 after decades of development. By directly converting individual x-ray photons into an electric signal, photon-counting detector CT can decrease the detector pixel size and improve the image’s spatial resolution.
“Additionally, photon-counting CT has demonstrated much better dose efficiency than standard CT, which allows for acquisition of ultra-high-resolution images of large areas of the body…”
The researchers also applied a deep learning AI technique developed at Mayo Clinic’s CT Clinical Innovation Center to reduce the noise in the very sharp photon-counting images. CT noise refers to an unwanted change in pixel values in the image, often loosely defined as the grainy appearance on cross-sectional imaging. The photon-counting detector CT with deep learning noise reduction demonstrated improvement in visualization and detected more lesions relative to conventional CT…
“We were excited to see that not only were we able to detect these features of multiple myeloma disease activity more clearly on the photon-counting scanner,” Dr. Baffour said, “with deep learning denoising techniques that allowed us to generate thinner image slices, we were able to detect more lesions than on the standard CT.” “
Prospective Multireader Evaluation of Photon-counting CT for Multiple Myeloma Screening
“Purpose- To determine whether photon-counting CT (PCCT) acquisition of whole-body CT images provides similar quantitative image quality and reader satisfaction for multiple myeloma screening at lower radiation doses than does standard energy-integrating detector (EID) CT…
Results ...PCCT helped identify more lesions… CNRs and SNRs were similar between modalities. PCCT had lower radiation doses than EID…dose-length product: EID, 1654.1 ± 409.6 vs PCCT, 253.4 ± 89.6…
Conclusion- This pilot investigation suggests that PCCT affords similar quantitative and qualitative scores as EID at significantly lower radiation doses…”
Radiology’s Ionising Radiation Paradox: Weighing the Indispensable Against the Detrimental in Medical Imaging
“Abstract– Ionising radiation stands as an indispensable protagonist in the narrative of medical imaging, underpinning diagnostic evaluations and therapeutic interventions across an array of medical conditions. However, this protagonist poses a paradox – its inestimable service to medicine coexists with an undercurrent of potential health risks, primarily DNA damage and subsequent oncogenesis…
Such techniques are vital in the early detection, accurate diagnosis, and successful treatment of various diseases, underpinning the crucial role of radiology in advancing patient care. Despite their remarkable diagnostic capabilities, these imaging techniques expose patients to ionising radiation, potentially increasing cancer incidence [6]…
Computed Tomography (CT)
CT scans transcend standard imaging, producing intricate cross-sectional images using a rotating X-ray beam coupled with detector arrays [1]. Despite its diagnostic prowess, the increased complexity and sophistication of CT imaging also introduce higher radiation doses, delivering a radiation dose generally between 2 and 20 mSv [1,6]…