However, quality of life deteriorates significantly for one in six (esophagectomy) patients to a level that remains much lower than the average population in the five years after surgery.
With most diagnoses of cancer, an early diagnosis means minimal therapy and a late-stage diagnosis means aggressive therapy. In the case of late-stage Esophageal Cancer, “the only established curative treatment includes extensive surgery, often of the abdomen, chest, and throat.” An esophagectomy often means an impaired quality of life.
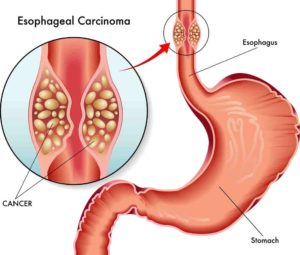
The top article puts responsibility for identifying EC patients with a poor quality of life on hospitals. I disagree. Years of living as a cancer survivor and as a cancer coach have taught me that it is EC patients themselves who know how they are doing, feeling and living.
Further, conventional medicine simply does not know much about nutrition, supplementation, and other lifestyle therapies shown to build the cancer survivor’s health and immune function.
I am both a cancer survivor and cancer coach. I work with patients to identify therapies shown to achieve their goals.
For more information about non-conventional, non-toxic therapies to manage EC, scroll down the page, post a question or comment and I will reply to you ASAP.
Thank you,
David Emerson
- Cancer survivor
- Cancer Coach
- Director PeopleBeatingCancer
“A new study shows that most patients who survive for at least five years after esophageal cancer surgery recover an average quality of life. However, quality of life deteriorates significantly for one in six patients to a level that remains much lower than the average population in the five years after surgery. This suggests, say the researchers, that hospitals must be better at identifying this patient group…
“The patients who show early signs of impaired quality of life should be identified and helped through a more intensive follow-up to avoid a persistently low quality of life,”
Depending on the problems identified by the patients, targeted intervention is often possible. For example, a patient with particular nutritional problems can be referred to a dietician with specialist knowledge of this patient group.”
Background: Esophagectomy represents an exemplar of controlled major trauma, with marked metabolic, immunologic, and physiologic changes as well as an associated high incidence of complications. Eicosapentaenoic acid (EPA) enriched enteral nutrition (EN) modulates immune function and limits catabolism in patients with advanced cancer, but its impact in the peri-operative period is unclear.
Conclusions: EPA supplemented early EN is associated with preservation of lean body mass post esophagectomy compared with a standard EN. These properties may merit longer-term study to address its impact on the recovery of function and quality of life in models of complex surgery or multimodal cancer treatment regimens.





