
Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- Newly Diagnosed »
- Barrett’s Esophagus- High-Grade Dysplasia Overdiagnosis?
Barrett’s Esophagus- High-Grade Dysplasia Overdiagnosis?
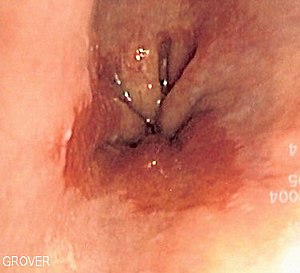
“Numerous histological mimics of high-grade dysplasia in Barrett’s esophagus predispose to overdiagnosis and potential serious mismanagement, including unnecessary esophagectomy.”
High-Grade Dysplasia in Barrett’s Esophagus (pre-esophageal cancer), DCIS (pre-breast cancer), and cervical dysplasia (pre-cervical cancer) , etc. have two important things in common. First, all are NOT cancer. Second, all three of these diagnoses can increase your risk of getting cancer. According to the article linked and excerpted below, high-grade dysplasia in Barrett’s Esophagus is WAY over-diagnsosed.
I consider trying not to “get cancer” the same way I approach remaining in complete remission from my cancer, multiple myeloma- an incurable blood cancer.
- Nutrition,
- Supplementatioin
- Lifestyle
Make no mistake- any cancer is difficult to assess under a microscope. But the one immutable truth I have learned as a cancer survivor of an incurable cancer, your diagnosis is used to design your treatment plan.
Therefore an accurate diagnosis of your “pre-cancer” is important to you.
Please consider the following-
- Get a second opinion
- Lower your risk of Barret’s Esophagus (high or low dysplasia) from becoming Esophageal Cancer through evidence-based nutrition, supplementation and anti-oxidants.
Have you been diagnosed with Barrett’s Esophagus? Do you have heartburn or G.E.R.D? High or low dysplasia? Any symtpoms? Scroll down the page, post a question or a comment and I will reply to you ASAP.
Thanks
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- I have Barrett’s Esophagus- what are my options?
- Barrett’s Esophagus- Diagnosis, Prognosis and Treatment
- Ask the Cancer Coach-“Stage 4 esophageal cancer diagnosis and treatment”
Overdiagnosis of High-grade Dysplasia in Barrett’s Esophagus: A Multicenter, International Study
“Numerous histological mimics of high-grade dysplasia in Barrett’s esophagus predispose to overdiagnosis and potential serious mismanagement, including unnecessary esophagectomy. This study investigates the prevalence and sources of this problem.
Biopsies from 485 patients diagnosed with Barrett’s high-grade dysplasia were screened for a multi-institutional, international Barrett’s endoscopic ablation trial. Screening included review of the original diagnostic slides and an additional protocol endoscopy with an extensive biopsy sampling. Observer variability by the study pathologists was assessed through two blinded diagnostic rounds on 437 biopsies from 26 random study endoscopies. Study diagnostic reassessments revealed significantly lower rates of high-grade dysplasia. Only 248 patients (51%) were confirmed to have high-grade dysplasia. The remaining patients had inflamed gastric cardia without Barrett’s (n=18; 7%), Barrett’s without dysplasia (n=35; 15%), indefinite change (n=61; 26%), low-grade dysplasia (n=79; 33%), adenocarcinoma (n=43; 18%), and other (n=1; <1%), yielding an alarming total of 194 or 40% of patients who were overdiagnosed with Barrett’s high-grade dysplasia. Study pathologists achieved a high-level agreement (90% three-way inter-observer agreement per biopsy, Kappa value 0.77) for high-grade dysplasia. Confounding factors promoting overdiagnosis included Barrett’s inflammatory atypia (n=182), atypia limited to the basal metaplastic glands (n=147), imprecise criteria for low grade neoplasia (n=102), tangential sectioning artifact (n=59), and reactive gastric cardiac mucosa (n=38). A total of 194 patients (40%) were overdiagnosed with Barrett’s high-grade dysplasia, as affirmed by the extensive screening process and high-level study pathologist agreement. The multiple diagnostic pitfalls uncovered should help raise pathologists’ awareness of this problem and improve diagnostic accuracy.
Diagnosis and grading of dysplasia in Barrett’s oesophagus
“This review focuses on the pathological features of dysplasia in Barrett’s oesophagus. Two categorisation schemes are used for grading dysplasia in the gastrointestinal tract, including Barrett’s oesophagus. The inflammatory bowel disease dysplasia morphology study group system is the one most commonly used in the USA. However, some European and most far Eastern countries use the Vienna classification system, which uses the term “non‐invasive neoplasia” instead of low‐grade dysplasia (LGD) or high‐grade dysplasia (HGD) and also uses the term “suspicious for invasive carcinoma” for lesions that show equivocal cytological or architectural features of tissue invasion.
The degree of dysplasia is based on a combination of cytological and architectural atypia. However, the precise number of HGD crypts that is necessary to upgrade a biopsy from LGD to HGD has never been investigated and varies widely among expert gastrointestinal pathologists.
The extent of dysplasia, particularly LGD, has also been recognised recently as an important prognostic parameter in Barrett’s oesophagus. Other problematic areas of dysplasia interpretation include differentiation of regenerating epithelium versus LGD and separating HGD from carcinoma.
Dysplasia associated with macroscopically visible lesions, such as ulcers, nodules or polyps, carry a high risk of synchronous or metachronous adenocarcinoma. Recently, immunostaining for α‐methylacyl‐CoA‐racemase has been shown to have a high degree of specificity for detection of dysplasia in Barrett’s oesophagus and may be used to help distinguish negative from positive biopsies in this condition. In this review, the problematic areas in dysplasia interpretation are outlined and a specific approach to these issues is discussed…”


