Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Heart Failure + Surgery = Higher Risk of Death
Heart Failure + Surgery = Higher Risk of Death

They found that within 90 days after surgery, 10.1 percent of heart failure patients who had symptoms from their heart condition died.
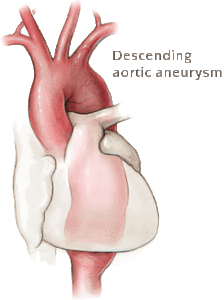
I developed chronic atrial fibrillation (afib) in the fall of 2010. The report that I received from that appointment with my cardiologist reported that my aorta was dilated and that I developed chemotherapy-induced cardiomyopathy.
An appointment with a different cardiologist in 2015 identified further dilation.
Skip ahead four years. An appointment on 1/2/19 showed that my aorta had dilated further. My cardiologist called me after the appointment and urgently counseled me to have surgery to treat my dilated aorta.
There was no mention of my 10% risk of death due to my heart failure. A long-term side effect created by cardiotoxic chemotherapy in 1995 had created an urgent need for open-heart surgery in 2019.
As a long-term cancer survivor I’m well aware that all therapies have risks. All therapies have side effects. In the case of HF patients undergoing surgery, the risk of death, according to the article linked below, is more than 10%.
While I understand all therapies carry risks, I do expect physicians to explain these risks in detail to their patients. I consider this information to be the job of the M.D.
That is a very high risk and a very serious side effect.
So what is my solution? What is my plan to avoid surgery for the rest of my life? Cardiac Rehabilitation. To be honest, I may have to undergo surgery someday. And I may have to take conventional heart meds such as beta blockers, ACE inhibitors, etc. someday.
But my goal is to avoid the short, long-term and late stage of conventional heart therapies as long as I can with evidence-based, non-toxic cardiac rehabilitation such as
- nutrition,
- supplementation,
- daily moderate exercise and more
To learn more about evidence-based, non-toxic heart therapies, scroll down the page, post a question or comment and I will reply to you ASAP.
Thank you,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- CoQ10 to Improve Ejection Fraction in Congestive Heart Failure
- CoQ10/Ubiquinol for Heart Disease But for Prostate Cancer Too?
- Chemotherapy-induced Heart Failure- Cardiac Rehabilitation Prevent, Heal?
Heart failure boosts risk of death following surgery
“Patients with heart failure are more likely to die after surgery than patients without HF, a study led by surgeon Sherry Wren, MD, has found. The higher mortality rate held even when the researchers considered that HF patients are generally in poor health and are more likely to undergo complex surgeries.
“We adjusted for the level of surgery complexity,” said Ben Lerman, a fourth-year medical student who was the lead author on the study. “We also split up patients by the degree of HF, comparing like to like. That effect, the higher mortality, remains.”
In other words, if you take two 80-year-old male patients with the same health problems, except that one has HF and the other doesn’t, and perform the same surgery on them, the one with HF is more likely to die.
Even patients with the least severe HF — a group that Wren said has never been studied — suffered higher mortality after surgery…
HF, a condition in which the heart is unable to adequately pump blood throughout the body, is relatively common: 5.7 million people in the U.S. live with HF. It is also progressive: About half will die within five years of diagnosis.
Surgeons are aware that HF is a risk factor, Wren said, but prior research hadn’t quantified the risk. “I really felt that there was an underappreciation by surgeons, cardiologists and internal medicine doctors that HF, especially non-symptomatic or non-severe heart failure, had on postoperative death risk,” she said…
- They found that within 90 days after surgery, 10.1 percent of heart failure patients who had symptoms from their heart condition died.
- For asymptomatic heart failure patients, that number was 4.9 percent,
- and for patients without heart failure, it was 1.2 percent.
While all HF patients showed higher death rates, Wren said, “the worse the HF, the greater the mortality.”
The researchers conjectured that HF patients may not tolerate anesthesia as well as patients without heart failure. “Surgery is a massive physiological stress on even a healthy body,” Lerman said. “Even when patients’ hearts can handle everyday life, it seems they sometimes can’t handle the stress of surgery.”
Lerman and Wren said that they hope their findings are included in the American College of Surgeons’ risk calculator, which helps clinicians determine the chance of complications or death following surgery. They’d also like to see more physicians telling their HF patients about the risks, especially for surgeries that are non-essential.
“Five percent represents a high risk,” Wren said. “Patients and physicians need to have better discussions about those risks.”