“Persistent pain and sensory disturbances following surgical treatment for breast cancer is a significant clinical problem. The pathogenic mechanisms are complex…”
An article titled “Breast Cancer May Be Gone, but Pain Lingers” details a research study that shows a high prevalence of pain after treatment for breast cancer.
The article brings up some important points. I suspect that some of the pain has to do with damaged nerves, especially in those with extensive surgery. In my case, the surgery was not extensive, yet there is still some discomfort when pressure is applied — a minor problem. Like the article says, I used to worry that this might mean a recurrence, but after seven years I have pushed those worries aside, at least in that I think of it only occasionally as opposed to very frequently.
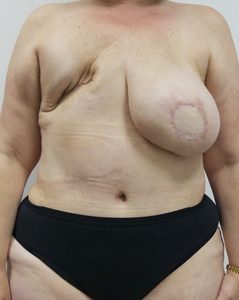
I don’t know if my pain is associated with the surgery or with the radiation, but I think the radiation can sometimes make it much worse. My friend, who had a very radical surgery, was recovering nicely and mostly pain-free until her extensive (even her supraclavicular nodes) radiation began. She quickly began to feel her muscles and tendons stiffening and was left with pain and pneumonitis after the radiation. She also has pain related to lymphedema which started after the radiation therapy.
I find it odd that oncologists might be unaware of the pain. I certainly mentioned my little dab of pain to my oncologist several times before deciding it was “normal” for me.
To Learn More about Lymphedema- click now
Mary Miller BC Profile in Courage
JAMA. 2009 Nov 11;302(18):2034-5.
Arch Surg. 2010 Mar;145(3):224-5.
Women’s Health (Lond Engl). 2010 Mar;6(2):175-7.
CONTEXT: Persistent pain and sensory disturbances following surgical treatment for breast cancer is a significant clinical problem. The pathogenic mechanisms are complex and may be related to patient characteristics, surgical technique, and adjuvant therapy.
OBJECTIVE: To examine the prevalence of and factors associated with persistent pain after surgical treatment for breast cancer.
DESIGN, SETTING, AND PATIENTS: A nationwide cross-sectional questionnaire study of 3754 women aged 18 to 70 years who received surgery and adjuvant therapy (if indicated) for primary breast cancer in Denmark between January 1, 2005, and December 31, 2006. A study questionnaire was sent to the women between January and April 2008.
MAIN OUTCOME MEASURES: Prevalence, location, and severity of persistent pain and sensory disturbances in 12 well-defined treatment groups assessed an average of 26 months after surgery, and adjusted odds ratio (OR) of reported pain and sensory disturbances with respect to age, surgical technique, chemotherapy, and radiotherapy. RESULTS: By June 2008, 3253 of 3754 eligible women (87%) returned the questionnaire. A total of 1543 patients (47%) reported pain, of whom 201 (13%) had severe pain, 595 (39%) had moderate pain, and 733 (48%) had light pain. Factors associated with chronic pain included young age (18-39 years: OR, 3.62; 95% confidence interval [CI], 2.25-5.82; P < .001) and adjuvant radiotherapy (OR, 1.50; 95% CI, 1.08-2.07; P = .03), but not chemotherapy (OR, 1.01; 95% CI, 0.85-1.21; P = .91). Axillary lymph node dissection (ALND) was associated with increased likelihood of pain (OR, 1.77; 95% CI, 1.43-2.19; P < .001) compared with sentinel lymph node dissection. Risk of sensory disturbances was associated with young age (18-39 years: OR, 5.00; 95% CI, 2.87-8.69; P < .001) and ALND (OR, 4.97; 95% CI, 3.92-6.30; P < .001). Pain complaints from other parts of the body were associated with increased risk of pain in the surgical area (P < .001). A total of 306 patients (20%) with pain had contacted a physician within the prior 3 months for pain complaints in the surgical area. CONCLUSION: Two to 3 years after breast cancer treatment, persistent pain and sensory disturbances remain clinically significant problems among Danish women who received surgery in 2005 and 2006.