Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Pre-Cancer- OverDiagnoses, OverTreatment?
Pre-Cancer- OverDiagnoses, OverTreatment?
Even the word pre-cancer can be terrifying. I read the fear in newly diagnosed patients writing in online groups daily. Let’s face it. The word cancer strikes fear into all who are diagnosed with it. Regardless of your prognosis.
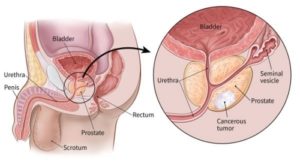
According to the NYT opinion article linked below, two board-certified surgical oncologists are calling for the pre-cancer stages of breast and prostate cancer- ductal carcinoma in-situ (DCIS) and Gleason 6- breast and prostate respectively, to no longer be referred to as cancer.
According to the oncologists, referring to these pre-cancer stages as cancer simply scares many newly diagnosed patients into aggressive treatments that can result in short, long-term and late stage side effects. For diagnoses that would probably never result in health problems anyway.
An everyday example of the idea of pre-cancer is that men die with prostate cancer IN their prostates even though they die of something other than prostate cancer.
PeopleBeatingCancer offers many examples of pre-cancer that should not be called cancer and may be over-treated as a result. Over-treatment that can result in side effects without changing the prognosis.
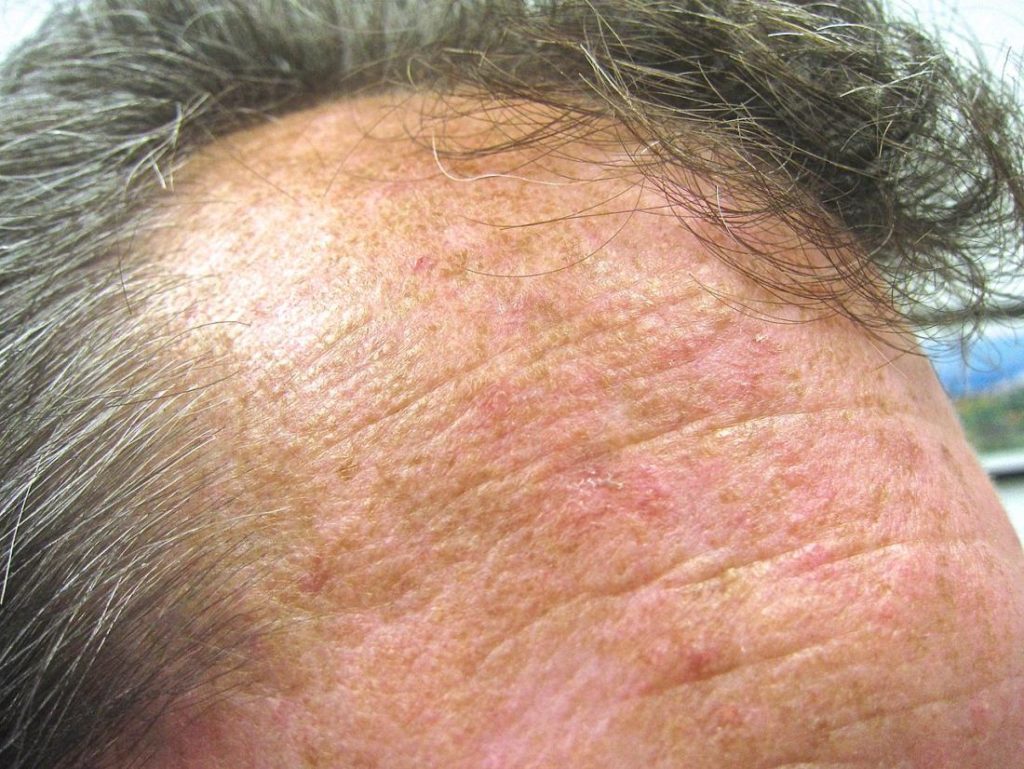
The image in the upper right corner of this post is of a man’s bald head covered with actinic keratosis- a form of pre-cancer for skin cancer. According to the Skin Cancer Foundation, there were more than 58 millions Americans affected by AK diagnoses. Reducing a person’s risk of skin cancer can be accomplished with nutrition, supplementation and lifestyle therapies.
- Actinic Keratoses- Skin Cancer But Not Skin Cancer
- Dysplasia of the Tongue-Reduce Risk of Cancer?
- Non-Toxic Pre-Myeloma Therapies
- Earl Kielley – Reverse pre-cancerous prostate cancer
- DCIS: Overdiagnosis and Overtreatment?
- Prostate Cancer- Low risk- Non-Toxic Therapies
Have you been diagnosed with a stage of pre-cancer such as DCIS or prostate cancer with a Gleason scare of 6? If you would like to learn more about non-toxic therapies cited to reduce your already low risk of progression, scroll down the page, post a question or a comment and I will reply to you ASAP.
Thank you,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Not Everything We Call Cancer Should Be Called Cancer
“Laura Esserman and
Dr. Esserman is a surgeon and breast cancer oncologist at the University of California, San Francisco. Dr. Eggener is a surgeon and urologic oncologist at the University of Chicago.
“You Have Cancer.” Ask anyone who has been told this: It’s terrifying.
That’s one reason we need to rethink what we call cancer. Despite amazing advances in our understanding of the disease, we have neglected to update how we define what has been called the emperor of all maladies.
Some pre-cancers have extraordinarily low risks of altering the quality or length of life but get lumped in with those that do. And that often leads to unnecessary treatment, disfigurement, side effects and a constellation of other psychological, relationship and financial issues…
But as newer and more sensitive technologies come into use, we are increasingly identifying medical conditions that might have gone undetected without any issues. This phenomenon of overdiagnosis is a well-documented consequence of screenings for breast and prostate cancer…
Early detection of cancer sounds intuitively attractive and in many cases saves lives. But automatically calling something cancer can lead to aggressive treatment, even if the cancer in question is unlikely to cause problems.
For many cancers (stages if pre-cancer), the term simply doesn’t match how the disease behaves.
Let’s look at two examples.
- For prostate cancer, a biopsy showing a grade of Gleason 6 (also known as Grade Group 1) is considered low or very low risk.
- In breast cancer, diagnosis of ductal carcinoma in situ, or D.C.I.S., is similarly low or very low risk, indicating the very earliest, noninvasive stage of the disease.
These findings- Gleason 6 and DCIS, make up about 20 percent to 25 percent of prostate and breast cancer diagnoses in the United States, involving about 100,000 people annually. These patients are routinely treated with surgery or radiation, even though their conditions are not life threatening and cause no symptoms at the time they are spotted. To our knowledge, neither Gleason 6 nor D.C.I.S. spreads to other parts of the body unless more aggressive forms of cancer develop or are simultaneously present. They are more accurately explained as risk factors for prostate or breast cancers with malignant potential…
Renaming very low-risk cancers would make it easier to persuade patients when it’s appropriate to adopt monitoring and risk reduction as their approaches. Early-stage “cancers” that meet the microscopic definition of the disease (what a pathologist sees through the microscope) but not the clinical definition (a condition that is highly likely to grow and cause symptoms and has the potential to kill a person) could be designated as IDLE (indolent lesion of epithelial origin) or preneoplasia — anything but the dreaded C-word…
Changing the label would make matters considerably less stressful for patients and their families. It would greatly reduce unnecessary treatment. The financial and psychological benefits for patients would be profound. Screening for life-threatening cancers would improve…
By modifying the names of early-stage prostate and breast “cancer” to appropriately reflect how they behave, we’d reduce unnecessary treatments and their side effects and improve screening, prevention and care.”