Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Chemotherapy-induced Liver Damage
Chemotherapy-induced Liver Damage
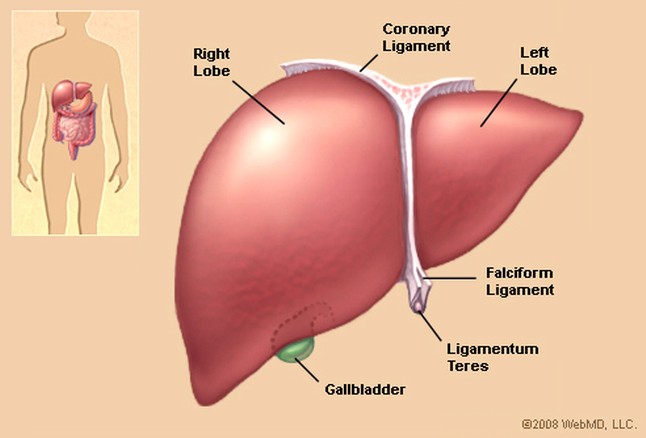
Chemotherapy-induced liver damage is not about the type of cancer you have but the type of FDA approved “safe and effective” therapy you are prescribed. And, according to the first two studies linked and excerpted below there is a long and growing list of regimens that can cause chemotherapy-induced liver damage.
While you probably won’t die from chemotherapy-induced liver damage, you may very well sustain long-term damage to your liver function as is outlined in the last study linked below.
If you are fortunate enough to be reading this post after your cancer diagnosis but before you have begin undergoing chemotherapy then you need to pre-habilitate with one or more of the evidence-based non-conventional therapies listed below shown to protect the liver from chemotherapy-induced liver damage.
If you have already undergone chemo and you have already sustained liver damage (such as two of the posts linked below) your choices are to discuss a therapy vacation/break with your oncologist giving your liver a chance to heal and/or undergo the of the hepto-protective therapies such as milk thistle shown to protect liver health.
Chemotherapy-induced liver damage surprisingly common yet treatable with evidence-based non-conventional therapies-
- Dark Coffee- Bone, Liver, Kidney Health for the Myeloma
- Multiple Myeloma Diet- Liver Enzymes, Inflammation
- Myeloma- Milk Thistle, Silymarin, Liver Healing
- Curcumin- Cirrhosis of the Liver
- Myeloma Symptoms, Side Effects- Liver Damage
Diagnostic tests that look at liver function include:
- Alanine transaminase (ALT)
- Aspartate transaminase (AST)
- Alkaline phosphatase (ALP)
- Albumin and total protein
- Bilirubin
- Gamma-glutamyltransferase (GGT)
- L-lactate dehydrogenase (LD)
- Prothrombin time (PT)
Have you been diagnosed with chemotherapy-induced liver damage? Are your bilirubin levels out of the normal range? Scroll down the page, post a question or a comment and I will reply to you ASAP.
Hang in there,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Management of hepatotoxicity of chemotherapy and targeted agents
“Hepatotoxicity of chemotherapeutic agents such as
- methotrexate,
- oxaliplatin, and
- irinotecan
have been well documented and characterized allowing for careful management by oncologists during administration. However, the rapid advance of the field of oncology and introduction of new classes of therapies such as small molecule inhibitors and immunotherapies have introduced new hepatotoxicity challenges and management strategies…”
Management of hepatotoxicity of chemotherapy and targeted agents
“A wide variety of drugs exhibit hepatotoxicity that must be monitored for including, but not limited to, drugs such as
- acetaminophen,
- amiodarone,
- amoxicillin-clavulanate,
- and the statins.
Additionally, conventional chemotherapeutic agents have well characterized hepatotoxic effects with some of the most common identified agents including methotrexate, irinotecan, and oxaliplatin [8]. Hepatotoxicity related to administration of chemotherapeutic agents includes
- elevations of liver function tests (LFTs),
- drug-induced hepatitis,
- veno-occlusive disease,
- steatohepatitis,
as well as potential chronic manifestations such as fibrosis and liver failure [9–11]…
Agents that have been shown to cause increased hepatotoxicity in conjunction with radiation therapy include
Classes of chemotherapies that cause hepatotoxicity include-
- antitumor antibiotics,
- alkylating agents,
- platinum agents,
- antimetabolites,
- antimicrotubular agents, and
- topoisomerase inhibitors.
The rest of this review will place more focus on the hepatotoxicity of new classes of anticancer therapies. These targeted agents include:
- anti-HER-2 therapies,
- targeted small molecule inhibitors such as VEGF and tyrosine kinase inhibitors,
- immune checkpoint inhibitors (ICI), and
- chimeric antigen receptor T (CAR-T) cells
Chemotherapy typically induces cellular damage that results in impaired cell division or apoptosis of rapidly dividing cells. The nonselective characteristics of traditional chemotherapeutic agents result in off target adverse effects including, but not limited to, hepatotoxicity…
Recently published case reports of chemotherapy related hepatotoxicity include toxicity related to oxaliplatin treatment as well as a cisplatin and 5-FU regimen [38,39]…
Conclusions-In conclusion, hepatotoxicity represents a common clinical manifestation that is associated with a variety of anticancer therapies. The inherent toxicity of anticancer therapies requires oncologists to maintain a broad awareness of their effects on the body, including the liver. As novel anticancer therapies are developed, especially targeted agents, clinicians must remain informed their new side effects, including hepatotoxicity…”
What might help protect the liver during chemotherapy?
“Many chemotherapy medications rely onTrusted Source the liver for metabolization. However, some can cause severe liver damage. Chemotherapy medications may causeTrusted Source mild liver problems, and combination therapies can worsen these effects…
How to protect the liver-
Milk thistle: According to a 2020 studyTrusted Source, silymarin extracted from milk thistle may help protect the liver from the effects of chemotherapy…
Curcumin- Palipoch et al. (2014) found that curcumin pretreatment could decrease liver lipid peroxidation and NADPH oxidase expression in cisplatin-treated rats to prevent cisplatin-associated liver damage. Curcumin is also proven to protect mitochondria from chemotherapy-induced oxidative stress…”
Omega-3 fatty Acids- “In the many, large, randomized controlled trials of the omega-3 fatty acids, side effects have been minimal. Use of omega-3 fatty acids even in high doses has not been linked convincingly to serum enzyme elevations or to instances of clinically apparent liver injury…”
Traditional Chinese Medicine: An older study from 2011Trusted Source suggests that traditional Chinese Medicine may help improve or maintain liver function during chemotherapy treatment…
Eating foods with antioxidants: A 2015 studyTrusted Source indicates that some foods and supplements containing antioxidants may help prevent liver damage…
Chemotherapy induced liver abnormalities: an imaging perspective
“Conditions such as SOS, steatosis, pseudocirrhosis, and even hepatic necrosis can occur as a direct result of chemotherapy, which may simulate a clinical presentation of long term hepatic damage and cirrhosis…”