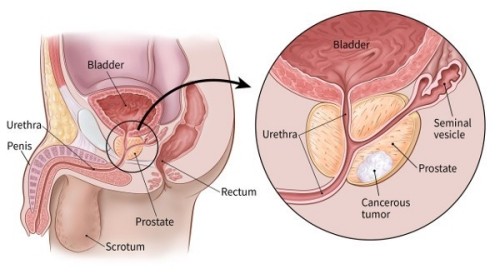
“Active Surveillance” is based upon the prolonged natural history of low-risk prostate cancer and is an attempt to balance the risks and side effects of over-treatment against the possibility of disease progression and a lost opportunity for cure.”
Low-risk prostate cancer is an excellent example of what years of research and experience have shown me. Many early cancers are over-diagnosed and over-treated.
The second study linked below explains that most low-risk prostate cancer patients understand the benefit of active surveillance or watchful waiting.
But let me take this idea one step further. Consider undergoing evidence-based, non-toxic therapies while you actively surveil your low-risk prostate cancer.


Curcumin and vitamin D3 are just two of the non-toxic anti-PCa therapies that I’m referring to. Nutrition, frequent, moderate exercise and many other therapies have been shown to fight prostate cancer.
If you have been diagnosed with low-risk prostate cancer then you have already made the decision not to actively treat your PCa with toxic therapies. Consider evidence-based but Non-Toxic therapies shown to fight prostate cancer.
To Learn More About Prostate Cancer- click now
To Learn More About Low-Risk Prostate Cancer- click now
Scroll down the page, post a question or a comment and I will reply to you ASAP.
Hang in there,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
“Active surveillance for localized prostate cancer entails initial expectant management rather than immediate therapy, with “curative-intent” treatment deferred until there is evidence that the patient is at increased risk for disease progression.
This is a response to the clearly documented risks of over diagnosis and overtreatment of low-risk prostate cancer, which in most cases poses little or no threat to the patient. It is based upon the prolonged natural history of prostate cancer and is an attempt to balance the risks and side effects of overtreatment against the possibility of disease progression and a lost opportunity for cure. Low-risk prostate cancer is more accurately viewed as one of multiple risk factors for the presence of higher grade prostate cancer. Like atypical small acinar proliferation, (ASAP), it may be managed with close follow up but without radical intervention, unless there is clear evidence of more aggressive disease.
“The number of men with prostate cancer who opted for active surveillance (AS) doubled nationally between 2014 and 2021, according to experts who say the dramatic increase reflects a growing understanding among both researchers and patients that low-grade prostate tumors can be safely watched for years without requiring treatment.
Roughly 60% of men eligible for AS chose that approach in 2021, up from 27% in 2014 and less than 10% in 2010.
Cooperberg attributed the hike in AS rates in the United States to the growing scientific literature and guidelines supportive of the approach, which calls for periodic assessments of low-risk tumors but no surgery, radiation, or other therapies. In Canada and parts of Europe, approximately 80%-90% of men who are eligible for AS choose that approach, experts said…
In 2012, the US Preventative Services Task Force (USPSTF) recommended against screening for prostate-specific antigen (PSA), concluding that the benefits of the test did not outweigh the risks, such as overdiagnosis and overtreatment of low-risk prostate cancer….
In 2018, following protests by urologists and patient advocates, the USPSTF revised its statements to include shared decision-making for PSA testing in men aged 55-69 years, reflecting emerging evidence of longer-term benefits and widespread adoption of active surveillance after detection of low-risk disease, he said…
Cooperberg said financial incentives are real. “I think it’s a small minority of docs that are heavily driven by the financial incentive, but it certainly exists,” he told Medscape. When you look at the extreme variation of active surveillance rates, there is no question that factors like reimbursement are going to play a role…”
“The variability of AS adoption among practices and physicians varies from 0% to 100%. Therefore, some are too ‘tight’ in recommending AS and some are ‘too loose.’ I do not attempt to steer [patients] into treatment unless I believe that would be their best option. Nevertheless, some opt for surveillance when I believe they are making a mistake, and some opt for treatment when I believe surveillance would have been a rational choice.”
Cooperberg agreed that a personalized approach is important and that both physicians and patients should be flexible in their decision-making. “There will always be some men with low-grade disease who should get immediate treatment. For example, a young man with very high-volume disease, even if it’s Gleason 3+3,” he said. “If it is clearly inevitable that he’s going to need treatment, he could reasonably make a decision to get immediate treatment…”
“The long latency and high incidence of prostate carcinogenesis provides the opportunity to intervene with chemoprevention in order to prevent or eradicate prostate malignancies. We present here an overview of the chemopreventive potential of curcumin (diferuloylmethane), a well-known natural compound that exhibits therapeutic promise for prostate cancer.
In fact, it interferes with prostate cancer proliferation and metastasis development through the down-regulation of androgen receptor and epidermal growth factor receptor, but also through the induction of cell cycle arrest. It regulates the inflammatory response through the inhibition of pro-inflammatory mediators and the NF-κB signaling pathway. These results are consistent with this compound’s ability to up-induce pro-apoptotic proteins and to down-regulate the anti-apoptotic counterparts. Alone or in combination with TRAIL-mediated immunotherapy or radiotherapy, curcumin is also reported to be a good inducer of prostate cancer cell death by apoptosis. Curcumin appears thus as a non-toxic alternative for prostate cancer prevention, treatment or co-treatment…”
“Vitamin D promotes the differentiation of prostate cancer cells, raising the possibility that vitamin D deficiency over time may contribute to the progression from subclinical prostate cancer to clinical disease. Since low-risk prostate cancers are monitored over time in an effort to determine which progress into clinically important, more aggressive cancers, they provide an excellent model in which to study, over an extended period of time, the effects of enhancing vitamin D status and related changes in tumor progression.
This is particularly relevant to African-American men, who exhibit a high prevalence of vitamin D deficiency as well as higher incidence of prostate cancer and higher mortality rates from prostate cancer than Caucasians.
Our research team has recently completed an open-label clinical trial aimed at assessing the safety and potential efficacy of vitamin D3 supplementation at 4000 international units (IU) per day for one year in subjects diagnosed with early stage, low-risk prostate cancer.
The results of this clinical study suggest that supplementation with vitamin D3 at 4000IU per day may benefit patients with early stage, low-risk prostate cancer on active surveillance, because of the improved outcome (a decreased number of positive cores at repeat biopsy) in more than half of the subjects enrolled in the trial…”