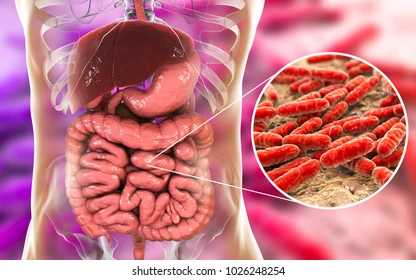
“An emerging factor that could influence not only the refractoriness of Multiple Myeloma but also a progression from asymptomatic MGUS to MM is the gut microbiome.”
First came conventional therapies such as chemo, radiation and surgery. Then came non-conventional therapies such as nutrition and supplementation. And now comes a non-conventional therapy that combines the two the gut microbiome.
Let me explain. Chemo, radiation and surgery by themselves won’t cure the newly diagnosed MM patient. The Mediterranean diet or curcumin by themselves won’t cure the NDMM patient.
According to the studies linked below, where the two therapies come together in the gut microbiome- that’s the next frontier where MM treatment happens.
It is certainly too early to use the “c” word. But we’re getting closer.
Are you a newly diagnosed MM patient? Consider treating your MM with conventional therapies, nutrition, supplementation and your gut microbiome.
Scroll down the page, post a question or a comment if you have questions. I will reply ASAP.
Thank you,
David Emerson
- Cancer Survivor
- Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
“In response to emerging discoveries, questions are mounting as to what factors are responsible for the progression of plasma cell dyscrasias and what determines responsiveness to treatment in individual patients. Recent findings have shown close interaction between the gut microbiota and multiple myeloma cells. For instance, that malignant cells shape the composition of the gut microbiota. We discuss the role of the gut microbiota in (i) the development and progression of plasma cell dyscrasias, and (ii) the response to treatment of multiple myeloma and highlight faecal microbiota transplantation as a procedure that could modify the risk of progression or sensitize refractory malignancy to immunotherapy…
Conclusions-
Despite some progress in the outcomes of treatment of MM, it remains a disease that cannot currently be cured, due to relapse or refractoriness to any available therapy. An emerging factor that could influence not only the refractoriness of MM but also a progression from asymptomatic MGUS to MM is the gut microbiota.
We see that changes in the composition of commensal bacteria can affect the process of transforming MGUS to MM. Further, these changes are associated with colonisation with opportunistic pathogens that can become an aetiological agent of complications due to infection that are associated with treatment.
Probably, in the future, it will be possible to identify patients who have an especially high risk of progression to MM, or even to modulate intestinal microflora to reduce the risk of progression of MGUS. It is also possible that the gut microbiota will be modulated to reduce complications that are due to treatment and disease, or to improve treatment outcomes. However, the field of microbiota in MM is still in its infancy and further work is required to gain a fuller understanding of the phenomena.
Importance The gut microbiome, home to the vast kingdom of diverse commensal bacteria and other microorganisms residing within the gut, was once thought to only have roles primarily centered on digestive functions. However, recent advances in sequencing technology have elucidated intricate roles of the gut microbiome in cancer development and efficacy of therapeutic response that need to be comprehensively addressed from a clinically translational angle.
Observations This review aims to highlight the current understanding of the association of the gut microbiome with the therapeutic response to immunotherapy, chemotherapy, radiotherapy, cancer surgery, and more, while also contextualizing possible synergistic strategies with the microbiome for tackling some of the most challenging tumors. It also provides insights on contemporary methods that target the microbiota and the current progression of findings being translated from bench to bedside.
Conclusions and Relevance Ultimately, the importance of gut bacteria in cancer therapy cannot be overstated in its potential for ushering in a new era of cancer treatments. With the understanding that the microbiome may play critical roles in the tumor microenvironment, holistic approaches that integrate microbiome-modulating treatments with biological, immune, cell-based, and surgical cancer therapies should be explored.
“In recent years, the consumption of over-the-counter probiotics to promote health has grown rapidly worldwide and become an independent industry. In medicine, various studies have demonstrated that probiotics can help improve the immune system and intestinal health. They are usually safe, but in some rare cases, they may cause concerning adverse reactions. Although the use of probiotics has been widely popularized in the public, the results of many probiotic clinical trials are contradictory. Particularly in cancer patients, the feasibility of probiotic management providing benefits by targeting cancer and lessening anticancer side effects requires further investigation…
Probiotics to Prevent and Treat Cancer
The results of many in vitro studies have shown that probiotics have beneficial properties in regulating proliferation and apoptosis of cancer cells (31). For example, it has been demonstrated that in mouse colon cancer HGC-27 and human colon cancer Caco-2, DLD- 1, and HT-29 cells that Lactobacillus rhamnosus GG strain inhibits proliferation and induces apoptosis (32).
These specific microbial strains can be used either alone or in combination with cancer treatment agents. The goal of treatment was achieved by activating immune surveillance against cancer (19). For example, Shi L et al. found that combined treatment with TGF-β receptor blockers and probiotics could enhance the antitumor immune response, thereby inhibiting the growth of tumors (37).
Studies have indicated that the anticancer mechanisms of probiotics primarily include positive regulation of intestinal flora, changes in metabolic activity, the binding and degradation of carcinogenic compounds, immunomodulation to improve chronic inflammation, lowering intestinal pH and the inhibition of enzymes that produce potential carcinogenic compounds (26, 38) (Figure 4). The positive role of probiotics in the treatment of tumors has been confirmed, at least in animal models (39, 40)…
Conclusions
As a dietary supplement, probiotics lack strict standards for efficacy and safety certification. Although the efficacy of several strains has been experimentally supported, the health-promoting effects of most probiotics have not been proven. Relevant publicity of probiotic products rarely mentions the potential risks.
In a number of trials evaluating the protective effects of probiotic therapy on antitumor treatment-related side effects, combined use of probiotic strains did have a positive protective effect for patients with respect to certain immune functions (47). However, for patients with severely impaired immune function, especially patients with neutropenia, careful consideration is required (87). Due to the complex pathogenesis of tumors, different patients receive different treatment options, and different strains will affect the results, so large-scale clinical trials are urgently needed.
Identifying the most beneficial strains for the prevention and treatment of different types of cancer requires a very extensive human database, and it is necessary to carefully analyze correlations between different strains and clinical responses. Once we have identified a beneficial flora for cancer prevention and treatment, the next challenge is how to use probiotics and their products to regulate patient flora.
At the same time, we can use the intestinal flora as a new cancer biomarker based on its response to changes in the pathophysiological environment. The ultimate goal is to identify specific strains or combinations of strains that can both reduce the side effects of cancer treatment and boost anticancer treatment (88)…