Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Managing Chronic Non-Cancer Pain in Cancer Survivors
Managing Chronic Non-Cancer Pain in Cancer Survivors

“…about one-third of cancer survivors (34.6%) reported having chronic pain. That is almost double the rate in the general US population.”
You have been diagnosed with cancer. You underwent FDA approved, standard-of-care (SOC) therapies such as surgery, chemotherapy and/or radiation. You’ve completed your SOC therapies and consider yourself a cancer survivor-Yay!!!. Yet you live with chronic pain. You’re reading this post to learn what you can do about your chronic non-cancer pain.
First of all, to define our situation-
Chronic non-cancer pain (CNCP) is typically defined as pain that is moderate or severe lasting six months or more, and includes conditions like low back pain, osteoarthritis, rheumatoid arthritis, neuropathic pain, fibromyalgia, and a range of other conditions.
The focus of this blog post is on the cancer survivor:
- You have completed your cancer therapies- induction, ASCT and maintenance chemo-
- According to diagnostic tests, you have little if any cancer IN YOU-
- Yet, you may have to deal with several different types of chronic pain caused by the therapies you underwent that were supposed to treat your cancer-
As a cancer survivor you are in all likelihood dealing with a number of long-term and/or late stage side effects. Pain- nerve, bone, muscle, etc. is one of the possible long-term side effects.
This post has been created in an effort to educate cancer survivors in hope of addressing my mantra “I wish I knew then what I know now.” As well as link resources and previous blog posts that will provide more information and help to you.
I think I do pretty well on the chronic pain front. Meaning, while I do deal with nerve, bone/joint, skin, and muscle pain, I think it could be a lot worse. I don’t take any opioids. I manage any/all pain through evidence-based, non-toxic, non-conventional therapies such as exercise, massage, acupuncture, CBD oil, stretching, etc.
I have been researching and writing about non-cancer pain for years. Non-cancer pain comes in all shapes and sized.
- Acupuncture- Pain, Nerve, Dry Mouth
- Chemotherapy-Induced Pain-I.D. Manage
- Radiation-Induced Pain- Dermatitis, Dysphagia, CIPN, RILP
- High-dose Cytoxan- Chemobrain, Painful Bladder-
- C-B-D for Myeloma Bone, Pain Therapy
- Alternative Options for Pain Management in Cancer Patients
- 3 Ways of Coping with Chronic Pain
- Chronic Neuropathic Pain in Women after Breast Cancer Treatment-
- Skin Cancer Pain and Itch?
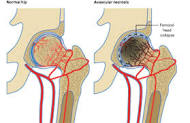
- Steroid-Induced Shoulder Avascular, Osteonecrosis: I.D. Therapies
- Fibromyalgia and CoQ10
- Hip Fracture, Osteoporosis- Bisphosphonate Therapy?
- Multiple Myeloma, Inflammation, Arthritis, Psoriasis
- Radiation-induced Plexopathy, Radiculopathy or Myelopathy?
Unfortunately, I think I’ve learned to ignore low-intensity pain. A resident in my condo building asked me if I was alright the other day. I was simply getting out of my car. I didn’t realize that I was grunting and groaning as I was standing up…ooops.
Everything I have ever learned about or experienced about cancer is that the patient or survivor must utilize the best of both conventional and evidence-based non-conventional therapies.
I have studied and blogged about chronic non-cancer pain as a long-term side effect of cancer survivors. The articles linked below are designed to address general therapies for CNCP. I have written separate posts about both chemotherapy and radiation-induced nerve pain (CIPN and RILP) as well as avascular necrosis (joint pain).
My point is, in general, when it comes to CNCP and surviving cancer, remaining in remission, preventing secondary cancers, healing other long-term side effects, etc. my practice and belief is that all cancer survivors must live a basic anti-cancer lifestyle through a clean diet, anti-inflammatory supplementation (curcumin, resveratrol, omega-3 fatty acids, etc.) and evidence-based anti-cancer lifestyle therapies such as daily, moderate exercise, whole body hyperthermia, etc.
- Learn about healing chemotherapy-induced aging- click now
- Learn about my long-term myeloma survivor experience- click now
- To Learn More about short, long-term and late stage side effects- click now
If you have any questions about CNCP, scroll down the page, post a comment and I will reply to you ASAP.
Hang in there,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Multiple Myeloma, Chronic Pain and Cure vs. Control
- Velcade/Bortezomib- CIPN, Heart, Blood, Muscle Damage
- Multiple Myeloma Side Effects- Radiation-Induced Lumbosacral Plexopathy
11 Tips for Living With Chronic Pain
- Learn deep breathing or meditation to help you relax.
- Reduce stress in your life. Stress intensifies chronic pain.
- Boost chronic pain relief with the natural endorphins from exercise.
- Cut back on alcohol, which can worsen sleep problems.
- Join a support group. Meet others living with chronic pain.
- Don’t smoke. It can worsen chronic pain.
- Track your pain level and activities every day.
- Learn biofeedback to decrease migraine and tension headache pain.
- Get a massage for chronic pain relief.
- Eat a healthy diet if you’re living with chronic pain.
- Find ways to distract yourself from pain so you enjoy life more.
Chronic Pain Management
“Chronic noncancer pain (CNCP) is a major challenge for clinicians as well as for the patients who suffer from it. The complete elimination of pain is rarely obtainable for any substantial period. Therefore, patients and clinicians should discuss treatment goals that include reducing pain, maximizing function, and improving quality of life.
The best outcomes can be achieved when chronic pain management addresses co-occurring mental disorders (e.g., depression, anxiety) and when it incorporates suitable nonpharmacologic and complementary therapies for symptom management…
- Non-Opioid Analgesics-Non-opioid pharmacological options include acetaminophen and nonsteroidal anti-inflammatory drugs (NSAIDs), as well as adjuvant medications-
- Benzodiazepines-
- Cannabinoids-
Nonpharmacological Treatments- Common nonpharmacological therapies for CNCP include:
-
Therapeutic exercise.
-
Physical therapy (PT).
-
Cognitive–behavioral therapy (CBT).
-
Complementary and alternative medicine (CAM; e.g., chiropractic therapy, massage therapy, acupuncture, mind–body therapies, relaxation strategies)…
Opioid Therapy-
Increasing incidence of chronic pain in cancer survivors
“According to one study approximately 33% of cancer patients experience long-term pain and there is research evidence linking poor pain control to adverse quality of life, after all the aim is not just to survive into bare existence.
The impact of uncontrolled pain extends far beyond suffering and disability, leading to physical, psychological and social issues. Problems such as loss of control, reduced strength and mobility, anxiety, fear and depression are common accomplices of uncontrolled pain. Increased demands placed on caregivers can adverse impact relationships…”
Effects of Pulsed Electromagnetic Field Therapy on Pain, Stiffness, Physical Function, and Quality of Life in Patients With Osteoarthritis:
“Objective: Pulsed electromagnetic field (PEMF) therapy is a potentially useful treatment for osteoarthritis (OA), but its effectiveness is still controversial…
Results: Sixteen studies were included in our systematic review, while 15 studies with complete data were included in the meta-analysis. Our primary outcome was the standardized mean difference, which was equal to the treatment effect in the PEMF group minus the treatment effect in the placebo group divided by the pooled standard deviation. For pain, the standardized mean difference was 1.06 (95% CI = 0.61 to 1.51), for stiffness 0.37 (95% CI = 0.07 to 0.67), for function 0.46 (95% CI = 0.14 to 0.78), and for QOL 1.49 (95% CI = -0.06 to 3.04). PEMF parameters did not influence symptoms.
Conclusions: Compared with placebo, there was a beneficial effect of PEMF therapy on pain, stiffness, and physical function in patients with OA. Duration of treatment may not be a critical factor in pain management. Further studies are required to confirm the effects of PEMF therapy on QOL.
Impact: Our study suggests that PEMF therapy has clinically significant effects on pain in patients with OA. The current evidence was limited to the short-term effects of PEMF therapy.”
What is BEMER Therapy and What’s It Used For?
BEMER therapy uses pulsed electromagnetic waves to stimulate the muscles and increase blood circulation…
- Chronic low back pain-
- Myofascial pain dysfunction syndrome (MPDS)
- Complex regional pain syndrome type I (CRPS-I)
- Osteoarthritis (OA)
- Fibromyalgia
- Multiple sclerosis (MS)
The use of low-dose naltrexone (LDN) as a novel anti-inflammatory treatment for chronic pain
“Conclusions- The totality of the basic and clinical research to date suggests that LDN is a promising treatment approach for chronic pain conditions thought to involve inflammatory processes. The clinical data supporting its use are very preliminary, and more research is needed before the treatment approach can be widely recommended.
Critical parameters such as dosing still need to be refined. LDN may emerge as the first of many glial cell modulators that could be used to treat chronic conditions, with more specifically targeted medications developed in the future. As conventional anti-inflammatories have poor blood brain-barrier permeability, we expect centrally active immune modulators to be an area of interest in the future…”