
Diagnosed with Cancer? Your two greatest challenges are understanding cancer and understanding possible side effects from chemo and radiation. Knowledge is Power!
Learn about conventional, complementary, and integrative therapies.
Dealing with treatment side effects? Learn about evidence-based therapies to alleviate your symptoms.
Click the orange button to the right to learn more.
- You are here:
- Home »
- Blog »
- side effects ID and prevention »
- Chemo-induced DVT aka blood clot
Chemo-induced DVT aka blood clot
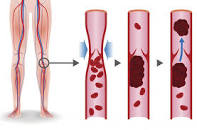
“Five to 25 percent of cancer patients (particularly those with metastatic disease) get blood clots. Not all of them go on to wreak havoc, but many do result in hospitalizations, pain and suffering, and even death..”
That means that as many as 450,000 cancer patients develop blood clots annually. Deep-vein thromboses aka DVTs seemingly appear out of nowhere. Chemo can cause blood clots. Cancer can cause blood clots. Sitting can cause blood clots.
Make no mistake. Blood clots are complicated, sneaky and can kill. As one of the blog posts linked and excerpted below explains, conventional therapies such as blood thinning drugs don’t always prevent blood clots. And blood thinning therapies come with side effects of their own.
- According to research, more than 10 million people worldwide are diagnosed with a blood clot annually.
- Having a deep vein thrombosis, DVT, blood clot, increases the risk of a second DVT.
So what is a person to do? While I’m not a board certified medical doctor and therefore can’t prescribe medicine, I can tell you what I do, how I have remained free from deep vein thromboses since I developed my own chemotherapy-induced DVT in 1995.
Let me be clear. Conventional therapies such as coumadin, Xarelto, Pradaxa, Eliquis, etc. are the standard-of-care to prevent a DVT. I am saying that coumadin caused side effects from me and short, long-term and late stage side effects need to be clearly understood.
When I developed my second DVT in 1999, the M.D. prescribed the standard-of-care therapy at the time- coumadin. I tried coumadin for a few months. I experienced fatigue and gained a few pounds. I went online to research possible side effects of this SOC therapy.
I didn’t like what I found and stopped taking coumadin. I now take the therapies listed below and haven’t had a DVT since.
Let me be clear. Conventional blood thinning therapies have their place in the prevention and management of DVT’s. However, my experience and research has shown me that evidence-based, non-toxic, non-conventional blood thinning therapies can be a better option for you.
Benefit of chemotherapy?
Was the benefit of my chemo worth my blood clots? Does chemotherapy help cancer patients? Is the cure worse than the disease? I’m not going to tackle that debate in this blog post certainly. But I will say that each and every chemotherapy I underwent from my original diagnosis through my oncologist telling me “we can do nothing more for you” should have been treated with one or more prophylactic therapies to reduce my risk of a blood clot.
Alternatives to chemotherapy?
Again, this is too big, too complicated a question to be debated in this blog post. In the case of this post, DVTs, blood clots, the issue is prevention and prophylactics.
Therapies to heal or prevent chemotherapy-induced deep vein thrombosis?
- Nattokinase-
- Omega-3 Fatty Acids
- Curcumin-
- Lifestyle therapies such as exercise, hydration, diet-
- etc.
Chemotherapy and radiation have saddled me with serious long-term and late stage side effects such as post-thrombosis syndrome as well as an increased risk of a future blood clot. My view is to work to prevent any and all health problems from these long-term and late stage side effects.
I have been researching and writing about blood clots for years.
- Cardiac Rehabilitation-Curcumin, Cardiovascular Disease, Heart Failure
- Multiple Myeloma Symptom, Side Effect, COD- Hyperviscosity, Blood Clots
- Stroke Prevention Diet and Supplementation
- Hospitalized for Heart Failure, Stroke? Reduce Blood Clot (VTE) Risk-
- Xarelto Lawsuit Highlights Risks of Conventional Blood Thinners
- VTE Blood Clot Treatment Dissatisfaction
- Multiple Myeloma Side Effects-PostThrombotic Syndrome
- 80% of Pediatric Cancer Survivors Suffer Chemo-Induced Heart, Brain, Joint Damage
- Lung Cancer Patients at Risk for VTE and Early Mortality-
- Low Vitamin D Levels in Stroke Patients Up Risk of DVT
- Omega-3 Fatty Acids- A Long-Term Multiple Myeloma Survivor’s Best Friend-
- Cardiac Rehab-Lower Blood Pressure-Nattokinase- Non-toxic, Inexpensive Therapy
- Multiple Sclerosis and your risk of Blood Clots
If you have ever had a deep-vein thrombosis/DVT/bloot clot, you live with an increased risk of having another blood clot. Scroll down the page, post a question or a comment and I will reply to you ASAP.
- Learn about healing chemotherapy-induced aging- click now
- Learn about my long-term myeloma survivor experience- click now
- To Learn More about short, long-term and late stage side effects- click now
Thanks,
David Emerson
- MM Survivor
- MM Cancer Coach
- Director PeopleBeatingCancer
Recommended Reading:
- Cancer Coaching Testimonials- PeopleBeatingCancer
- Long-Term Multiple Myeloma Survivor- If I Knew Then What I Know Now
- Heart Failure- Chemo-Induced Afib, Hi BP, DVT
Prevention of Blood Clots During Chemotherapy
“In fact, compared to the well-known symptoms of nausea, fatigue, and hair loss, (blood clots) can be much more dangerous…
Blood clots: What cancer patients need to know
“Five to 25 percent of cancer patients (particularly those with metastatic disease) get blood clots. Not all of them go on to wreak havoc, but many do result in hospitalizations, pain and suffering, and even death, as well as, of course, high health care costs. A 2018 study found cancer patients who developed a venous thromboembolism, or VTE, while hospitalized had an average cost of $37,352, with an average length of stay of more than 12 days, compared to patients without VTEs who had average costs of $19,994 and spent about a week in the hospital.
They’re common, they’re scary, they’re potentially lethal and they’re pricey — yet they’re not always on the radar of patients or clinicians…”

